CHAPTER 205 Rattlesnake Envenomation
Rattlesnakes belong to the pit viper group of venomous snakes, which are responsible for most bites involving humans and small animals. There is no information on the relative frequency of rattlesnake bites in horses compared with that of other species of snakes, and there is only a small amount of literature describing the clinical signs, diagnosis, and treatment of rattlesnake envenomation in horses. Most of the therapeutic recommendations are based on anecdotal information, the results of only a few retrospective studies, and extrapolation from human or small animal medicine.
DIAGNOSIS
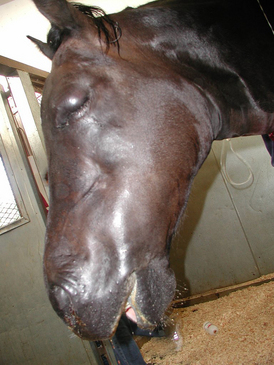
Rattlesnake bites are usually not challenging to diagnose. Differential diagnoses for local swelling and edema should be considered. The time of year, location of the swelling (frequently the muzzle), and identification of a bite wound are strongly supportive of the diagnosis (Figure 205-1).
An envenomation scoring system has been developed in human medicine, and a modification of this scoring system for horses is proposed in Table 205-1. The maximum score is 13 points, and horses should be reassessed every 6 hours. This scoring system was applied to a group of eight horses I treated for rattlesnake bite. Of those, all horses with a score less than or equal to 7 survived. Three horses with scores from 10 to 12 died or were euthanized because of clinical deterioration in the face of aggressive supportive treatment.
Table 205-1 Scoring System for Rattlesnake Envenomation∗
| System | Score† | Signs |
|---|---|---|
| Respiratory | 0 | Normal |
| 1 | Slight respiratory distress | |
| 2 | Respiratory distress with tachypnea and increased work of breathing | |
| 3 |