• The hoof capsule is comprised of tubular and intertubular keratin arranged as a laminated composite material. • Ninety per cent of the energy imparted by foot strike is dissipated by the hoof capsule and its associated structures. • The anatomy of the support structures within the hoof must be understood to appreciate the various sites that could cause distal limb lameness. The hoof capsule not only provides strength but also supports the horse’s skeletal column. In the horse, the tubular hoof of the wall is composed of hard keratin and is rich in disulphide bonds, so has great physical strength. The frog and the white zone are rich in sulfhydryl groups, but poor in disulphide bonds, and therefore have lower physical strength but greater elasticity. The strength, hardness, and insolubility of keratin are due to disulphide bonds between and within the molecules. The corium is the region of the foot that nourishes the hoof-wall cells. There are several distinct zones, the coronary corium, lamellar corium, solar corium, and frog corium. The coronary corium fills the coronary groove and blends distally with the lamellar corium. Its inner surface is attached to the extensor tendon and the cartilages of the coffin bone by the subcutaneous tissue of the coronary cushion. Collectively the coronary corium and the germinal epidermal cells that produce the hoof wall are known as the coronary band. A feature of the coronary corium is the large numbers of hair-like papillae projecting from its surface.1 The supporting structures within the hoof include the collateral cartilages, digital cushion, digital extensor tendon, collateral ligaments of the distal interphalangeal joint, deep digital flexor tendon, collateral sesamoidean ligament, distal sesamoidean impar ligament.2 The collateral cartilages have considerable variation in anatomic details from horse to horse. They vary in thickness and degree of mineralization, but the heel portion is usually thinner than the more dorsal and distal portions. The cartilages are stabilized by ligaments that attach to the middle and distal phalanges, the navicular bone and to the collateral sesamoidean ligaments. A venous plexus lies on the abaxial surface of the cartilage.2 The digital cushion is an elastic tissue composed of collagen, elastin and adipose tissue. It lies between the frog and the deep digital flexor tendon at the heel of the foot and is responsible for shock absorption.2 The navicular bone is stabilized by: 1. the paired collateral sesamoidean ligaments which originate on the distal, abaxial and dorsal aspects of the first phalanx and insert on the abaxial surfaces of the second phalanx and the proximal border of the navicular bone 2. the distal sesamoidean impar ligament which originates on the distal border of the navicular bone and inserts on the flexor surface of the distal phalanx and 3. the distal extension of the deep digital flexor tendon that courses over the flexor surface of the navicular bone and inserts on the flexor surface of the distal phalanx. The distal border of the navicular bone also has synovial invaginations that contain blood vessels.2 The distal interphalangeal joint shares an articulation with the dorsal surface of the navicular bone and is stabilized by collateral ligaments that originate on the distal abaxial surface of the middle phalanx and insert in the abaxial surface of the distal phalanx.2 This joint has a dorsal and palmar pouch. The dorsal pouch extends proximally to the mid-portion of the middle phalanx. The palmar pouch is extensive and is closely associated with the palmar nerves, making desensitization of palmar structures of the foot with anatomic specificity problematic.2,3 The navicular bursa lies between the deep digital flexor tendon and the flexor surface of the navicular bone and has close association with the distal interphalangeal joint. Size, shape, toe length, heel length, hoof pastern axis, and position of each foot relative to each limb and to each other are assessed with the horse standing quietly.4–6 Hoof alignment is viewed from the dorsal and lateral aspect.2 Most horses will have a hoof angle between 50 and 55°. Ideally, when the horse is standing square; the cannon bone, pastern, and hoof should have straight axial alignment as observed from the front. From the side, the hoof/pastern axis should be straight. The angle created by the dorsal hoof wall should be the same as the pastern angle and the heel angle should be within 5° of the toe angle.7 Horses that have a low hoof angle compared to the pastern have a broken-back hoof/pastern axis (Fig. 14.1). This hoof conformation is also called ‘long toe and low heel’. The opposite case is a steep hoof angle and sloping pastern which will have a broken-forward hoof/pastern axis. This hoof conformation may also be called ‘club foot’. From this point it is natural to begin manipulating the foot in the non-weight-bearing position.4 Begin by cleaning the bottom of the hoof and lightly paring away any debris that obscures visualization of the frog, sulci of the frog, sole, and white line if the horse is unshod. The frog should be examined for size, shape, and consistency, and to determine whether it is securely attached to the underlying tissue and its sulci (collateral and central). The frog should be resilient and rubbery, rather than hard and flaky, and the caudal two-thirds should be nearly level with the ground surface of the hoof wall. The frog should not be recessed deep into the sulci of the foot and nor should the frog be convex at its apex. The receded frog is often associated with upright narrow feet, whereas the convex frog is associated with weak and underrun heels. Lightly support the limb at the metacarpus (metatarsus) and allow the foot to drop naturally. Position your line of vision so as to appreciate foot balance and levelness of the walls (see above). Examine the entire ground surface of the foot to determine the divisions of the hoof (toe, quarters, and heels) and their proportions (Fig. 14.2). Imagine a line drawn through the axial center of the limb, which transects the ground surface of the foot, and then determine the relative proportion of medial and lateral foot to this imaginary line. For example, a given foot may demonstrate a unilateral medial heel contraction in combination with a flared lateral quarter and toe (diagonal imbalance). If the horse is shod, the exam should include the following additions.4 Note the shoe type as well as the presence or absence of additions such as toe grabs, block heels, trailers, and so forth. Determine if abnormal shoe wear exists. As part of the overall evaluation of the horse an objective assessment of hoof balance is important. Examination of lateral and dorsopalmar (plantar) radiographic projections of the hoof allows objective evaluation of hoof balance. The lateral radiograph should be evaluated for middle and distal phalanx alignment, which may reveal the presence of a broken-hoof axis (Fig. 14.3). In addition, the alignment between the distal phalanx and the hoof wall should be assessed. If the hoof wall and dorsal surface of the distal phalanx are not parallel the functional hoof angle can be determined by measuring the angle of the dorsal surface of the bone with the ground. The slope of the heels can be seen on the radiograph and evaluation is used to determine whether the heels are underrun. The dorso-palmar radiographic projection should be assessed for joint alignment, medial and lateral hoof wall lengths, and foot symmetry (Fig. 14.4). Joint alignment is determined by examining the symmetry of the joint space. The hoof wall length can be measured directly from digital images. Two manipulative tests should be performed: hoof tester examination and distal limb flexion. Two additional manipulations, hoof extension wedge test, and palmar hoof wedge test, may add more information.8 A positive response to any of these tests is important but a negative response is equivocal and does not rule out any problem. Examine the foot systematically with hoof testers. Percussion utilizing a small hammer can also provide important information regarding pain in the hoof wall or sole. The distal limb flexion test can exacerbate lameness if any of the three distal joints of the leg are affected by synovitis or osteoarthritis. A positive response could also be expected by any condition that causes induration of the tissues of the foot. This has been shown to be positive in over 95% of horses with foot pain.8 After localization of the lameness to the foot imaging will be necessary to determine what pathology is present. Radiographic examination of the hoof requires a minimum of five radiographic views of each foot.9 The views consist of a dorso-60°-proximal to palmarodistal (D60PrPD) of the navicular bone, a dorso-45°-proximal to palmarodistal (D45PrPD) of the distal phalanx, a lateral to medial projection, a horizontal dorsopalmar projection, and a palmaroproximal to palmarodistal navicular bone projection (navicular skyline). Digital imaging is the current standard for radiography and provides more detail than analog film/screen radiography, allows for manipulation of image window and level, and permits measurement of various aspects of conformation using DICOM image software. Many structures within the hoof may be evaluated sonographically.10 The collateral ligaments of the DIP joint can be clearly identified, as can the deep flexor insertion on the third phalanx, the distal deep flexor tendon, the impar ligament, and the navicular bursa (see Chapter 20). The presence or absence of inflammation within the distal limb can be evaluated through the use of nuclear scintigraphy.11 Magnetic resonance imaging (MRI) has increased the understanding of the inter-relationships between soft tissues, bone and cartilage within the foot. To fully determine the cause of foot lameness, MRI must be considered for a horse with lameness that resolves with distal limb diagnostic analgesia and that has few abnormalities evident on a radiographic or sonographic study of the distal limb. MRI allows for high-detail imaging in multiple planes and is a particularly sensitive technique for soft tissue evaluation.12,13 Imaging with fat suppressed MRI sequences also provides a degree of physiological understanding of the region. For example, fat suppressed MRI imaging may identify increased levels of fluid within bone, referred to as bone contusion or bone edema that cannot be identified with any other imaging technique.14 • Lameness associated with hoof wall defects is due to irritation of the sensitive lamellae due to exposure, local infection or shearing of the unstable hoof capsule. • Treatment should clean and stabilize the defect to permit healing from the coronary band. Healing of these injuries is based on growth of new horn from the coronary band. These tissues do not heal side to side; therefore healing is slow, and may take 5–10 months. The defect must be stabilized to prevent the crack from expanding. This can be accomplished by application of a bar shoe that relieves pressure on the affected wall. The bar may be a full bar or a diagonal bar. Also, if the crack is near the heel, weight bearing to the heel can be reduced by floating the heel (Fig. 14.5). The affected heel is trimmed short enough to prevent contact with the shoe during weight bearing. The objective is to relieve shear forces across the defect, which may cause movement at the area of the crack. In addition, clips placed on either side of the defect will help prevent hoof expansion and, therefore, will further immobilize the crack. The crack may also be sutured or wired. In some cases a small metal plate can be screwed into the wall over the crack. • First aid should control hemorrhage and prevent further contamination. • Damage to the corium may result in hoof wall defects. • Deep wounds may affect synovial structures. • Wounds that involve the hoof capsule will heal slowly by second intention. Lacerations to the hoof causing loss of germinal tissue and either partial or complete avulsions of the hoof wall are not common injuries to the horse. When these injuries do occur, however, their management can be perplexing for the veterinarian.
Diseases of the foot
Anatomy
Examination of the distal limb
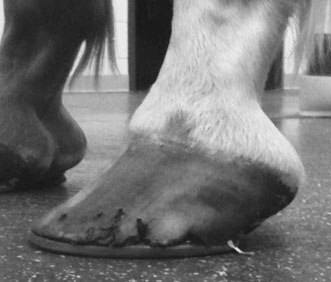

Objective assessment of hoof balance
Assessment of pain
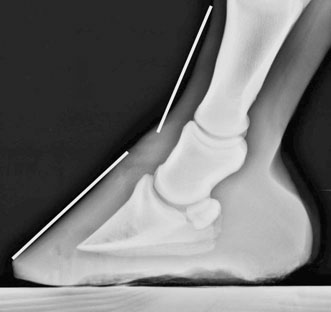
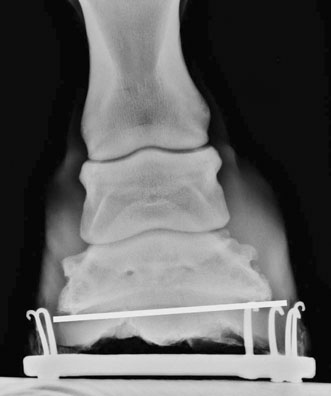
Imaging of the foot
Diseases of the hoof wall
Hoof wall defects
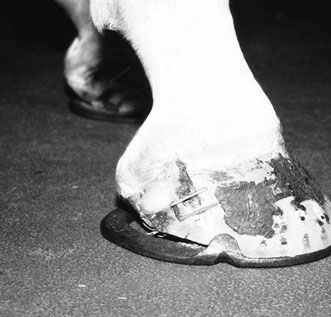
Treatment and prognosis
Therapy
Lacerations to the hoof and coronary band

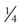 inch) using a rotary hand burr. Some defects can be reinforced by wire laced across the gap. This not only helps immobilize the area but also adds substrate to which the repair material can bond. If the defect is not sutured, holes should be drilled from the normal hoof into the undermined area to allow penetration of repair material. The holes should be 0.5 to 1 cm apart.
inch) using a rotary hand burr. Some defects can be reinforced by wire laced across the gap. This not only helps immobilize the area but also adds substrate to which the repair material can bond. If the defect is not sutured, holes should be drilled from the normal hoof into the undermined area to allow penetration of repair material. The holes should be 0.5 to 1 cm apart.

