57 Otitis externa and otitis media in a dog
CASE HISTORY
The relevant history in this case was as follows:
• A 3-year history of recurrent tick infestation, otitis externa and intermittent, non-seasonal papulocrustous eruptions over the axillae and groin.
• The dog had received frequent treatment with systemic and topical aural glucocorticoid and antimicrobial therapy, which resulted in an improvement, but the disease always recurred within weeks of treatment withdrawal. Topical antibacterials previously used included framycetin, fucidic acid, polymixin B, gentamycin, marbofloxacin and antifungals, including miconazole and nystatin.
• Over the past year, systemic prednisolone therapy had been more or less continuous in order to control pruritus, but had been withdrawn 4 weeks prior to examination.
CLINICAL EXAMINATION
• There was mild diffuse erythema of the muzzle and both external ear canals, with a bilateral purulent aural discharge (Fig. 57.1).
• Otoscopic examination was not performed at this stage because the ears were considered to be too painful.
• A papular eruption and mild scaling were evident over the flexural aspect of the left elbow, with the scaling extending distally over the anterior aspect of the left forelimb.
• Dorsal and plantar interdigital erythema and a greasy discharge were evident over all four feet (Fig. 57.2).
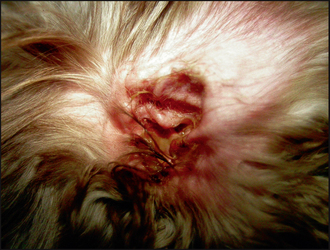
Figure 57.1 Pseudomonas otitis externa. Purulent aural discharge and erythema of the external ear canal are seen.
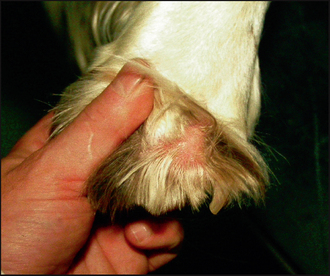
Figure 57.2 The same dog as in Fig. 57.1. Interdigital erythema due to Malassezia dermatitis can be observed.
CASE WORK-UP
• Cytological evaluation of aural discharge from the ear canals and from the tympanic bullae if there is evidence of otitis media.
• Full evaluation of underlying diseases, including blood work where necessary, diet trials, and intradermal and/or ELISA testing.
A diet trial, intradermal testing and blood work were indicated in this case and, as treatment of the otitis was likely to require glucocorticoid therapy, the decision was made to do intradermal testing at this stage.
The results of the work-up were:
• No evidence of ectoparasitism was found on microscopic examination of scale and deep skin scrapes from the pustular areas over the limbs.
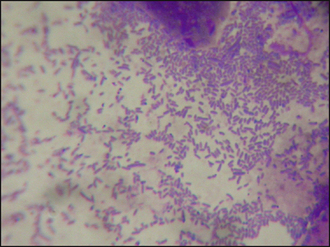
• Many rod-shaped bacteria were evident on cytological examination of the aural discharge (Fig. 57.3).
• A swab was taken from both horizontal ear canals for bacterial culture and sensitivity testing, which grew Pseudomonas aeruginosa resistant to all the topical antibacterials used, including fluoroquinolones, and sensitive only to ticarcillin in vitro.
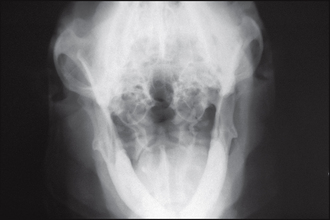
• Radiographic evaluation of the ear canals and tympanic bullae revealed ear canal stenosis of the proximal horizontal ear canals (Figs 57.4 and 57.5). There was no radiographic evidence of otitis media.
• Flushing and video-otoscopic examination of the ear canals under general anaesthesia revealed markedly erythematous and mildly ulcerated canals with no visible tympanic membranes. The ear canals were moderately stenotic.
• Samples for cytology and culture were collected from both tympanic bullae using a fine-tipped swab. Rods were seen on cytology, and culture and sensitivity testing grew Pseudomonas aeruginosa with a similarsensitivity pattern to the organism cultured from the horizontal canals.
• As prednisolone had been withdrawn 4 weeks previously, an intradermal test was performed that gave positive reactions to Dermatophagoides farinae, Dermatophagoides pteronyssinus and house dust.
• Routine haematological and biochemical examinations showed neutrophilia, lymphopoenia and elevated serum alkaline phosphatase, results consistent with previous glucocorticoid administration.
• Basal serum thyroxine concentration was 21 nmol/l. This was consistent with normal thyroid function.
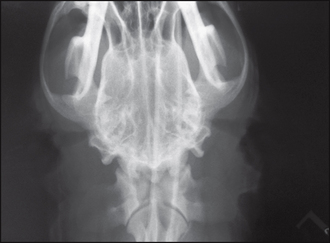
Figure 57.4 Ventrodorsal radiograph of the dog in Fig. 57.1. Stenosis of the proximal horizontal ear canals is apparent.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree