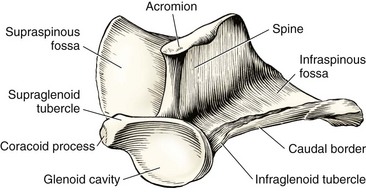
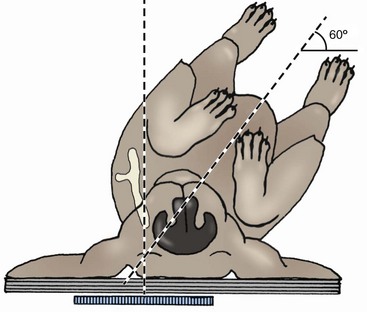
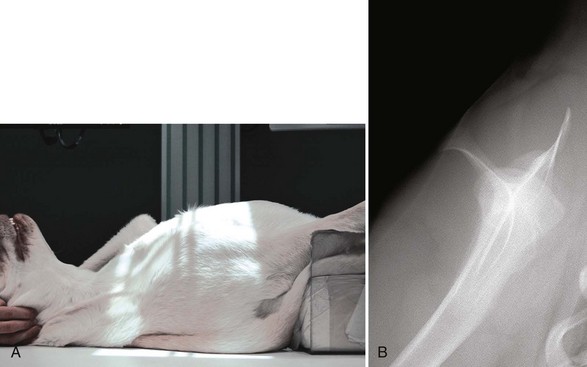
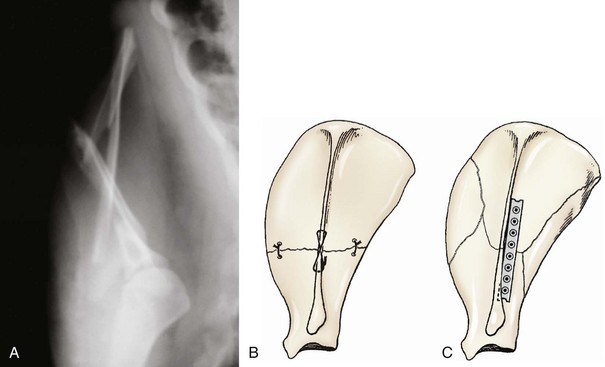
Chapter 50 The scapula is a flat bone with fairly extensive muscular protection both medially (subscapularis and serratus ventralis muscles) and laterally (omotransversarius, supraspinatus, infraspinatus, deltoideus, trapezius, triceps, and teres minor muscles). Scapular fractures are reported to account for approximately 0.5% to 2.4% of all fractures in dogs.1–4 The only large case series available in the veterinary literature reported the incidence of scapular fracture as 1.2% of all canine fracture cases.1 As a result of extensive soft tissue protection, substantial trauma is required to produce scapular fracture. Consequently, 56% to 70% of scapular fractures reportedly have concurrent injuries.1,5 The most common concurrent injuries include thoracic injury, fractures of other bones, and neurologic trauma. The dorsal border of the scapula, the scapular spine, and the acromion (at the distal extent of the scapular spine) are the palpable bony landmarks of the scapula. Important surgical landmarks include the fossae cranial and caudal to the scapular spine, which serve as the origin for the supraspinatus and infraspinatus muscles, respectively; the acromion, which is the origin of the acromial head of the deltoideus muscle; the supraglenoid tubercle, which is the origin of the biceps brachii muscle; and the glenoid cavity, which serves as the articulation with the humeral head (Figure 50-1). The suprascapular nerve emerges cranially from the scapular notch and travels caudally to wrap distal to the scapular spine, deep to the acromion. The axillary nerve emerges from the caudal border of the subscapularis muscle and crosses the caudal aspect of the scapulohumeral joint.15 As with all skeletal imaging, at least two orthogonal views are required for radiographic evaluation of the scapula. The standard scapular craniocaudal view is taken with the thorax rotated approximately 30 degrees away from the limb being radiographed (Figure 50-2). The mediolateral view is taken with the limb retracted caudally, thus forcing the scapula cranially and superimposed over the cervical vertebrae, rather than over the thorax.13 An additional radiographic view, the distoproximal or axial view, was advocated by Roush for more complete evaluation of scapular fracture.16 The image is taken with the patient in dorsal recumbency. The elbow is extended and the limb pulled caudally so it is parallel with the table, and the humerus is 90 degrees to the scapular spine (Figure 50-3).16 Several scapular fracture classification systems have been described. These systems have traditionally described scapular fractures based on anatomic location of the fracture: type I—fractures of the body and spine (including the acromion); type II—fractures of the neck; and type III—glenoid fractures (including the supraglenoid tubercle).13 Systems that describe fractures solely on the basis of anatomic location do not take into account the biomechanical considerations necessary to make surgical decisions. Cook et al.1 developed a scapular fracture classification scheme that attempts to aid in case management. Classification with this scheme, from least to most severe, is as follows: stable extra-articular, unstable extra-articular, and intra-articular. Surgical stabilization is advised for unstable extra-articular and intra-articular classifications. Unstable extra-articular fractures include displaced scapular neck fractures, fractures of the acromion, and unstable, overriding scapular body fractures, and may also include scapular body fractures with severe angulation.1 As noted in the fracture classification scheme, the decision to manage scapular body fractures conservatively, rather than with surgical stabilization, is based largely on the stability of the fracture and the pattern of displacement (Figure 50-4). Additionally, the presence of concurrent orthopedic injuries must be considered. Multiple-limb injury typically indicates the need for surgical stabilization. For those fractures that are managed conservatively, application of a Velpeau sling improves patient comfort and minimizes the likelihood of further fracture displacement. The sling is typically maintained, along with strict confinement, for 3 to 4 weeks. To minimize the risk of flexural contracture of the carpus, some authors advocate not including the flexed carpus in the bandage (i.e., allow the carpus/pes to be extended outside the bandage).4 If the “modified” Velpeau is used, the paw must be monitored closely for swelling. Conservative management is often successful because the extensive muscle-derived blood supply of the scapula provides a favorable environment for bone healing. When a scapular body fracture is surgically stabilized, a lateral approach is made over the spine of the scapula. After incision of the deep fascia along the spine of the scapula, the omotransversarius and trapezius muscles are retracted cranially, and the spinous head of the deltoideus muscle is retracted caudally.15 The supraspinatus and infraspinatus muscles are elevated from the scapular spine and the cranial and caudal fossae, respectively. Bone plates are commonly used for the stabilization of scapular body fractures. However, the thin bone of the cranial and caudal fossae provides little purchase for bone screws. The advent of the use of locking plates may improve the success of plating at the fossae, although no current reports in the veterinary literature describe their use for this purpose. More bone is available for screw purchase at the base of the scapular spine (Figure 50-5). Inverted tubular plates have traditionally been recommended for a “best fit” when plating at this location. The plate can be placed cranial or caudal to the spine. The proximal-to-distal cross-sectional morphometry of the scapular spine has been studied to evaluate bone thickness available for screw purchase. The study evaluated bone depth available for screw purchase with a screw angled at 45 degrees to the scapular spine (see Figure 50-5). Study investigators concluded that bone depth was greater cranially in the ventral half of the scapular spine and caudally in the dorsal half of the scapular spine.10 The implication is that fractures within the dorsal half of the scapular body should be plated caudally, and fractures in the distal half should be plated cranially. The study did not address ideal plate location for midbody fractures.
Scapula
Scapular Body Fractures
< div class='tao-gold-member'>
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree