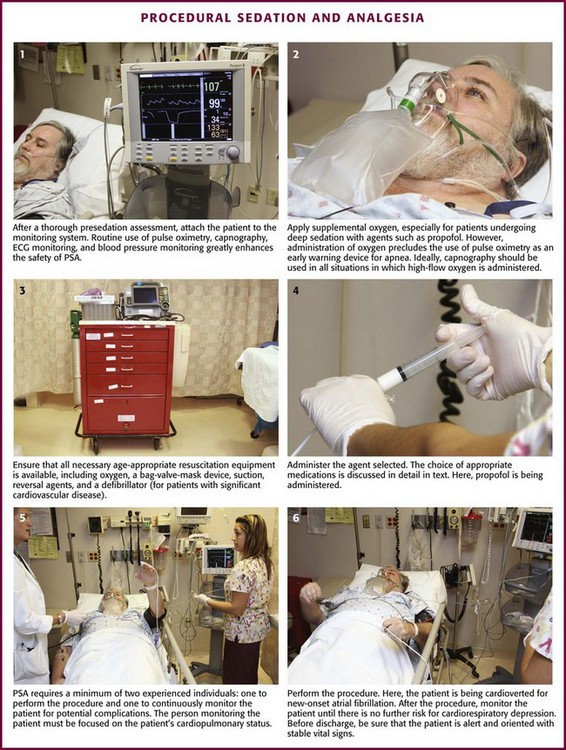
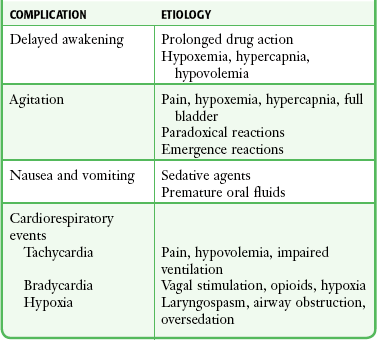
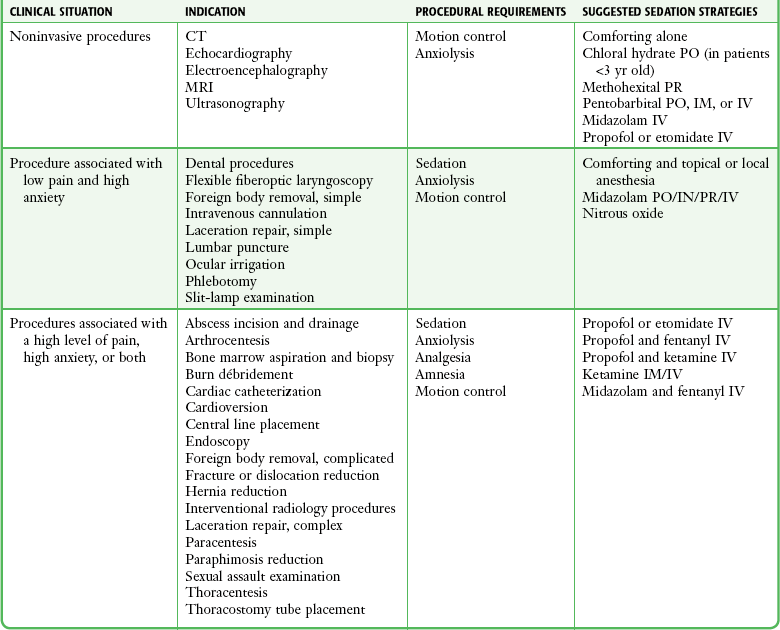
Chapter 33 Procedural sedation and analgesia (PSA) refers to the use of analgesic, dissociative, and sedative agents to relieve the pain and anxiety associated with diagnostic and therapeutic procedures performed in various settings. PSA is an integral element of emergency medicine residency and pediatric emergency medicine fellowship training and curricula, and graduates of these programs are skilled in the practice of PSA. Emergency clinicians are skilled in resuscitation, vascular access, and advanced airway management, which permits them to effectively recognize and manage the potential complications associated with PSA.1 In a recent study of all practitioners, the most common clinical errors associated with PSA were delayed recognition of respiratory depression and arrest, inadequate monitoring, and inadequate resuscitation,2 mistakes that are unlikely to be made by emergency clinicians. The safety of PSA techniques by emergency clinicians has been well documented in numerous series in both children and adults.3–7 Safe and successful application of PSA requires careful patient selection, customization of therapy to the specific needs of the patient, and careful monitoring of patients for adverse events. Emergency clinicians must ensure that all patients receive pain relief and sedation commensurate with their individual needs during any procedure. In 1985, the American Academy of Pediatrics (AAP) and the National Institutes of Health issued guidelines for the management and monitoring of children receiving sedation for diagnostic and therapeutic procedures in response to the growing use of opioids and sedative-hypnotic agents in the outpatient setting and a number of sedation-related deaths.8,9 In these documents, three levels of sedation were defined (conscious sedation, deep sedation, general anesthesia) to create a common language for describing drug-induced alterations in consciousness (Box 33-1).10,11 A key development in the field of PSA has been revision of the original terminology and adoption of clearer descriptions of varying types and degrees of sedation (see Box 33-1). Though historically popular, the widely misinterpreted and misused term “conscious sedation” has fallen into disfavor12; it has been labeled as “confusing,”13 “imprecise,”12 and an “oxymoron”12,13 and has been replaced with the term “moderate sedation.”10 Before the promulgation of PSA guidelines by specialty societies and governmental agencies, clinicians simply administered sedatives in varied clinical settings and used individual judgment to determine the need for specific monitoring devices and supporting personnel. Since 1985, at least 27 sets of PSA guidelines have been published,15 each crafted for the unique and differing settings in which PSA is practiced. Naturally, not all are in agreement.5 The intent of each of these guidelines is to better standardize the manner in which PSA is performed to enhance patient safety. Those most pertinent to emergency clinicians are from the American College of Emergency Physicians,3 the AAP,16 and the American Society of Anesthesiologists (ASA).14,17 In the early 1990s, the Joint Commission on Accreditation of Healthcare Organizations, an independent, not-for-profit organization that evaluates and accredits hospitals in the United States, took a special interest in PSA, with the central theme being that the standard of sedation care provided should be comparable throughout a given hospital. Thus, patients sedated in the emergency department (ED) should not receive a significantly different level of attention or monitoring than those sedated for a similar-level procedure in the operating room or in the endoscopy suite. To ensure this, the Joint Commission requires specific PSA protocols to be applied consistently throughout each institution. These hospital-wide sedation policies will vary from site to site based on the specific needs and expertise available within each institution. In 2001, the Joint Commission released new standards for pain management, sedation, and anesthesia care.10 At each hospital accreditation survey the Joint Commission determines whether practitioners practice PSA consistently with their hospital-wide sedation policy and whether they provide sufficient documentation of such compliance. Clinicians must be familiar with their hospital’s sedation policies and should work with their medical staff to ensure that such policies are suitably detailed, yet reasonable and realistic. Unduly restrictive policies do a disservice to patients by discouraging appropriate levels of analgesia and anxiolysis. Most hospitals pattern their sedation policies after the Joint Commission standards and definitions. It is important to note that the unique ketamine dissociative state does not fit into the existing Joint Commission definitions of sedation and anesthesia.11 A ready solution is to assign a distinct definition for “dissociative sedation” (see Box 33-1). The Joint Commission requires that PSA practitioners who are permitted to administer deep sedation be qualified to rescue patients from general anesthesia.10 Emergency clinicians typically perform all levels of sedation except general anesthesia. Moderate sedation suffices for the majority of procedures in adults and cooperative children, although it will not be adequate for extremely painful procedures (e.g., hip reduction, cardioversion). Deep sedation can facilitate such procedures, but with greater risk for cardiorespiratory depression than is the case with moderate sedation. Moderate sedation is frequently insufficient for effective anxiolysis and immobilization in younger, frightened children, and deep or dissociative sedation is an appropriate alternative. Assess the type and severity of any underlying medical problems. This is usually best documented by the standard ED medical record, history, physical examination, and nursing notes. Another tool used for this purpose is the ASA physical status classification for preoperative risk stratification (Table 33-1). Verify current medications and allergies. Inquire about previous adverse experiences with PSA or anesthesia. TABLE 33-1 ASA Physical Status Classification ASA, American Society of Anesthesiologists. From Krauss B, Green SM. Sedation and analgesia for procedures in children. N Engl J Med. 2000;342:938. Inspect the airway to determine whether any abnormalities (e.g., severe obesity, short neck, small mandible, large tongue, trismus) are present that might impair airway management. Consider assessments such as Mallampati scoring or the distance between the chin and hyoid bone (see Chapter 4, Fig. 4-3). Assess the time and nature of the last oral intake because pulmonary aspiration of gastric contents is a dreaded complication of vomiting when protective airway reflexes are impaired. Figure 33-1 shows a four-step assessment tool to stratify the risk for aspiration before sedation and to identify prudent limits of targeted sedation,18 although this tool has not yet been validated. Figure 33-1 Prudent limits of targeted depth and length of emergency department procedural sedation and analgesia based on presedation assessment of aspiration risk. (From Green SM, Roback MG, Miner JR, et al. Fasting and emergency department procedural sedation and analgesia: a consensus-based clinical practice advisory. Ann Emerg Med. 2007;49:454.) More conservative guidelines from the ASA for elective surgery or procedures in healthy patients specify an age-stratified fasting requirement of 2 to 3 hours for clear liquids and 4 to 8 hours for solids and nonclear liquids.19 Nonetheless, they acknowledge that regarding PSA, “the literature provides insufficient data to test the hypothesis that preprocedure fasting results in a decreased incidence of adverse outcomes.”14,17 The concept of preprocedure fasting is logistically difficult or impossible for emergency clinicians, who have no control over patients’ oral intake before arrival at the ED. In actual practice, emergency clinicians routinely perform PSA safely on patients who are noncompliant with the ASA elective-procedure fasting guidelines.18–20 Procedures can sometimes be delayed for a number of hours; however, this must be balanced against prolongation of pain and anxiety in the patient, inconvenience for the patient and family, and expenditure of room space and other finite ED resources. In addition, many ED procedures require urgent if not immediate attention (e.g., débridement and repair of animal bite wounds, acute burn management, arthrocentesis for suspected septic arthritis, reduction of joint dislocations, lumbar puncture in an uncooperative septic patient, hernia reduction, eye irrigation for ocular trauma or chemical burns, cardioversion in a hemodynamically unstable patient). Though uncommon, there may be occasions in which nonfasting patients require urgent procedures with a substantial depth of sedation that may be more safely managed in the operating room with endotracheal intubation to protect the airway. The most important element of PSA monitoring is close and continuous observation of the patient by an individual capable of recognizing complications of sedation (Fig. 33-2). This person must be able to continuously observe the patient’s face, mouth, and chest wall motion. Equipment or sterile drapes must not interfere with such visualization. Such careful observation allows prompt detection of adverse events such as respiratory depression, apnea, partial airway obstruction, emesis, and hypersalivation. During deep sedation, the individual dedicated to patient monitoring should have experience with this depth of sedation and no other responsibilities that would interfere with the advanced level of monitoring and documentation appropriate for this degree of sedation.16 Individual hospital-wide sedation policies may have additional requirements regarding how and when deep sedation is administered based on the patient’s specific needs and the clinician’s expertise. Capnography is a very useful tool that provides a continuous, breath-by-breath measure of the respiratory rate and CO2 exchange. Importantly, capnography can detect the common adverse airway and respiratory events associated with PSA.21–33 Capnography is the earliest indicator of airway or respiratory compromise and will show abnormally high or low end-tidal carbon dioxide pressure well before pulse oximetry detects falling oxyhemoglobin saturation, especially in patients receiving supplemental oxygen. Early detection of respiratory compromise is especially important in infants and toddlers, who have smaller functional residual capacity and greater oxygen consumption than older children and adults do.34–36 Capnography provides a non–impedance-based respiratory rate directly from the airway (via an oral-nasal cannula). This is more accurate than impedance-based respiratory monitoring, especially in patients with obstructive apnea or laryngospasm, in whom impedance-based monitoring will interpret chest wall movement without ventilation as a valid breath. Two recent randomized controlled trials have demonstrated that the use of capnography during procedural sedation decreases the incidence of hypoxic events.37–39 Both studies randomized patients to standard monitoring alone (oximetry, ECG, and blood pressure) or standard monitoring with capnography, with hypoxia being the outcome measure. In both studies, the addition of capnography to standard monitoring alerted clinicians to ventilatory abnormalities before the development of hypoxia, and as a result, capnography significantly decreased the incidence of hypoxic events.37,38 The bispectral index (BIS) is a monitoring modality that uses a processed electroencephalogram signal to quantify the depth of anesthesia or sedation. A BIS value of 100 (unitless scale) is considered complete alertness, 0 represents no cortical activity at all, and the range of 40 to 60 is believed to be consistent with general anesthesia. Although this technology has been used widely to monitor the depth of sedation in the operating room, the ASA has judged that its clinical applicability for this purpose “has not been established.”40 Furthermore, a 2011 study found that patients in whom a modified minimum alveolar concentration protocol (i.e., the inhalational anesthetic concentration needed for 50% of patients to not move with the application of a noxious stimulus) was used had fewer awareness events than did those in whom a BIS protocol was used.41 Even though PSA research has demonstrated statistical associations between BIS and standard sedation scores, these studies have also noted unacceptably wide ranges of BIS values at various depths of sedation.21,42–46 Thus, although BIS is correlated with the depth of sedation in aggregate groups, it lacks sufficient capacity to reliably gauge such depth in individual patients and therefore cannot currently be recommended for ED PSA. Substantial variation in practice exists with regard to the use of supplemental oxygen during PSA. The premise is a logical one—increasing systemic oxygen reserves should naturally delay or perhaps avert hypoxemia should an airway or respiratory adverse event occur. However, the price paid for this well-intentioned safeguard is the loss of pulse oximetry as an early warning device.12,15,21 Hyperoxygenated patients will desaturate only after the apnea is prolonged—indeed, the time required for preoxygenated, apneic, healthy adults and adolescents to desaturate to 90% averages more than 6 minutes.47,48 Deitch and colleagues have shown in a series of randomized controlled trials that high-flow supplemental oxygen decreases the incidence of hypoxia during propofol sedation (number needed to benefit of 4)49 whereas lesser amounts of oxygen (3 L/min) do so only marginally with propofol and not at all with lighter levels of sedation.23,50 Thus, high-flow oxygen is strongly recommended with propofol or other deep sedation, assuming that interactive monitoring includes capnography to promptly identify