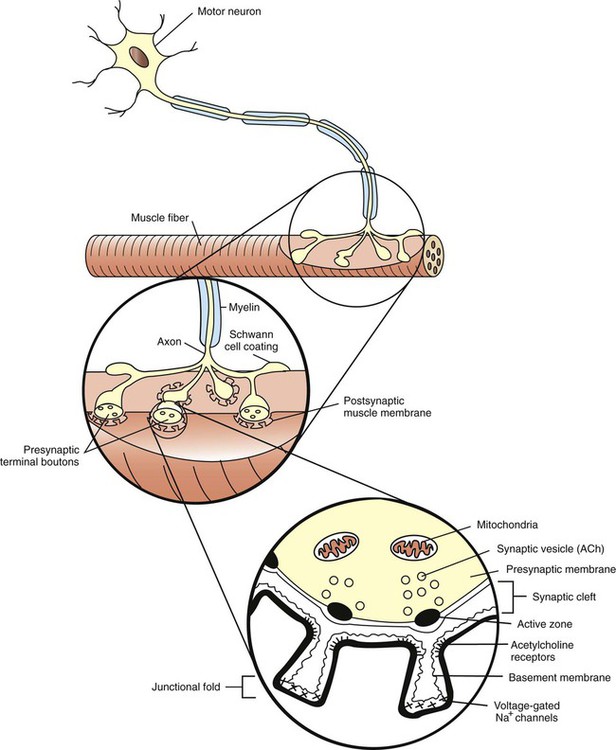
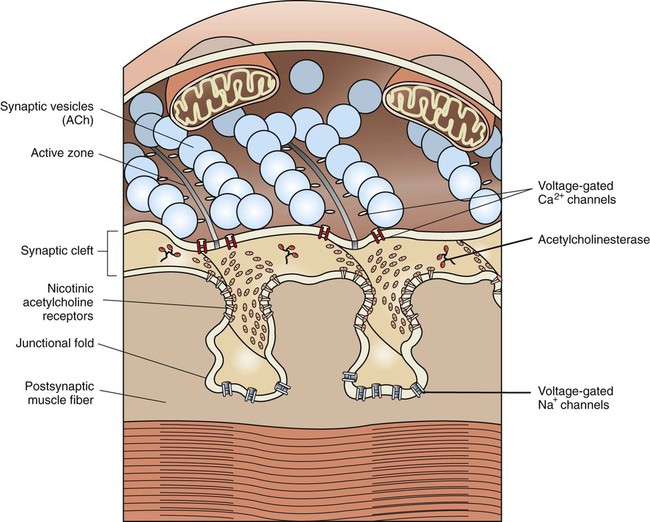
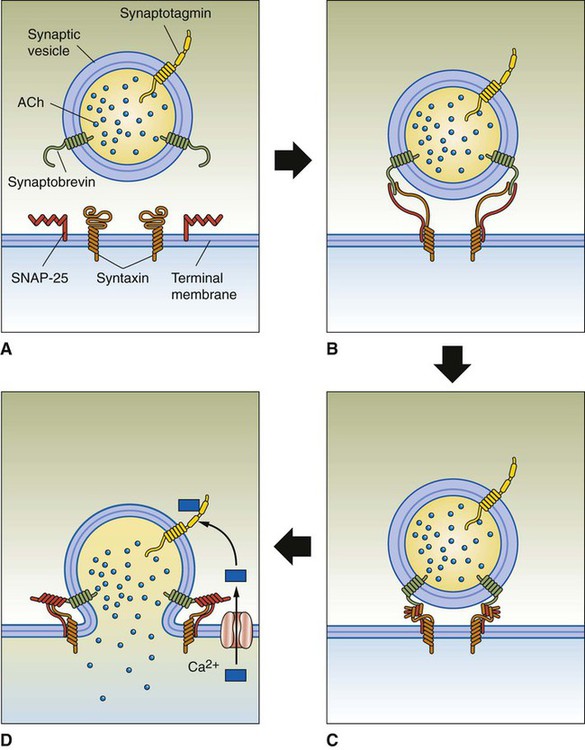
1. The anatomy of the neuromuscular junction is specialized for one-way synaptic communication. 2. An action potential on the presynaptic neuron triggers an action potential on the muscle cell through the release of acetylcholine. 3. There is greater variety in the specifics of neuron-to-neuron synaptic transmission than in transmission at the neuromuscular junction. Neurons communicate with each other and with other cells of the body, such as muscle and secretory cells. In Chapter 4 the generation of the action potential and its rapid conduction down the axon to the presynaptic terminal was discussed. Using these processes, the neuron can rapidly notify its presynaptic terminals, often located far from its cell body, to initiate the transfer of information to other cells. Such communication occurs between cells rapidly, and often focally, at specialized junctions called synapses (Greek, “junction” or “to bind tightly”). Synaptic transmission between cells can be either electrical or chemical. At electrical synapses, ionic current flows directly between presynaptic and postsynaptic cells as the mediator for signal transmission. Although electrical synapses in the mammalian nervous system appear to be more widespread than originally thought, synaptic transmission is more frequently mediated by a chemical messenger. Released from the presynaptic terminals on arrival of the action potential, this chemical messenger rapidly diffuses to the postsynaptic cell membrane, where it binds with receptors. This binding initiates a postsynaptic change in function, often generating a postsynaptic potential. The best-understood chemical synapse is that between a motor neuron and a skeletal muscle cell (fiber): the neuromuscular synapse, also known as the neuromuscular junction (Figure 5-1). Given the emphasis in Section II of this text on posture and locomotion, this synapse is the focus of this chapter. Synaptic communication at the neuromuscular junction is fundamentally similar to that between neurons, although there is greater variety in the specifics of neuron-to-neuron synaptic transmission, as also discussed. The neuromuscular junction, like most chemical synapses, has (1) a presynaptic side; (2) a narrow space between the neuron and muscle fiber, called the synaptic cleft; and (3) a postsynaptic side (see Figure 5-1). The presynaptic side of the synapse is made up of the terminal (transmitting) portion of the motor neuron. This presynaptic terminal has a swelled, buttonlike appearance and is also called a synaptic bouton. The terminal (or synaptic bouton) contains a large number of membranous storage vesicles, called synaptic vesicles, which contain the chemical neurotransmitter substance, in this case acetylcholine. These synaptic vesicles are lined up in rows along the inner surface of the terminal membrane (Figure 5-2). The presynaptic membrane region associated with each double row of vesicles is called an active zone and is the site where the synaptic vesicles will eventually release acetylcholine into the synaptic cleft. The presynaptic terminal also contains mitochondria, an indication of active metabolism in the cytoplasm. Some mitochondrial products (e.g., acetyl-CoA, ATP) play a role in the local synthesis of acetylcholine and in its movement into the synaptic vesicles. The presynaptic (neural) and postsynaptic (muscle) cell membranes are separated by a narrow space, the synaptic cleft, that is about 50 nm wide (see Figures 5-1 and 5-2). The cleft contains extracellular fluid and a basal lamina, composed of a matrix of molecules, that is a specialized region of the muscle basement membrane. Some of these matrix molecules mediate synaptic adhesion between neuron and muscle. The postsynaptic muscle cell membrane has several specialized features that facilitate synaptic transmission. Directly opposite the face of the presynaptic terminal, the postsynaptic muscle cell membrane contains receptors for the acetylcholine transmitter (see Figures 5-1 and 5-2). In this focal region the membrane has a series of invaginations, called junctional folds, that increase the surface area where acetylcholine receptors can reside. The acetylcholine receptors are most densely packed at the mouth of these junctional folds, and these mouths are closely aligned with the active zones of the presynaptic terminals from which the acetylcholine is released. Thus, there is a good match between the focal region of transmitter release from the neuron and the focal location of the receptors on the muscle fiber. Because the neurotransmitter is found only on the presynaptic neural side of the neuromuscular junction, transmission can go only from neuron to muscle, not in the reverse direction. Also, it should be noted that a motor neuron gives off several presynaptic terminals (synaptic boutons) to an individual muscle fiber. Together, this cluster of terminals is localized to a restricted region of the muscle fiber. An action potential on a motor neuron arises at its initial axon segment and then travels along the entire axon, eventually arriving at the presynaptic terminal (see Chapter 4). As previously noted, the exchange of Na+ and K+ ions, across axonal voltage-gated Na+ and K+ channels, is responsible for the generation of the action potential and its conduction to the terminal. However, as the action potential arrives at the presynaptic membrane, the wave of depolarization opens voltage-gated Ca2+ channels located in this region (see Figure 5-2); as Ca2+ flows toward equilibrium across the membrane, the Ca2+ enters the presynaptic terminal. This increase in the intracellular Ca2+ level is critical for the release of neurotransmitter from the terminal. Recall that the acetylcholine-containing synaptic vesicles are lined up at the active zones of the presynaptic terminal. They will dock there by the intertwining of binding proteins that respectively reside on the vesicle membrane (synaptobrevin) and on the inner surface of the terminal membrane (syntaxin and SNAP-25) (Figure 5-3). This holds the vesicles near the location of Ca2+ entry given that the voltage-gated Ca2+ channels are efficiently located in the vicinity of these active zones. When Ca2+ flows into the terminal, the ion binds with yet another protein on the synaptic vesicle membrane (synaptotagmin). This triggers fusion of the vesicle with the presynaptic membrane, opening of the vesicle, and release of acetylcholine into the synaptic cleft. After transmitter release, the vesicle membrane is retrieved back into the presynaptic terminal and can be recycled to re-form a vesicle that is then refilled with acetylcholine synthesized in the cytoplasm. Certain bacterial toxins (e.g., botulinum, tetanus) can destroy the binding proteins involved in vesicle docking, ultimately interfering with the ability of the vesicle to release its contents into the synaptic cleft.
The Synapse
The Anatomy of the Neuromuscular Junction Is Specialized for One-Way Synaptic Communication
An Action Potential on the Presynaptic Neuron Triggers an Action Potential on the Muscle Cell Through the Release of Acetylcholine
< div class='tao-gold-member'>
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


The Synapse
Only gold members can continue reading. Log In or Register to continue