Chapter 104 Vestibular Disease
• Patients with vestibular disease have dysfunction of the vestibular system and are often presented for treatment on an acute emergency basis.
• The vestibular system is comprised of a peripheral component within the structures of the inner ear and central components in the brain stem and cerebellum.
• Central vestibular disease typically is accompanied by loss of proprioceptive and motor function, in addition to multiple cranial nerve deficits and mentation changes.
• The differential diagnosis for the cause of vestibular disease depends on the localization of the lesion to the peripheral or central components.
NEUROANATOMY OF THE VESTIBULAR SYSTEM
Nerve Pathways to the Extraocular Muscles
Two neurons make up the pathway responsible for the sensory input of the head to the cerebral cortex (Figure 104-1).
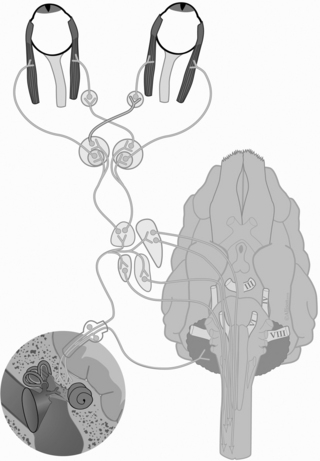
Figure 104-1 Diagrammatic overview of the neuroanatomy of the vestibular system.
From Platt S, Olby N, editors: Manual of canine and feline neurology, ed 3, Gloucester, 2004, British Small Animal Veterinary Association.
CLINICAL SIGNS
Specific Signs of Vestibular Dysfunction
Signs of vestibular dysfunction are outlined in Table 104-1.
Table 104-1 Neurologic Examination Findings in Animals With Peripheral and Central Vestibular Dysfunction
| Clinical Signs | Peripheral Vestibular Disease | Central Vestibular Disease |
|---|---|---|
| Head tilt | Toward the lesion | Toward the lesion, or away from the lesion with paradoxical disease |
| Spontaneous nystagmus | Horizontal or rotatory with the fast phase away from the side of the lesion Rarely positional | Horizontal, rotatory, vertical and or positional with the fast phase toward or away from the lesion |
| Paresis and proprioceptive deficits | None | Commonly ipsilateral to the lesion |
| Mentation | Normal to disoriented | Depressed, stuporous, obtunded, or comatose |
| Cranial nerve deficits | Ipsilateral CN VII deficit | Ipsilateral CN V, VII, IX, X, and XII |
| Horner’s syndrome | Common ipsilateral to the lesion | Uncommon |
| Head tremors | None | Can occur with concurrent cerebellar dysfunction |
| Circling | Infrequent but can be seen toward the side of the lesion | Usually toward the side of the lesion |
CN, Cranial nerve.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


