27 Staphylococcal pyoderma
INTRODUCTION
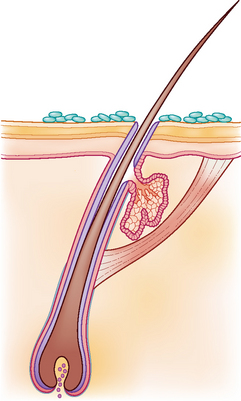
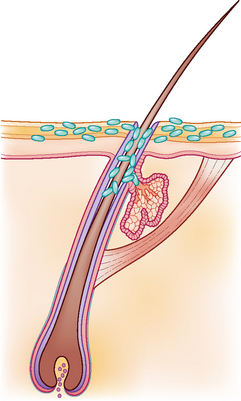
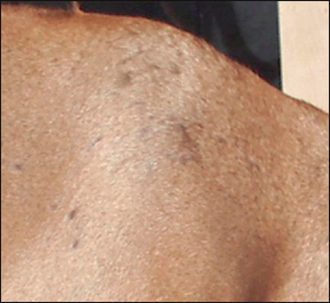
The majority of cases of canine pyoderma involve infection with resident bacteria, in particular, Staphylococcus intermedius, and arise because of an underlying systemic or cutaneous disease that renders the cutaneous microenvironment more favourable for bacterial proliferation and infection. Ectoparasitic disease, hypersensitivity disorders, endocrinopathies and primary scaling disorders are amongst the recognized underlying diseases. Some cases of canine pyoderma, however, are idiopathic. Pyoderma is classified as either surface, superficial or deep depending on the depth of infection. Surface infection is limited to the surface of the stratum corneum (Fig. 27.1), and includes intertrigo (skin fold dermatitis), pyotraumatic dermatitis (acute moist dermatitis) and some mucocutaneous pyodermas. Superficial infection involves the epidermis and/or the follicular infundibulum (Fig. 27.2), and includes impetigo, superficial folliculitis, superficial spreading pyoderma and some mucocutaneous pyoderma. Deep pyoderma involves all the portions of the hair follicle and the dermis (Fig. 27.3). This group includes deep folliculitis, furunculosis and cellulitis, German shepherd pyoderma and pyotraumatic folliculitis and furunculosis. In addition, localized deep infections are classified as: pedal pyogranulomas, or as nasal, muzzle, chin, callus and pedal folliculitis, or furunculosis. This case describes a case of superficial folliculitis, which is a common presentation in short-coated dogs and results in a characteristic moth-eaten appearance.
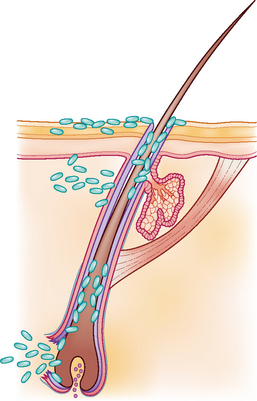
Figure 27.3 Diagrammatic representation of deep infections which can result in rupture of hair follicles.
CASE HISTORY
The level of pruritus in dogs with pyoderma varies from none to severe but dogs with an underlying allergic skin disease are usually pruritic. However, a ventral pyoderma in a young dog without a previous history of pruritus may be the first harbinger of the onset of atopic dermatitis. A history of a generalized scaling skin disease and possibly alopecia prior to the onset of more typical pyoderma lesions might suggest a primary seborrhoea or a genodermatosis such as colour dilution alopecia. The owner should be questioned regarding symptoms suggestive of systemic involvement. For example, lethargy and weight gain might suggest hypothyroidism, and polyuria, polydipsia and polyphagia should alert the clinician to the possibility of hyperadrenocorticism or diabetes mellitus. Owners may report that the dog’s skin is greasy and malodorous, especially when deep pyoderma is present.
In this case the relevant history was:
CLINICAL EXAMINATION
The relevant findings in this case were:
CASE WORK-UP
The history and clinical signs were suggestive of a pyoderma and, in general, the most convenient way to confirm bacterial involvement is on cytological examination (see Chapter 2).
The following diagnostic tests were performed:
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree