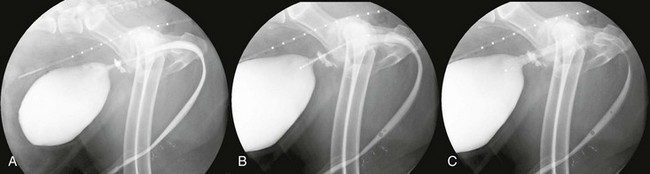
Chapter 76 Urethral stenting has been described in several human studies. Reports of the treatment of malignant urethral obstructions in both dogs and cats have been published (Christensen et al, 2010; Newman et al, 2009; Weisse et al, 2006), and this treatment is now available in many clinics (Figure 76-1). In the first veterinary case series (Weisse et al, 2006), 12 dogs underwent placement of urethral stents to relieve malignant urethral obstructions secondary to prostatic or urethra-bladder neoplasia; in all cases, the dogs were experiencing severe or complete obstruction. All dogs regained the ability to urinate after stent placement. Although urinary incontinence occurred in 25% of cases after stenting, the outcome was considered fair to excellent in 10 of 12 dogs (Weisse et al, 2006). Urethral stenting has been reported in two separate feline case reports of malignant obstruction as well (Christensen et al, 2010; Newman et al, 2009). Both cats were diagnosed with urothelial carcinoma and were noted to have successful urination after stent placement. Figure 76-1 Urethral stenting: prostatic carcinoma. A, A positive-contrast cystourethrogram has been obtained, and a urethral obstruction in the region of the prostate is noted. B, A urethral stent has been placed over a guidewire and is positioned over the obstructed region of the urethra. C, The stent has been deployed, and the obstruction has been relieved. A technique for percutaneous placement of ureteral stents in dogs with malignant ureteral obstruction was reported recently (Berent et al, 2011). In this series of 12 dogs, the obstructed ureters were accessed in antegrade fashion through the placement of a needle within the renal pelvis (successful in 11 of 12 dogs); ultrasonographic guidance was used to position the needle appropriately. In all cases, a double-pigtail stent was placed with the goal of leaving the cranial pigtail in the renal pelvis and the caudal pigtail in the urinary bladder beyond the obstruction. All patients with azotemia demonstrated improvement in blood urea nitrogen and creatinine concentrations after stent placement. Of the 10 patients that underwent abdominal ultrasonography after stent placement, all were demonstrated to have decreased severity of hydronephrosis and hydroureter. Overall, ureteral stent placement was determined to be safe and well tolerated in that cohort of dogs.
Interventional Oncology
Veterinary Interventional Oncology Treatment Categories
Palliation
Stenting of Malignant Obstructions
Urethra.
Ureter.
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Interventional Oncology
Only gold members can continue reading. Log In or Register to continue
