Ocular Surgery
Conjunctival Rotating Pedicle Flap
Corneal ulceration and trauma leading to rupture of the eye requires emergency management to restore sight and function. Conjunctival pedicle flaps have been used successfully to seal these defects and facilitate healing of the cornea of camelid patients.1,2 This procedure is done under general anesthesia and is greatly improved with the use of an operating microscope to ease suture placement. The edges of the defect are carefully debrided and any protruding tissue (e.g. iris) trimmed. The anterior chamber may require an infusion of an air bubble or viscous fluid to reestablish its volume after the defect has been successfully sealed. Although conjunctival sliding advancement pedicle grafts are occasionally done, the most common type of conjunctival flap is made parallel to the limbus as a rotating pedicle flap. The length of the flap should be positioned such that the corneal defect is located at approximately the junction of the one third length closest to the base of the pedicle and the middle one third of the graft. This allows rotation of the graft in a manner that minimizes the tension and angle of rotation. Preservation of blood flow to the graft is essential for successful healing. The length of the graft should be longer than the distance from the base to the defect; if the graft base is 1.5 centimeters (cm) from the defect, a 2-cm pedicle graft will ensure sufficient length for rotation and suturing without tension. The graft should be wider than the corneal defect; if the defect is 0.5 cm in diameter, the graft should be approximately 0.75 cm wide. The conjunctiva is harvested from the limbal margin closest to the defect to minimize the length of graft needed. The graft should be harvested as a thin, semitransparent tissue to minimize the thickness of the healed cornea after grafting. The fibrous layer covering of the conjunctiva (Tenon capsule) should be dissected free from the conjunctiva involved in the pedicle graft so as to minimize the risk of dehiscence of the graft. The surgeon must use care when separating these tissue layers so that the integrity of the conjunctival graft is not disrupted. The conjunctiva is sutured to the margins of the defect by using No. 6-0 to No. 8-0 polyglactin (PG)-910 suture material and a simple interrupted suture pattern. Sutures are placed as partial thickness in the cornea to avoid causing further injury to the anterior chamber of the eye. After securing the pedicle graft, the harvest bed should be sutured closed by using No. 6-0 absorbable suture material in a simple continuous suture pattern. This will help minimize the risk of morbidity at the graft donor site.
Enucleation
Enucleation may be indicated because of ocular neoplasia, congenital defects, trauma, glaucoma, or infection (Figure 56-1).3,4 Clinical experience suggests that camelids adapt rapidly to monocular vision.
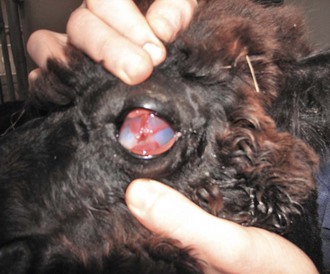
Figure 56-1 Ocular trauma in a juvenile alpaca. Note the corneal opacity and the conjunctival adhesions to the cornea.
Clinical experience suggests that camelids may be more prone to sudden and excessive parasympathetic responses (“vagovagal reflex”) during ocular surgery.5 Extreme parasympathetic responses are associated with bradycardia, hypotension, and cardiovascular collapse. This has been observed in several llamas and alpacas during enucleation, and the surgical team must be prepared to respond quickly and efficiently to these emergencies. In one 3-year old alpaca, respiratory failure occurred during the immediate postoperative period, requiring mechanical ventilation for a period of 20 hours.5
Preservation of a sterile or clean-contaminated orbit during removal of the eye can be accomplished using a transpalpebral approach. First, the upper and lower eyelids are sutured closed using a simple continuous pattern, stainless steel skin staples, or penetrating towel clamps. This helps seal the external portions of the globe and prevent contamination of the orbit. Then, a skin incision is made approximately 0.5 cm from the margins of the eyelids until a circumferential incision is complete. The skin incision is continued in a manner so as to reflect the skin away from the eyelids and towards the bony rim of the orbit. Mayo or metzenbaum scissors are used to dissect through the periorbital tissues, muscles, and fascia until the optic pedicle is isolated. This process is facilitated by using the interior of the bony orbit as a guide for dissection. Transection of the medial and lateral canthal ligaments allows access to the caudal aspect of the orbit. Hemostasis is established, as needed, during dissection. In most cases, complete excision of orbital tissue is desired. Careful technique is advised during transection of the optic nerve and ophthalmic artery. Tension can be minimized by use of a right-angled vascular clamp, which also aids in hemostasis during excision of remaining orbital tissue (Figure 56-2). The pedicle is ligated using No. 2-0 absorbable suture material. Rapidly absorbing suture materials, such as polyglecaprone, reduce the potential for foreign body reaction or suture site infection. A transfixation suture may be required to ensure adequate security of ligation. A variety of suture patterns can be used to close the skin incision. Nonabsorbable, monofilament suture materials, such as No. 1 nylon or polypropylene, are recommended to minimize the risk of complications such as suture tract infection. Appositional suture patterns such as simple interrupted sutures, Ford interlocking suture pattern, cruciate suture pattern, or simple continuous suture patterns are recommended.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree