49 Retinal detachment
CLINICAL EXAMINATION
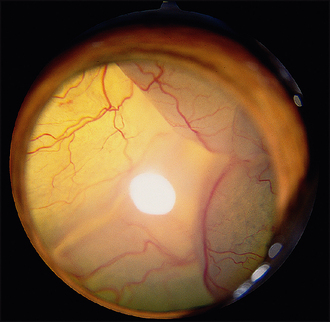
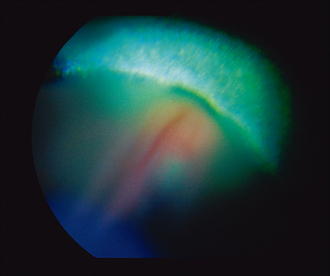
Most eyes will be ‘quiet’ with no pain or ocular redness. Some might have cataract formation which could preclude fundus examination – indeed the owner might believe that the patient is blind due to the cataract alone. The eye might also look opaque due to the retinal detachment itself – if a total bullous or rhegmatogenous detachment is present this can be visualized as a grey ‘veil’ floating immediately behind the lens (Figure 49.1). It can be seen on direct illumination with a pen torch without the need for an ophthalmoscope in many cases. If the retina has torn from its dorsal attachments at the periphery behind the lens, it will fall forward over the optic disc, obscuring it, while the tapetum will be more exposed and extremely hyper-reflective above the retinal detachment (Figure 49.2). There will be a complete absence of retinal vessels dorsal to the disc but they may be visualized out of focus in the grey detached ventral retina.
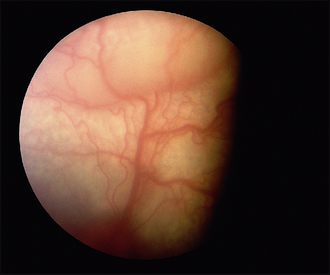
Less severe detachments will require ophthalmoscopy and will manifest as out-of-focus areas of the retina and a reduction in reflectivity due to increased thickness of the retina as it becomes oedematous and fluid accumulates between the retina and tapetum (Figure 49.3). Perivascular cuffing (exudates around the blood vessels) might be noticeable along with retinal, and sometimes vitreal, haemorrhage as the detached vessels are stretched and torn. If the patient is blind in just one eye with a total detachment, the other fundus should be carefully evaluated for early signs of problems – for example, collie eye anomaly, retinal dysplasia, chorioretinitis, vascular anomalies and so on could be present.
CASE WORK-UP
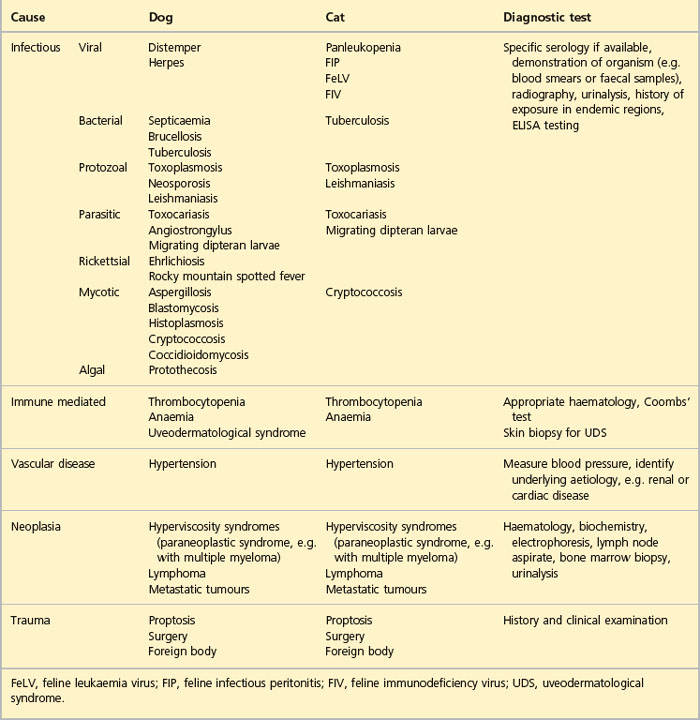
A fairly extensive work-up can be required to reach a definitive diagnosis in cases of retinal detachment, particularly in adults with serous detachments. Blood samples should be taken for haematology and biochemistry screening. These might show a neutrophilia suggesting infectious disease or hyperviscosity syndromes for example, such that serum electrophoresis is warranted, along with bone marrow biopsy. Renal and hepatic disease might be present. Urinalysis should be considered. Systemic blood pressure should always be taken since hypertension is a common cause of retinal detachment in both dogs and cats. If chorioretinitis is suspected, specific serological testing for the various causes of this can be considered (Table 49.1).
If the fundus cannot be directly visualized, for example because of the presence of a total cataract, then ocular ultrasonography will be invaluable in detecting a retinal detachment. General abdominal and cardiac ultrasonography might also be indicated depending on the preliminary investigation results – looking for cardiac disease or adrenal masses in cases of systemic hypertension for example, or for the location of a primary tumour in hyperviscosity syndromes. Unfortunately, in some instances, the underlying aetiology might not be revealed despite extensive work-up.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree