Chapter 16 Hemorrhage (Gastrointestinal)
Definition
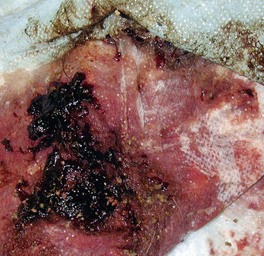
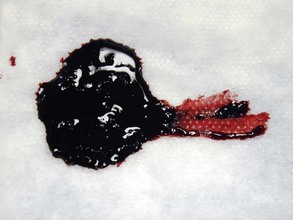
Gastrointestinal (GI) hemorrhage can be occult or it can be heralded by significant blood loss via the oral cavity or anorectum. Hematemesis refers to conditions associated with the vomiting of blood (Fig. 16-1). Hematochezia refers to frank red or reddish-brown blood pigments in the feces, while melena refers to black, tarry feces (Fig. 16-2). Melena requires significant blood loss in a relatively short period of time, and the blood must remain in the stomach and/or small intestine long enough to be at least partially digested before passage in the feces. Many patients have melena and hematemesis concurrently, but some patients may only have one of these signs. Other patients may be dying of severe GI hemorrhage, but may not have obvious melena.
Pathophysiology and Mechanisms
Hematemesis and melena can have similar causes, all principally upper GI in location. Gastric ulceration or erosion is one of the more commonly sought causes of upper GI hemorrhage.1 Gastric ulceration or erosion has many causes, including poor gastric mucosal blood flow, interference with normal prostaglandin metabolism, excessive gastric acidity, and direct damage to the mucosa (e.g., chemicals, foreign objects).2
Direct damage to gastric mucosa may be caused by drugs (e.g., aspirin and other nonsteroidal antiinflammatory drugs [NSAIDs]), various ingested toxic substances (chemicals, plants), tumors, and even mucosal trauma associated with repeated, vigorous vomiting. Cats are infrequently affected with gastric ulceration or erosion, but have the same possible causes as dogs.3 Helicobacter spp. do not appear to be a major cause of gastric ulceration or erosion in dogs or cats as they do in humans, even though numerous organisms can be found in ulcerative tissue.4 Despite long-standing beliefs, renal failure does not appear to be a common or important cause of gastric ulceration/erosion.5
Intestinal ulceration/erosion is much less common than gastric ulceration/erosion. Disruption of intestinal mucosa is primarily caused by infiltrative disease (e.g., neoplastic or inflammatory) or inability to neutralize gastric acidity (e.g., paraneoplastic effects of mast cell tumors and gastrinomas). It can also be associated with many of the NSAIDs (e.g., flunixin).6 Hookworms can be surprisingly severe, even in older patients in endemic or unsanitary environments; monthly preventatives do not necessarily eliminate ancylostomiasis.
Differential Diagnosis
Anemia
Anemia can cause obvious clinical signs or may be discovered serendipitously during routine blood testing. Anemia has three major causes: hemolysis, hemorrhage, and bone marrow disease. Anemia occurring in conjunction with hypoalbuminemia is suggestive of blood loss, particularly from the GI tract. Anemia resulting from GI hemorrhage may be regenerative or nonregenerative, depending upon chronicity of the condition, but classically is more often associated with hypoalbuminemia (not necessarily hypoproteinemia or panhypoproteinemia). Chronic GI hemorrhage presents typically as a poorly regenerative, iron deficiency–type anemia (microcytic and hypochromic) with moderate to severe hypoalbuminemia.7 However, GI blood loss must be substantial and of sufficient chronicity to produce these specific changes; most animals with GI hemorrhage do not have this type of anemia. Hemorrhage sufficient to cause anemia often occurs in the absence of hematemesis, hematochezia, and melena.
Hematemesis
The most common causes of gastric ulceration or erosion in dogs are drug-induced (e.g., NSAIDs, dexamethasone, and other glucocorticoids8), stress (e.g., hypovolemic shock, systemic inflammatory response syndrome, excessive physical exertion), cancer disruption of the gastric mucosa, adrenal insufficiency, and hepatic failure.1,2,9
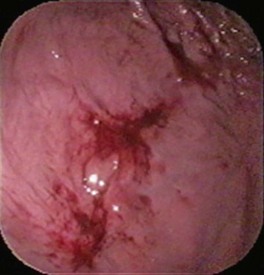
Dual or multiple risk factors (e.g., NSAIDs plus dexamethasone or NSAIDs plus poor mucosal perfusion) increase the likelihood of gastric ulceration or erosion.1,10 Cyclooxygenase (COX)-2 selective inhibitors (e.g., carprofen, etodolac, deracoxib, meloxicam) have been developed to minimize the ulcerogenic effect of NSAIDs in the GI tract. Although these newer NSAIDs lessen the risk of gastric ulceration or erosion, they do not completely eliminate it. Many dogs have developed gastric ulceration or erosion following use of these putatively safer NSAIDs.11,12 Some NSAIDs are especially well known for their ulcerogenic potential in dogs, including naproxen and flunixin meglumine.6 It should be noted that gastric ulceration or erosion is not excluded by an absence of hematemesis or anemia. Dogs with substantial gastric bleeding because of stress-related gastric ulceration or erosion can appear clinically normal and function at a high level (Fig. 16-3).2 Furthermore, there appears to be little relationship between bleeding and perforation as they do not necessarily arise from the same pathogenesis.
Cats are infrequently diagnosed with gastric ulceration and erosion. Lymphoma and other tumors appear to be the most important causes of gastric ulceration in this species, but there are very few published studies in cats to confirm or deny this opinion.3
It should be confirmed that “hematemesis” is not just reddish tinged gastric fluid caused by food digestion in the stomach. True hematemesis may range from minimal to copious amounts of blood. If there are simply a few spots or “flecks” of blood (Fig. 16-4), gastric mucosal trauma as a consequence of vigorous vomiting is a major differential (Fig. 16-5). If copious, there are numerous possible causes, and a methodical approach is best (Fig. 16-6). If history, physical examination, and routine blood tests do not give clues as to the cause of hematemesis, the basic approach should be to first eliminate coagulopathy, search for evidence of upper GI mucosal disease, and, finally, respiratory tract disease with ingestion of blood following hemoptysis.
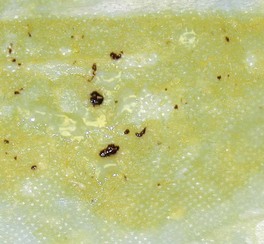
Figure 16-4 Vomitus from a dog with pancreatitis. Most of the material is bilious, but there are several spots of blood present. (Compare with Fig. 16-1.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree