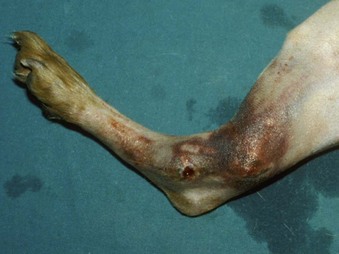
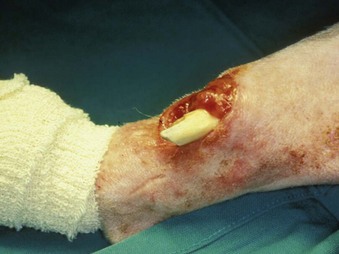
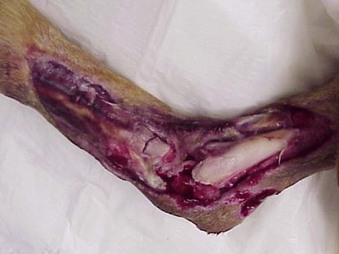
Chapter 42 An open fracture is one in which fractured bone is exposed to environmental contamination resulting from disruption of soft tissue integrity.31 Open fractures are typically the result of high-energy trauma such as from automobile accidents and most frequently involve bones with minimal soft tissue coverage, such as those of the antebrachium and crus.2 Complete and detailed assessment of the patient’s systemic health should be performed and resuscitation of the patient instituted as necessary before the fracture is evaluated. Oxygen saturation, electrocardiography (ECG), blood pressure monitoring, serum chemistry panel, complete blood count, and thoracic and abdominal radiographs are frequently indicated. Appropriate analgesics and, if required, intravenous fluid resuscitation, oxygen supplementation, and blood products are administered before musculoskeletal injury is addressed. Successful management of open fractures involves patient assessment, fracture classification, antibiotic therapy, debridement and irrigation, wound management, restoration of the soft tissue envelope, and fracture stabilization. Open fracture classification schemes describe the relationship and degree of soft tissue damage and are designed to correlate with treatment guidelines and prognosis (Box 42-1). Open fractures in human patients can be classified according to numerous methods; the most common is the Gustilo-Anderson classification scheme.58 The major shortcoming of this scheme is that it results in only moderate (60%) interobserver agreement.10,40 Ideally, a classification scheme should be simple, anatomically all-inclusive, and based on pathoanatomy, and it should focus on anatomic characteristics of the injury.58 The Orthopedic Trauma Association has proposed a new untested classification scheme (S1-3 M1-3 A1-3 B1-3 C1-3)58,79 that consists of five factors, including skin defect (S), muscle injury (M), arterial injury (A), bone loss (B), and contamination (C). They are divided into mild, moderate, and severe subgroups (1 to 3). This system provides much more precise pathoanatomic definition, and it encompasses the most essential categories for assessment of severity of open fractures.58 Such a classification system, if adopted, could help communicate patient status, guide treatment decisions, and predict prognosis. Open fractures in small-animal patients represent a unique combination of soft tissue and orthopedic injury. Successful management of open fractures prevents infection, promotes fracture healing, and restores function to the affected extremity. The keys to successful treatment include prompt and aggressive debridement of contaminated material and nonviable tissue, vigorous irrigation, administration of antimicrobials, and restoration of soft tissue coverage to healing bone, tendons, ligaments, and neurovascular structures.46 Preventing further contamination and soft tissue trauma is of utmost importance. A temporary sterile covering should be applied until proper debridement and irrigation can be performed. Copious amounts of sterile, water-soluble lubrication should be placed directly into the wound, and the hair should be clipped widely. Bordering skin is aseptically cleansed with a 4% chlorhexidine gluconate solution.45 Gross debris is removed, nonviable soft tissues are surgically debrided, and the wound is copiously lavaged with sterile isotonic fluid at a desired pressure of 7 to 8 psi. This can be accomplished with a 1-liter fluid bag placed with an external pressure sleeve and the pressure raised to 300 mm Hg.25 Alternatively, a 0.05% chlorhexidine solution can be an effective lavage solution, providing antibacterial activity without causing tissue reaction.1 A sterile dressing and bandage are applied with rigid external support to minimize pain and ideally to prevent propagation of soft tissue and orthopedic and neurovascular trauma until definitive surgical debridement and fracture stabilization can be performed. Once the patient has been stabilized, radiographic evaluation is performed to determine the precise orthopedic abnormalities. Significant debate has focused on the most appropriate method by which to manage open fractures. Open fractures have been considered one of the true orthopedic emergencies by some; however, optimal treatment for open fractures has not been definitively described in the scientific literature.31,61 Antibiotics are one required component of successful treatment. The importance of prompt initiation of intravenous antibiotics has been well documented.31,46,61,62 A prospective study of 1104 open fractures in human beings documented a significant decrease in infection rate when antibiotics were administered within 3 hours after injury (4.7%), compared with 4 hours or longer after injury (7.4%).61 The lowest infection rates are achieved when a combination of antibiotics, covering Gram positive and Gram negative aerobic and anaerobic organisms, is administered. Factors found to increase the risk of infection include lack of antibiotics, resistant organisms, too much time from injury to initiation of antibiotics, extensive soft tissue trauma, and a positive post debridement-irrigation culture.61 In a prospective study of 1025 open fractures in human beings, treating all open fractures with emergent surgical debridement, administering antibiotics before surgery, primarily closing type I and type II fractures with delayed closure of type III fractures, and using no internal fixation (use of external skeletal fixation preferred) resulted in significantly fewer infections (5%) when compared with historical controls (12%).31 The main shortcoming of this landmark study was the lack of independent variable analysis. Numerous more recent studies also acknowledge the importance of many factors toward achieving a successful outcome; however, early administration of broad-spectrum antibiotics is described by many to be the single most important factor in reducing infection.61,69,74 Infections of open fracture wounds are increasingly the result of pathogens acquired in a hospital setting. Unnecessarily maintaining an open fracture wound likely increases the rate of nosocomial infection.80 The authors of a prospective, randomized, double-blinded study found that only 18% of open fracture infections were caused by organisms cultured at the time of initial presentation.60 Numerous studies have demonstrated that the organism cultured initially (the contaminating organism at the time of presentation) is not the organism that ultimately causes infection.61,62,66 Hospital-acquired organisms play a prominent role in the development of infections in open fractures, many of which are resistant to numerous antibiotics.61 With these consequences in mind, early soft tissue coverage may aid in preventing disastrous complications. The time frame of “cleanest” may be that immediately following initial aggressive debridement and irrigation, presuming that debridement is adequate and no preexisting local infection is present. Systemic antibiotic(s) selected for initial treatment of an open fracture should be directed toward a wide range of Gram-positive and Gram-negative organisms.12,62 Bacteria frequently isolated from initial wound cultures include Staphylococcus spp., Streptococcus spp., Klebsiella spp., Pseudomonas spp., Clostridium spp., Enterobacter spp., and Escherichia coli.62,66,70 A randomized, double-blinded study of 171 open fractures in human beings treated with ciprofloxacin or the combination of a second-generation cephalosporin and gentamicin found no difference in infection rates of type I and type II fractures at 5.8% and 6%, respectively. The infection rate for type III fractures was significantly higher for the ciprofloxacin only group (31%) than for the cephalosporin/gentamicin group (7.7%).60 The degree of soft tissue compromise and increased contamination in type III fractures put them at higher risk for development of infection; therefore, they require broader antimicrobial coverage.60 Initial use of a first- or second-generation cephalosporin for type I and II fractures and the combination of a cephalosporin and a fluoroquinolone for treatment of type III fractures have been recommended to avoid the potential adverse effects of an aminoglycoside.60 Continuation of antibiotics, however, should be guided by results of aerobic and anaerobic cultures and sensitivities. Cultures acquired before surgical debridement can be predictive of subsequent organisms that may cause infection, especially in cases of delayed time to presentation.57,60 However, the decision to continue antibiotic therapy is best based on post–surgical debridement samples.52 Additionally, postdebridement samples aid in evaluation of the success of debridement and risk of subsequent infection.52,73 Implantation of antibiotic beads is a treatment option. The application of local antibiotics to severe open fractures has been shown to be a successful adjuvant for preventing the development of deep infection.9,37,59 The authors of a retrospective evaluation of 1085 open fractures in human beings concluded that combining antibiotic-impregnated polymethylmethacrylate beads with systemic antibiotics significantly decreased infection rates from 12% to 3.7%.59 In cases of open fracture, there is an obvious need to provide aggressive management, including antibiotic therapy, debridement, irrigation, and rapid stabilization. A historical dogma adopted by many physicians and veterinarians is that surgical debridement must be performed within 6 hours of the time of injury to have the best chance for a successful outcome.31,61 Prompt administration of antibiotics, thorough surgical debridement, and irrigation all play a vital role in reducing the likelihood of infection; however, no definitive evidence supports the need for surgical debridement within a specified time to prevent complications. Numerous studies of open fractures in human beings have demonstrated no significant difference in infection rates between patients receiving initial surgical debridement within 6 hours of injury and those undergoing initial surgical debridement longer than 6 hours after injury.35,52,69,71,74 These data certainly should not undermine the importance of prompt and thorough surgical debridement; however, time from injury alone should not be the definitive factor in surgical decision making or prognosis. Treatment decisions and prognosis of open fracture wounds should be based on assessment of soft tissue damage, viability, contamination, and infection—not on a time interval.
Open Fractures
Fracture Classification
Wound Treatment
Antimicrobial Therapy
Initial Surgical Debridement
Open Fractures
Only gold members can continue reading. Log In or Register to continue

Full access? Get Clinical Tree