respiratory depression.51,52 For lighter levels of sedation, supplemental oxygen has no established benefit and may impair detection of respiratory depression when using pulse oximetry without capnography.52 Monitor all patients receiving PSA until they are no longer at risk for cardiorespiratory depression (Table 33-2). Before discharge be sure that patients are alert and oriented (or have returned to an age-appropriate baseline) with stable vital signs. Many hospitals have chosen to use standardized recovery scoring systems similar to those used in their surgical postanesthesia recovery areas (Table 33-3). Although no generally accepted minimum durations for safe discharge have been established, one large ED study found that in children with uneventful sedation, no serious adverse effects occurred more than 25 minutes after final medication administration.53 This suggests that in most cases, prolonged observation beyond TABLE 33-2 From Krauss B, Brustowicz R, eds. Pediatric Procedural Sedation and Analgesia. Philadelphia: Lippincott, Williams & Wilkins; 1999:145. TABLE 33-3 Sample Recovery Scoring Systems From Krauss B, Brustowicz R, eds. Pediatric Procedural Sedation and Analgesia. Philadelphia: Lippincott, Williams & Wilkins; 1999:157. Make sure that all patients leave the hospital with a reliable adult who will observe them after discharge for postprocedural complications. Document the name of the individual in the hospital record. Give written instructions regarding appropriate diet, medications, and level of activity (Boxes 33-2 and 33-3). Even though patients may appear awake and able to comprehend instructions, they may not remember details once they leave the ED. To be eligible for safe discharge, children are not required to walk unaided or demonstrate that they can tolerate an oral challenge because most PSA agents are emetogenic. Forcing fluids after sedation can lead to emesis before or after discharge. The AAP guidelines require only that “the patient can talk (if age-appropriate)” and “the patient can sit up unaided (if age-appropriate).”16 When infants and young children are discharged after their evening bedtime, caution parents to position the child’s head in the car seat carefully. Significant forward flexion might cause airway obstruction if the child falls asleep on the way home. Before drug administration, every effort should be made to minimize a patient’s anxiety and distress, particularly in children. The emotional state of a patient on induction strongly correlates with the degree of distress on emergence and in the days immediately after the procedure.54–57 Avoid being pressured by consultants to cut corners or rush PSA. Incorporating into the presedation preparation a discussion with the consultant about the sedation plan and the length of time required to safely prepare and sedate the patient can avoid the risks associated with hurried sedation. The oral, transmucosal (i.e., nasal, rectal), and IM routes are more convenient means of administration because IV access is not necessary, but they are much less reliable for timely dose titration to a desired response. New drug delivery systems, however, are expanding the effectiveness and ease of use of these routes of administration. The refinement of intranasal drug delivery has significantly increased the efficacy of this route of administration.58,59 Before the development of metered-dose atomizers, the degree of absorption and effectiveness of intranasal drug administration were operator dependent. Furthermore, new drug formulations with concentrations appropriate for intranasal administration are becoming available for study.60,61 The majority of nonpainful or minimally painful ED procedures in older children and adults can be performed without systemic sedation and analgesia. Skilled practitioners can frequently combine a calm, reassuring bedside manner with distraction techniques, careful local or regional anesthesia, or both.62–64 Many procedures, however, cannot be technically or humanely performed without PSA. These situations can be divided into three categories. Insufficient Analgesia.: Despite a cooperative patient, for some procedures it is impossible to achieve effective pain control with local or regional anesthesia. Examples of procedures requiring systemic PSA include fracture reductions, dislocation reductions, incision and drainage of large loculated abscesses, wounds that require scrubbing such as “road rash,” cardioversion, bone marrow aspiration/biopsy, and extensive burn débridement. Insufficient Anxiolysis.: Despite effective local or regional anesthesia, some patients will be so frightened that procedures cannot be technically or humanely performed without PSA. Young children requiring repair of lacerations are frequently terrified, and older children and adults may be highly anxious in anticipation of such repairs in sensitive or personal regions (e.g., face, genitalia, perineum). Insufficient Immobilization.: Despite effective local or regional anesthesia and anxiolysis, PSA may be indicated to prevent excessive motion during procedures that require substantial immobilization (e.g., repair of complex facial lacerations, diagnostic imaging studies). Immobilization is most commonly an issue with young children and the mentally challenged. General Considerations.: Clinicians must therefore base customization of their selection of drugs (e.g., anxiolysis, sedation, analgesia, immobilization) on the unique needs of the patient and their individual level of experience with specific agents (Table 33-4). A risk-benefit analysis should be performed before every sedation (Box 33-4). The benefits of reducing anxiety and controlling pain should be carefully weighed against the risk for respiratory depression and airway compromise. Factors influencing the extent of pharmacologic management are listed in Box 33-5. Some general drug selection strategies are discussed later and shown in Table 33-3. TABLE 33-4 Indications for PSA and Sedation Strategies* *There is no universally accepted or clinically correct dose, medication, or combination. Many regimens are acceptable. This table is intended as a general overview. Sedation strategies should be individualized. Although the pharmacopoeia is large, clinicians should familiarize themselves with a few agents that are flexible enough to be used for the majority of procedures. In all cases it is assumed that practitioners are fully trained in the technique, appropriate personnel and monitoring are used as detailed in this chapter, and specific drug contraindications are absent. Modified from Krauss B, Green SM. Sedation and analgesia for procedures in children. N Engl J Med. 2000;342:938. Minor Procedures In Cooperative Adults and Older Children.: Such procedures can usually be managed with topical, local, or regional anesthesia. Systemic PSA is typically unnecessary, although mild anxiolysis (e.g., nitrous oxide, oral midazolam) can make these patients more comfortable. More Complex Procedures of Longer Duration In Cooperative Adults and Older Children.: Supplementation of topical, local, or regional anesthesia with either nitrous oxide or IV midazolam and fentanyl permits customization of the depth of sedation and pain relief to the specific needs of each patient. Procedures In Uncooperative Adults or The Mentally Challenged.: Essentially all procedures in uncooperative adult-sized patients are difficult without systemic PSA. Depending on operator experience, IV midazolam, IV propofol, IV etomidate, or IM/IV ketamine or midazolam may be used in these situations. Given that the sedatives midazolam, propofol, and etomidate lack specific analgesic properties, many emergency physicians attempt to control pain with an opioid such as fentanyl before the procedure. Midazolam can be titrated intravenously to a relatively deep level of sedation, although as discussed previously, the risk for adverse effects increases with the depth of sedation. Ketamine (typically with coadministered midazolam when used in adults) can also provide the profound analgesia and immobilization necessary to perform painful procedures. However, in adults there is a risk for unpleasant hallucinatory recovery reactions. Ketamine should be used with extreme caution in older adults because its sympathomimetic properties may aggravate any underlying coronary artery disease or hypertension. Occasionally, procedures in extremely uncooperative adults or the mentally challenged are best managed in the operating room with general anesthesia. Minor Procedures In Uncooperative Older Children and In Young Children.: Minor procedures (e.g., small lacerations, IV cannulation, venipuncture, removal of superficial foreign bodies) in uncooperative children can frequently be managed by skilled practitioners with a combination of nonpharmacologic techniques (e.g., distraction, guided imagery, hypnosis, comforting, breathing techniques) in conjunction with topical anesthesia, careful local anesthesia, and when necessary, brief forcible immobilization (by personnel or a restraining device). In other cases, supplementing nonpharmacologic techniques with topical or local anesthesia and anxiolysis with oral midazolam may be sufficient to permit successful wound repair. Although oral administration is most popular and least invasive, the nasal or rectal routes can also be used depending on operator experience and preference.
Systemic Analgesia and Sedation for Procedures
Terminology
PSA Guidelines
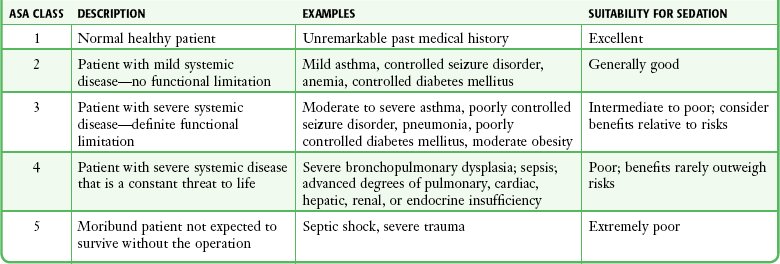
Evaluation before PSA
General
Airway
Gastrointestinal
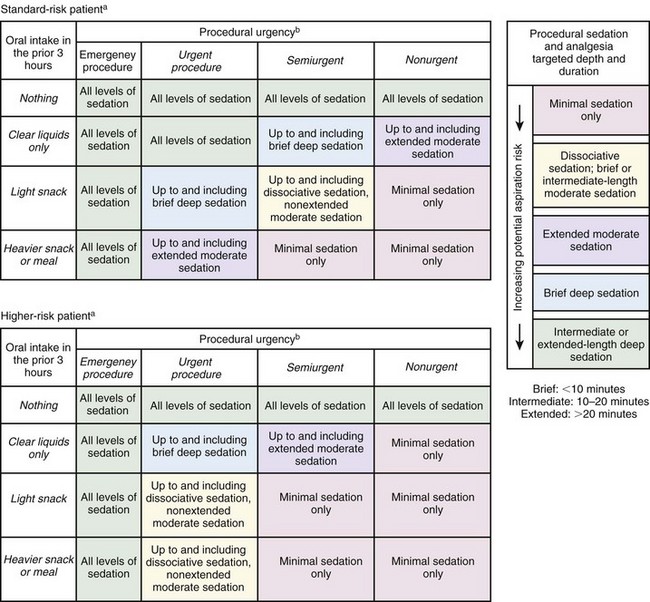
aHigher-risk patients are those with one or more of the following present to a degree individually or cumulatively judged clinically important by the treating clinician:
Personnel and Interactive Monitoring
Equipment and Mechanical Monitoring
Capnography
BIS Monitoring
Supplemental Oxygen
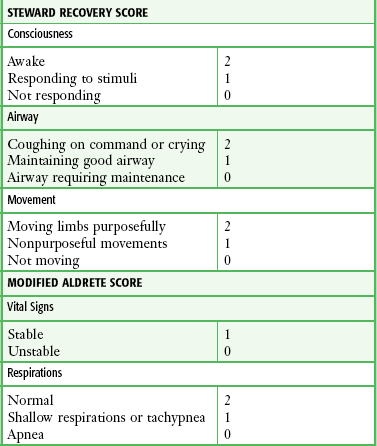
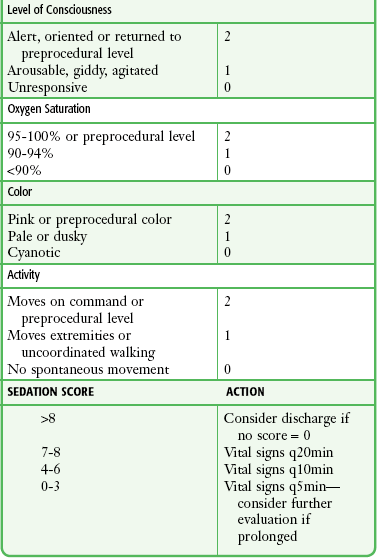
Discharge Criteria
 hour is unlikely to be necessary.
hour is unlikely to be necessary.
General Principles
Routes of Administration
Drug Selection Strategies
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree