27 Proliferative (eosinophilic) keratoconjunctivitis
PRESENTING SIGNS
Proliferative (eosinophilic) keratoconjunctivitis occurs in cats (and horses) but not dogs.
CLINICAL EXAMINATION
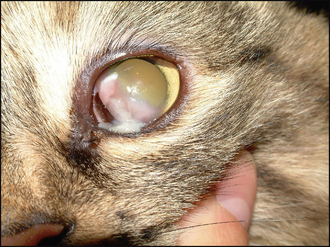
A pale pink mass, similar to granulation tissue, is seen extending across the cornea from the limbus. This is usually either at the temporolateral or ventronasal quadrant (Figure 27.1). The conjunctiva adjacent to the lesion is hyperaemic but no chemosis is usually present. A collection of white coloured tissue – almost globules or blobs – can be present on the surface of the pink mass, or adjacent to it. Some whitish discharge can accompany the signs. This looks similar to cottage cheese in consistency. There is normally corneal vascularization. Sometimes the nictitans membrane can be affected – particularly the bulbar side – so this should be examined. Ulceration is not usually a feature of the condition but care must be taken in interpreting fluorescein tests – the excess dye must be thoroughly flushed with sterile saline solution. Uptake of the green dye is quite possible on the pink fleshy tissue itself, often in tiny pinpoint patches, but not actually on the cornea – the epithelium usually remains intact.
If the condition is quite advanced, the pink tissue can extend all the way across the cornea and in these cases vision will be affected. The palpebral surface of the eyelids can be involved. Although normally initially unilateral, both eyes can be affected (especially in advanced or untreated cases) but usually to different degrees – the owner might have only been aware of one eye being abnormal but on careful ophthalmic examination it is discovered that the other eye has more subtle lesions (Figure 27.2).