To integrate appropriate nutritional recommendations for patient management, a two-step process is undertaken: a nutritional assessment phase (based on the Circle of Nutrition by the American College of Veterinary Nutrition; http://www.acvn.org) and an analysis, interpretation, and action phase.1 In the assessment phase three sets of factors are assessed: animal-specific factors, diet-specific factors, and feeding management and environmental factors.2 Animal-specific factors include age, physiologic status, disease processes, and activity of the patient. Diet-specific factors include safety and appropriateness of diet fed and nutrients of interest. Feeding factors include frequency, timing, location, and method of feeding, and environmental factors include living space and quality of the patient’s surroundings.1 An important part of the assessment phase is obtaining body weight, body condition score, and muscle condition score.1 Body condition score evaluates body fat (Figure 15-1).3–5 The goal for most patients is a body condition of 2.5 to 3.0 out of 5 or a 4 to 5 out of 9, which is associated with decreased health problems, including musculoskeletal conditions.6–10 Muscle condition score evaluates muscle mass, which can be independent from body fat content assessed by body condition score (Figure 15-2).11 Evaluation of muscle mass includes visual examination and palpation over temporal bones, scapulae, lumbar vertebrae, and pelvic bones. Muscle loss adversely affects strength, immune function, and wound healing. After collecting information from the assessment phase information is analyzed and interpreted and an action plan is implemented. After implementation of the action plan the patient undergoes repeated assessment and adjustment of the plan. Nutrition interacts with musculoskeletal disease. The prevalence of musculoskeletal disorders for all dogs at multicenter referral practices has been reported to be approximately one in four.12 In dogs less than 1 year of age the prevalence is 22%, with 20% of these possibly having a nutrition-related cause.13 We focus on two specific common conditions. The role of nutrition in the development of musculoskeletal disease in growing dogs has been recognized for decades. Developmental orthopedic disease refers to a group of skeletal abnormalities (e.g., osteochondritis dissecans, hip dysplasia, wobblers’ syndrome, ligamentous laxity, and hypertrophic osteodystrophy) that affect primarily rapidly growing, large- and giant-breed dogs. Nutrient excess (calcium and energy) and rapid growth (overfeeding and excess energy) are known risk factors for developmental orthopedic disease in dogs that have genetic risk.14–18 Restricting food intake during growth slows growth rate without significantly reducing adult body size and is associated with decreased incidence of developmental orthopedic disease.8,19 Dietary calcium greater than 3% on a dry matter basis is associated with increased risk despite an appropriate calcium-to-phosphorus ratio.15 Even if the diet contains less calcium than this, excess calcium intake can occur if owners provide supplemental calcium. For example, two level teaspoons of calcium carbonate added to a growth diet fed to a 15-week-old Rottweiler puppy doubles the calcium intake. For large- and giant-breed dogs during growth, recommended dietary composition includes the following20: • Energy: 3.2 to 4.1 kcal/kg of diet (lower end of range if at risk for developmental orthopedic disease or if clients use free-choice feeding) • Crude fat: 8.5% to 11% on a dry matter basis • Docosahexaenoic acid: ≥0.02% on a dry matter basis • Protein: ≥27% on a dry matter basis • Calcium: 0.8% to 1.2% (≤3% on a dry matter basis) with a calcium-to-phosphorus ratio of 1.1 to 2.0 : 1.0 The risk of developmental orthopedic disease is reduced if clients use limited meal-feeding rather than free-choice feeding and if growth rate is limited during the postweaning period.21 Obesity may contribute to the development and progression of osteoarthritis because of excess forces placed on joints and articular cartilage, which may lead to inactivity and further development of obesity. Thus a vicious cycle ensues. Additionally adipose tissue is recognized as being metabolically active and proinflammatory; therefore obesity may contribute to inflammation.22–26 Several studies have demonstrated a relationship between obesity and osteoarthritis9; however, a cause and effect has not been determined.27,28 A long-term study was performed of 48 Labrador retrievers from seven litters divided into two dietary groups. One group was fed an adult maintenance dog food at 0.27 kJ of metabolizable energy per kilogram of body weight per day, and the second group was fed the same diet at 75% of the amount (0.20 kJ of metabolizable energy per kilogram of body weight per day).8,29 Restricted fed dogs lived on average 1.8 years longer, weighed less, had better body condition scores, and had longer delay to treatment of chronic disease including osteoarthritis.21 In addition the restricted fed group had a lower incidence of osteoarthritis in most major joints, and if it occurred, it was less severe. Maintaining optimal or slightly lean body condition may be associated with lower risk of developing osteoarthritis, development of less severe osteoarthritis if osteoarthritis occurs, and delay of onset of clinical signs of osteoarthritis in dogs. Patients undergoing surgery that are healthy and in optimal body and muscle condition (see Figures 15-1 and 15-2) require no further intervention nutritionally other than to continue feeding the current diet at the same amount and frequency. Patients are not fed 8 to 12 hours before anesthesia and surgery, but can resume normal feeding patterns once recovered from the procedure. It may be necessary to add flavoring agents or feed a different diet to stimulate appetite in the postoperative period. Patients should be assessed daily following surgery to insure they are eating adequately and that no adverse events occur either from the procedure or from postoperative medications such as analgesics and sedatives. Energy requirements during hospitalization and in the immediate postoperative period when activity is restricted is estimated in most patients to be the resting energy requirement (RER).30,31 Although both equations are used to estimate RER, the authors prefer the second equation because body weight and RER are not linearly related as estimated with the first equation. As the patient becomes more active or as a rehabilitation program is initiated, energy requirements increase (see Nutrition and Rehabilitation). In many instances surgery in these patients is elective; therefore, depending on the urgency of the surgical procedure, consideration should be given to weight reduction before surgery in patients that are obese (see Obesity). Reducing body weight to the optimal weight decreases anesthetic risk, improves immune function, and allows patients to more easily undergo postsurgical physical rehabilitation.32 Patients with surgical musculoskeletal disease associated with trauma may or may not have increased nutritional requirements depending on the degree of trauma. If the trauma is less severe, then energy requirements are similar to nontraumatized surgical patients, and energy requirements approximate resting energy requirements.30,33 Energy requirements are determined by estimating RER as stated.30,31 Severely injured patients or those with closed head injuries typically have energy requirements exceeding resting energy requirements because of the extent of the injuries or activation of the sympathetic nervous system, in part.34 In these patients energy requirements may exceed two times the estimated resting energy requirements.30,31 Likewise protein requirements may exceed that required for maintenance to facilitate recovery, immune function, and wound healing.35,36 Recommended protein intake for adult dogs at maintenance is 2.62 to 3.28 g/BWkg0.75 and for adult cats is 3.97 to 5.90 g/BWkg0.75.37 With trauma or strenuous exercise, protein requirements may exceed these by 50% to 100%. Some patients may require facilitated nutritional support enterally or parenterally.30,38–44 Nutritional support in these patients should be individualized and intensive monitoring is required to maximize recovery and response to supportive care. Convalescent diets are available that are formulated to contain higher levels of protein and fat are more calorically dense, highly palatable, and have a homogeneous texture suitable for feeding tubes. Water is the most essential nutrient. It is the transport medium for nutrients, heat, and waste products. Total body water is divided into four compartments with 64% being intracellular, 22% in interstitial spaces, 7% in plasma, and the remaining 7% transcellular.45 Total body water is determined by total water intake and metabolic water production minus evaporation, urine, and fecal losses. An increase in muscle activity results in an increased demand for nutrients and removal of waste products. Only 20% to 30% of energy consumed by muscle tissue produces actual work, with the remaining 70% to 80% resulting in heat.45 Increased blood flow during exercise dissipates this heat. Increases in body heat during exercise must be removed because increases not only limit work, but also damage tissues. During rehabilitation, excitement, fear, pain, and other stress factors affect the simplest of nutritional needs, water and electrolytes. These stress factors can increase body temperature and respiration alone or during exercise. It is important to monitor hydration and electrolyte balance during the program. A study of sprinting and endurance racing dogs showed water intake can directly affect biochemical and red blood cell profiles.46 The same study showed increased blood cortisol and decreased blood glucose in sprint-racing sled dogs. These changes were attributed to metabolic stress and the physiologic response to high-intensity exercise.46 High-intensity exercise is not commonly used in a rehabilitation setting, but the summation of patient stress, new exercise level, and perhaps changes in water and food intake should be noted. Patients boarded for continuous rehabilitation may have poor diet and water intake in an unfamiliar environment.45 Water and food intake should be recorded for hospitalized patients. Owners of outpatient dogs should be questioned about food intake, water intake, and other nutritional changes they may have noted during the program. Water intake for healthy dogs approximates 50 to 60 mL/kg per day, but may be more with rehabilitation. Energy is a primary nutrient for maintenance, stage of life, and the therapy program. Diet supplies energy from carbohydrate, fat, and protein. Fats and carbohydrates are preferred substrates for exercise, whereas protein provides structural and functional tissue. Energy requirements correlate to work intensity, duration, and frequency, with intensity being the primary determinant. Studies show that sprinters depend on carbohydrates, whereas endurance activities use fat stores. Sprinters such as greyhounds that are running with maximum intensity have low energy requirements because of the short race duration and low frequency of training.47 These dogs mainly use carbohydrates to meet energy requirements. Studies of endurance sled dogs with long durations of work are at the other extreme, requiring high energy intake. High-fat diets are fed to meet these high-energy requirements.45,47,48 Exercise intensity has not been quantified in rehabilitation, unlike performance and working dogs. Therapy is likely an intermediate level of exercise, which has not been well defined. Intensity, duration, and frequency of exercise are highly variable; therefore it is difficult to predict the energy needs of these patients. Consideration of historical exercise level combined with current patient and diet assessment may provide some insight into energy needs. A house pet with a body condition score (BCS) of 4 to 6/9 (see Figure 15-1), which usually has low energy requirements, that begins a rigorous short duration, increasing intensity, daily program, may need energy intake adjustment during rehabilitation. The dog’s daily energy requirement (DER) is based on the resting energy requirement (RER) multiplied by a factor for life stage or disease. Resting energy requirements are estimated as described in the preceding equations and defined as the energy requirement (kcal/day; 1 kcal = 4.184 kJ) for a healthy but fed animal at rest in a thermoneutral environment.31 Maintenance, exercise, and life stage (growth, gestation, and lactation) are combined to develop factors of RER to estimate a patient’s DER. Life stage factors commonly used in clinical nutrition are as follows49: These life stage factors are guidelines. Variables such as breed, disease, environment, and age can greatly affect energy requirements. In rehabilitation, energy required to participate in a therapy program affects DER. If the therapist defines the treatment plan as work, then intensity, duration, and frequency of exercises are factored into the DER. Studies show sprinting greyhounds can have a DER of 1.6 to 2 × RER, whereas endurance sled dogs may require greater than 5 × RER.47 This comparison is useful because there are nutritional studies of racing greyhounds that may apply to a rehabilitation program. Assigning an exercise factor to common physical rehabilitation programs would be useful in calculating the dog’s DER. Until such data are provided it is important to recall that most house dogs have less than light exercise and may be obese or obese prone; therefore it is prudent to use low end exercise factors initially. Fat provides the most calories in dog foods at 8.5 kcal/g of dry matter diet. Carbohydrates and protein supply 3.5 kcal/g of dry matter in a diet. To increase the energy density of a commercial diet, the fat content of the diet is increased. Fat also increases palatability of diets. Studies of endurance sled dogs show a positive effect for higher fat diets regarding performance. Sled dogs have been known to consume 80% of their caloric needs from fat.45 In a study of well-conditioned beagles running on a treadmill, time to exhaustion correlated with fat intake, diet digestibility, and energy concentration of the diet.50 Increasing fat intake improves performance of dogs with extreme energy requirements. In rehabilitation therapy, the level of exercise is unlikely to equate to the extreme energy requirements of sled dogs. Fat intake still should be considered when a patient is in therapy, however. If we use the example of a sprinting greyhound, dogs in therapy may have similar fat requirements with fat providing 20% to 30% of the total energy requirement. This equates to a diet with a fat content of 8% to 10% on a dry matter basis.45 Stress factors of a new environment, exercise, fatigue, surgery, and illness may decrease diet intake. If there is appetite suppression, a higher-fat diet, which has a higher energy concentration and increased palatability, can be used to increase voluntary intake. Some dogs losing weight during a program are on diets too low in fat and energy concentration to meet the energy requirements of the rehabilitation program. The diet can be changed to a higher-fat diet with increased energy concentration to meet energy requirements. The type of fat in the diet should be evaluated. Diets must contain essential fatty acids in the form of unsaturated fatty acids. Linoleic acid, a 20-carbon n-6 fatty acid, is required in a dog’s diet. N-3 fatty acid utilization is an area of extensive research in both humans and dogs and is discussed in a later section. Carbohydrates are required only during gestation because dogs readily maintain normal blood glucose and tissue glycogen on a no-carbohydrate diet.45 However, dogs can readily use carbohydrates for energy and most pet foods contain 40% to 60% carbohydrates on a dry matter basis. Racing greyhounds depend on carbohydrates that are metabolized into muscle glycogen. Muscle glycogen is a readily available source of energy for these sprinters with utilization of 70% of muscle stores in a single race. In humans, rats, and horses, increasing muscle glycogen improves exercise performance.51,52 It is unknown whether increased carbohydrate intake in dogs enhances exercise performance or increases muscle glycogen stores. Studies have mixed results evaluating carbohydrate loading in racing greyhounds.45,53 Extrapolation from human data suggests that 50% to 70% of total energy intake should be fed to maintain muscle glycogen stores for sprinting.45 This is because anaerobic metabolism of glucose and glycogen is the dominant energy pathway that produces energy for sprinting. Because of the intensity of work and immediate energy needs for the racing greyhound, this extrapolation is logical, and these dogs are generally fed carbohydrates at a level that meets 50% or greater of the energy requirements. In physical rehabilitation, exercises are unlikely to have the intensity of work that is necessary to have an absolute carbohydrate requirement to employ anaerobic metabolism pathways. Carbohydrate intake using commercial dog foods appears reasonable. In a postabsorptive state, protein that has been broken down to amino acids provides the substrate for protein synthesis elsewhere in the body. Exercise increases protein synthesis and breakdown with the net result of decreased muscle protein. Ingestion of amino acids stimulates muscle protein synthesis, exceeding the rate of breakdown, and muscle mass increases. In one study of elderly humans, patients maintained on bed rest for 10 days were given a dietary supplement of amino acids or placebo in a double-blind randomized fashion.54 Supplementing essential amino acids in these individuals with absolute bed rest prevented decreases in muscle strength and function. Furthermore amino acid supplementation prevented the decreased rate of muscle synthesis that is normally seen with bed rest.54 Amino acid stimulation of muscle protein synthesis and exercise is synergistic. Exercise combined with amino acid intake produces a greater response regarding muscle synthesis than response to individual treatments. This suggests exercise can prime the muscle response to the anabolic effects of amino acids or exercise activates muscle synthesis, but adequate amino acid precursors are needed to increase muscle mass. Postexercise supplementation with carbohydrate and protein or protein hydrolysate increases muscle glycogen stores and may facilitate recovery.55–57 The effect of amino acid supplementation via infusion on muscle proteolysis in beagles was found to require concomitant glucose infusion; therefore an energy substrate for protein anabolism is required for the desired beneficial effect.58 Branched chain amino acids (leucine, isoleucine, and valine) supplementation decreases branched chain amino acid catabolism and exercise-induced muscle damage promoting muscle protein synthesis in humans59–61; however, results are contradictory and branched chain amino acids may only facilitate recovery of muscle following exercise.62 Alanine supplementation improves high-intensity aerobic performance of muscle.63 Carnitine is a quaternary ammonium compound biosynthesized from lysine and methionine and is a cofactor for transport of long-chain fatty acids across the mitochondrial membrane to liberate energy via β oxidation. In dogs, it has been shown to improve function and energy metabolism in muscle and may be useful in rehabilitation.64,65 However glutamine supplementation does not appear to be beneficial in preventing muscle protein catabolism with exercise.66 Weight reduction from an obese state is beneficial in the management of osteoarthritis in humans.67–69 In addition to improvement in mobility, weight reduction was associated with better quality of life scores in humans with knee osteoarthritis.70 Three uncontrolled clinical studies of obese dogs with osteoarthritis demonstrated improvement in mobility.71,72 In one study of nine dogs with body condition score of 5 out of 5 and coxofemoral osteoarthritis, obesity management resulted in loss of 11% to 18% of body weight, a decrease in body condition to optimal, and improvement in severity of subjective hind limb lameness scores.71 In the second study of 16 dogs with coxofemoral osteoarthritis, weight loss of 13% to 29% of body weight and decrease of body condition to optimal resulted in improvement of ground reactive forces as well as improvement in subjective mobility and clinical signs of osteoarthritis.72 In the third study, 14 client-owned dogs with clinical and radiographic signs of osteoarthritis participated in an open prospective clinical trial. Results indicated that body weight reduction caused a significant decrease in lameness with a weight loss of 6.10% or more. Kinetic gait analysis supported the results with a body weight reduction of 8.85% or more. These results confirm that weight loss should be presented as an important treatment modality to owners of obese dogs with osteoarthritis, and that noticeable improvement may be seen after modest weight loss of 6.10% to 8.85% body weight. Although these are uncontrolled clinical trials of a small number of dogs, results suggest that weight reduction may be beneficial in dogs with osteoarthritis. Weight loss is beneficial when used in combination with physical rehabilitation in dogs. In a non-blinded prospective randomized clinical trial, 29 adult dogs that were overweight or obese (body condition score of 4/5 or 5/5) having clinical and radiographic signs of osteoarthritis were evaluated.73 All dogs underwent weight loss. One group received caloric restriction and a home-based physical rehabilitation program and the other group received an identical dietetic protocol and an intensive physical rehabilitation program, including transcutaneous electrical nerve stimulation. Significant weight loss and improved mobility were achieved in both groups; however, greater weight reduction and better mobility was obtained in the group receiving intensive physical rehabilitation.73 There are other dietary supplements recommended for patients with osteoarthritis.74–87 Very few have been evaluated in a controlled manner and even fewer have been evaluated in dogs with osteoarthritis. Formation of free radicals as a consequence of cellular metabolism occurs constantly, but potential deleterious effects are minimized by antioxidants. Balance between free radicals and antioxidant defenses is an essential factor in preventing development of noxious processes at cellular and tissue levels. Recent evidence supports the theory that excessive production of free radicals or the imbalance between concentrations of free radicals and antioxidant defenses may be related to processes such as aging, cancer, diabetes mellitus, lupus, and arthritis.88 Progressive hypoxia resulting in production of reactive oxygen species may play a role in rheumatoid arthritis.89 Thus antioxidant therapy may be of benefit in the treatment of osteoarthritis.90 S-adenosylmethionine (SAMe) is a co-substrate involved in transmethylation, transsulfuration, and aminopropylation reactions, which occur primarily in the liver. In controlled trials of humans with osteoarthritis, SAMe was as effective as nonsteroidal antiinflammatory drugs (NSAIDs) and better than placebo in reducing pain and improving function with a lower likelihood of side effects91–98; however, no difference with an NSAID drug was found in one study.99 A systematic review was inconclusive and evidence of efficacy was hampered by inclusion of small trials of questionable quality.100 A double-blinded, placebo-controlled clinical trial of 33 dogs with presumed osteoarthritis did not show a benefit of SAMe as a sole treatment.101 An in vitro study showed SAMe adversely affected chondrocyte viability.102 SAMe may reduce inflammatory mediators, increase levels of the antioxidant glutathione, increase cartilage synthesis, be chondroprotective, and maintain DNA methylation.103 Most studies of antioxidant therapy for arthritis in humans involve rheumatoid arthritis, although several studies of knee osteoarthritis have been published. An early pilot study of vitamin E (tocopherols) demonstrated improvement in clinical signs and pain scores in 52% of 29 patients with knee osteoarthritis compared with 4% receiving placebo.104 In another placebo-controlled study of humans with osteoarthritis of coxofemoral or knee joints, high-dose tocopherols was as efficacious as diclofenac in reducing pain and improving mobility.105 This was also found in studies of humans with rheumatoid arthritis.106,107 Other studies have not demonstrated a benefit of vitamin E for either rheumatoid arthritis or osteoarthritis.108–110 Vitamin E has not been evaluated in dogs with osteoarthritis; however, large breed puppies fed a diet proportionately higher in protein, calcium, n-3 fatty acids, and antioxidants had increased lean body mass and improved cartilage turnover as maturity was attained.111 In greyhounds and sled dogs, supplementation is associated with increased plasma levels; however, no difference in muscle damage with exercise has been noted.112–114 Efficacy of vitamin C in humans with osteoarthritis has been difficult to determine due to contradictory results.115–118 In dogs, vitamin C administration was found to increase vitamin C plasma levels, but was associated with decreased racing performance in greyhounds.119 Selenium was not shown to be beneficial in humans with rheumatoid arthritis.120 An antioxidant cocktail was administered for 6 weeks to 48 dogs. Dogs were assigned to four groups: untrained/not supplemented, untrained/supplemented, trained/not supplemented, and trained/supplemented. Metabolomic profiling showed that dogs receiving the antioxidant cocktail recovered to baseline values 24 hours after exercise, whereas dogs receiving no supplementation did not. Therefore administration of an antioxidant cocktail apparently facilitates recovery from exercise.121 Avocado/soybean unsaponifiables (ASUs) are composed of the unsaponifiable fractions of avocado and soybean oils in a one-third to two-thirds proportion.122,123 Avocado/soybean unsaponifiables have anti-osteoarthritic properties by inhibiting interlukin-1 and stimulating collagen synthesis in cartilage cultures.123–125 In vivo there is one report in an ovine meniscectomy model of osteoarthritis that supports disease-modifying capabilities.125,126 Human clinical trials have shown some beneficial effects of ASUs on clinical symptoms of osteoarthritis and they may have some structure modification capabilities.127–129 However there are conflicting data as other studies found no long-term benefits.128,130–132 In one study of dogs, osteoarthritis was induced by anterior cruciate ligament transection that then received placebo or ASUs (10 mg/kg per 24 hours).133 The size of macroscopic lesions of the tibial plateau, severity of cartilage lesions, synovial cellular infiltration, and inducible nitric oxide synthase were decreased significantly and there was reduced loss of subchondral bone volume and calcified cartilage thickness in the group receiving ASUs.133 Blueberries are flowering plants of the genus Vaccinium, which includes cranberries and bilberries. They may have antioxidative and antiinflammatory actions because they contain pterostilbene, anthocyanins, proanthocyanidins, resveratrol, flavonols, and tannins.134 In a study of sled dogs, those receiving a blueberry supplement had higher antioxidant status than those not receiving the supplement; however, there was no difference in creatinine kinase activity and isoprostane levels (a measure of oxidative stress) in dogs receiving blueberries and those that did not.135 Boswellia, also known as Boswellin or Indian frankincense, comes from the Indian Boswellia serrata tree. Resin from the bark of this tree is purported to have antiinflammatory properties derived primarily from 3-O-acetyl-11-keto-β-boswellic acid (AKBA), which inhibits 5-lipoxygenase and matrix metalloproteinases, and decreases tumor necrosis factor α and interleukin 1β.136,137 Following oral administration, AKBA has poor bioavailability. However, two AKBA-containing compounds, Alfapin and 5-Loxin, have good bioavailability.138 Boswellia resin has been shown to improve clinical signs and pain in humans in controlled studies.139–141 Boswellia resin has been evaluated in 24 dogs in an open multicenter study.142 Improvement in clinical signs, lameness, and pain was found in 17 of 24 dogs. Diarrhea and flatulence occurred in five dogs. Chondromodulating agents are purported to slow or alter the progression of osteoarthritis. These agents are considered to be slow-acting drugs in osteoarthritis (SADOA) and can be subdivided into symptomatic slow-acting drugs (SYSADOA) and disease-modifying osteoarthritis drugs (DMOAD). Beneficial effects may include a positive effect on cartilage matrix synthesis and hyaluronan synthesis by synovial membrane, as well as an inhibitory effect on catabolic enzymes in osteoarthritis joints.143 Compounds fall under two different categories. One group includes agents that are approved by the US Food and Drug Administration, such as polysulfated glycosaminoglycan, which can have label claims of clinical effects. The second group includes products that are considered to be nutritional supplements, which are not required to undergo efficacy testing, and legally cannot claim any medical benefits. Examples of this group include glucosamine and chondroitin sulfate. Although many of these products are administered as a supplement or alternative treatment, some, such as glucosamine and green-lipped mussels, are incorporated into pet foods. Glucosamine is an amino sugar that is a precursor for biochemical synthesis of glycosylated proteins and lipids. D-glucosamine is made naturally in the form of glucosamine-6-phosphate and is the biochemical precursor of nitrogen-containing sugars.144 Specifically glucosamine-6-phosphate is synthesized from fructose-6-phosphate and glutamine145 as the first step of the hexosamine biosynthesis pathway. The end product of this pathway is UDP-N-acetylglucosamine, which is used for making glycosaminoglycans, proteoglycans, and glycolipids. Because glucosamine is a precursor for glycosaminoglycans, and glycosaminoglycans are a major component of joint cartilage, supplemental glucosamine may help enhance cartilage synthesis and there are in vitro and clinical data to support this claim, although in vitro studies often use concentrations not achieved in serum or plasma after oral administration.146–152 There are conflicting data on evidence of clinical effect of glucosamine-chondroitin in osteoarthritis.74,75,153–161 In a randomized, double-blind, positive-controlled clinical trial comparing glucosamine hydrochloride and chondroitin sulfate to carprofen in 35 dogs with osteoarthritis, carprofen-treated dogs had improvement in five subjective measures, whereas dogs treated with glucosamine-chondroitin sulfate had improvement in three of five measures, but only at the final assessment point of 70 days.162 A 60-day prospective, randomized, double-blinded, placebo-controlled trial of 71 dogs with osteoarthritis assessed subjective and objective measures comparing carprofen, meloxicam, glucosamine-chondroitin, and placebo. Results indicated that objectively measured variables improved significantly with carprofen and meloxicam, but not with glucosamine-chondroitin or placebo. Subjective findings of veterinarians agreed with results of objective evaluation, but subjective assessment by owners identified improvement only with meloxicam.163 Based on these results there is weak clinical evidence of benefit of glucosamine-chondroitin in dogs with osteoarthritis.153–155 The New Zealand green-lipped mussel (Perna canaliculus) is a rich source of glycosaminoglycans, although its proposed benefit is thought to be from its antiinflammatory effects.164 In 1986 dried mussel extracts became available that were stabilized with a preservative. The earlier studies that found no beneficial effect of the green-lipped mussel on arthritis used preparations that had not been stabilized, a point that may help explain some of the discrepancies in the research. A stabilized lipid extract is more effective than a nonstabilized extract at inhibiting inflammation.165 In an uncontrolled clinical trial stabilized lipid extract administration resulted in an 80% improvement in humans with rheumatoid arthritis.166 In a randomized controlled clinical study of 31 dogs with arthritis, green-lipped mussel powder (0.3%) was added to the diet during processing for one group of dogs.167 Compared with the control group, which was fed the same diet without added green-lipped mussel powder, there were significant improvements in subjective arthritis scores, joint swelling, and joint pain in the treated group. However, these data must not be overinterpreted. In a randomized, double-controlled and double-blinded clinical trial, 45 dogs with osteoarthritis were evaluated. Dogs receiving green-lipped mussels had improved mobility when compared with placebo; however, it was not as effective as carprofen.168 In a study of 81 dogs with presumptive osteoarthritis, clinical signs improved in both the green-lipped mussel and placebo-treated groups when compared with baseline. On day 56 of the study, dogs receiving green-lipped muscle had improved clinical signs but not musculoskeletal scores.169 An uncontrolled study of 85 dogs that were fed a green-lipped mussel supplemented diet for 50 days showed reduction of a composite arthritic score when compared with baseline scores on various diets dogs were consuming.170 In systematic reviews of agents used to treat canine osteoarthritis, the data regarding the benefits of green-lipped mussel extract in dogs were promising but uncertainties existed relating to the scientific quality of the data and no definitive relationship has been proved between clinical improvements and the therapy.154,155 Degenerative osteoarthritis involves an inflammatory component. Thus, it may be possible to modify the inflammation by nutritional components, specifically omega-3 (n-3) fatty acids. Arachidonic acid (an n-6 fatty acid) is incorporated into cell membranes, and when metabolized, it yields prostaglandins, leukotrienes, and thromboxanes of the two and four series. Many drugs used to treat degenerative osteoarthritis inhibit conversion of arachidonic acid to these eicosanoids. These n-6-derived eicosanoids have, for the most part, vasoactive and proinflammatory effects. Substituting an n-3 fatty acid in the membrane may decrease these responses. Metabolism of n-3 fatty acids results in eicosanoids of the three and five series, which are less vasoactive and less proinflammatory. In addition to modulating cytokines, n-3 fatty acids have been shown to reduce expression of cyclooxygenase-2, lipoxygenase-5, aggrecanase, matrix metalloproteinase 3 and 13, interleukin-1α and β, and tumor necrosis factor α.171–175 In addition to these effects, novel oxygenated products generated from n-3 fatty acids, eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) have been identified in resolving inflammatory exudates and tissues and are called Resolvins (resolution phase interaction products) and docosatrienes.176–178 They may have a role in inflammatory diseases such as osteoarthritis.179–184 Several studies have demonstrated a beneficial response to n-3 fatty acid incorporation into diets of humans with rheumatoid arthritis,185–189 although other studies have not demonstrated a benefit.190 There is a growing body of data showing positive effects of n-3 fatty acids on cartilage and its metabolism in the face of degradative enzymes; n-3 fatty acid supplementation can reduce inflammatory and matrix degradative responses elicited by chondrocytes during osteoarthritis progression.172–174,191 Eicosapentaenoic acid appears to be more effective than DHA and α-linolenic acid.171 An unpublished study was performed in dogs evaluating omega-3 fatty acids and experimentally induced stifle arthritis.192,193 Eighteen dogs were randomly assigned to one of three isocaloric diet groups containing 21.4% fat (dry matter basis) differing only in their fatty acid composition: a diet with an n-6 to n-3 fatty acid ratio of 28.0 : 1.0 (high n-6 diet), a diet with an n-6 to n-3 fatty acid ratio of 8.7 : 1.0 (control diet), and a diet with an n-6 to n-3 fatty acid ratio of 0.7 : 1.0 (high n-3 diet). Diets were fed for a total of 21 months. Dogs were begun on their assigned diet 3 months before surgical transection of the left cranial cruciate ligament, then continued until surgical repair 6 months later, and were maintained for an additional 12 months following repair. When compared with the high n-6 and control diets, consumption of the high n-3 diet was associated with lower serum concentrations of cholesterol, triglycerides, and phospholipids, lower synovial concentration of prostaglandin E2, better ground reaction forces, and less radiographic changes of osteoarthritis. Synovial membrane fatty acid composition mirrored the fatty acid composition of the diets consumed by the dogs. Another study in dogs reported results of owner observations who perceived improvement in their pet’s arthritic signs when treated with fatty acids for various dermatologic problems.194 In a study of 127 dogs with osteoarthritis, dogs fed a diet with a 31-fold increase in total n-3 fatty acid content and a 34-fold decrease in n-6 to n-3 fatty acid ratio for 6 months had improved ability to rise from a resting position and play when compared with dogs fed a control diet.195 In a randomized, double-blinded, controlled clinical trial of 38 dogs with osteoarthritis, dogs fed a diet containing 3.5% n-3 fatty acids for 90 days had improved peak vertical force values and subjective improvement in lameness and weight bearing when compared with a control diet.196 Another randomized, controlled clinical trial was performed with 131 dogs with stable chronic osteoarthritis treated with carprofen. Over a 12-week study carprofen dosage decreased significantly faster in dogs fed a diet supplemented with n-3 fatty acids when compared with a control diet.197 Based on results of these studies there is a rationale for n-3 fatty acid supplementation or feeding diets containing increased n-3 fatty acid levels to dogs with osteoarthritis.
The Role of Chondroprotectants, Nutraceuticals, and Nutrition in Rehabilitation
Nutritional Plan
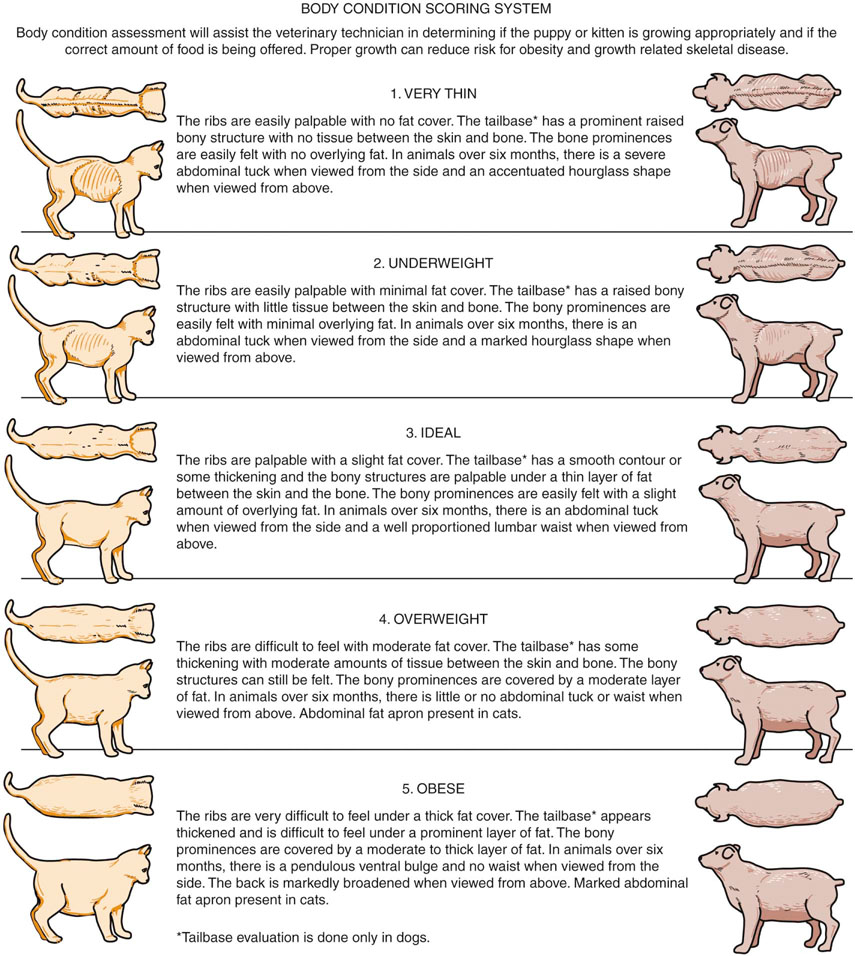
Figure 15-1 Body condition scoring (BCS) systems for the dog and the cat. (From Bassert JM, McCurnin DM: McCurnin’s clinical textbook for veterinary technicians, ed 7. St. Louis, Saunders, 2010.)
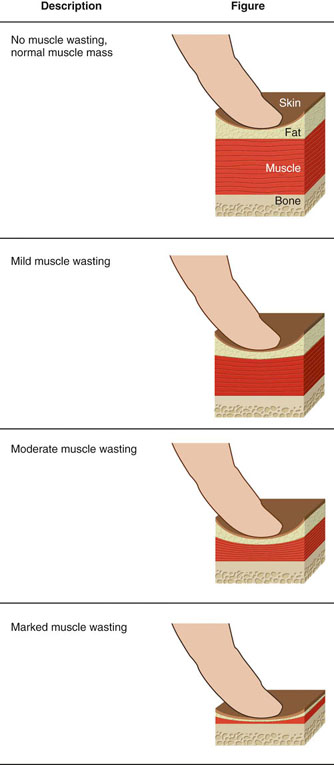
Figure 15-2 A muscle condition scoring (MCS) system. Evaluation of muscle mass includes visual examination and palpation over the temporal bones, scapulae, ribs, lumbar vertebrae, and pelvic bones. (Adapted from Baldwin K, Bartges J, Buffington T et al.: AAHA Nutritional assessment guidelines for dogs and cats, J Am AnimHospAssoc 46:285, 2010. IN Little S: The Cat: Clinical Medicine and Management, ed. 1, St. Louis, 2012, Saunders.)
Role of Nutrition in the Prevention of Musculoskeletal Disease
Developmental Orthopedic Disease
Obesity
Role of Nutrition in the Treatment of Musculoskeletal Disease
Nutrition and Surgery
Nontraumatized Surgical Patients
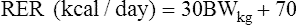
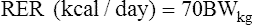
Traumatized Surgical Patients
Nutrition and Rehabilitation
Essential Nutritional Factors
Water
Energy
Fat
Carbohydrates
Protein
Obesity
Nutritional Compounds Evaluated in Dogs or In Vitro Using Canine Cells
Antioxidants
S-Adenosylmethionine.
Other Antioxidants.
Avocado/Soybean Unsaponifiables
Blueberries
Boswellia serrata
Chondroprotectants
Glucosamine and Chondroitin.
The New Zealand Green-Lipped Mussel
Omega-3 Fatty Acids
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


The Role of Chondroprotectants, Nutraceuticals, and Nutrition in Rehabilitation
Only gold members can continue reading. Log In or Register to continue
