CHAPTER 149 Non-neoplastic Nodular and Proliferative Lesions
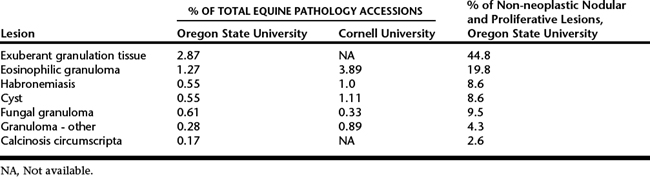
The differential diagnosis list for nodular cutaneous lesions in horses is long and includes both neoplastic and non-neoplastic diseases. A survey conducted at Oregon State University revealed that 8.7% of equine pathologic submissions were non-neoplastic nodular and proliferative skin lesions, and at Cornell University this type of lesion comprised approximately 11.8% of equine pathologic submissions.
The prevalence of non-neoplastic and proliferative lesions that are caused by infectious agents can vary according to geographic location, with variations related to climate, presence of infectious agents, and husbandry. However, comparison of survey information from Cornell University in the northeastern United States and from Oregon State University in the northwestern United States suggests that differences between these two regions are not dramatic (Table 149-1). Nodular non-neoplastic and proliferative lesions appear to be much less common in the skin of donkeys and mules than in horses. Only six cases of non-neoplastic lesions (four donkeys with exuberant granulation tissue, eosinophilic granuloma in a mule, and congenital papilloma in a mule) were identified in a study of 40 nodular and proliferative skin lesions in donkeys and mules at Oregon State University.
Table 149-1 Prevalence of Selected Non-neoplastic Nodular and Proliferative Lesions in the Northeastern
and the Northwestern United States
DIAGNOSIS
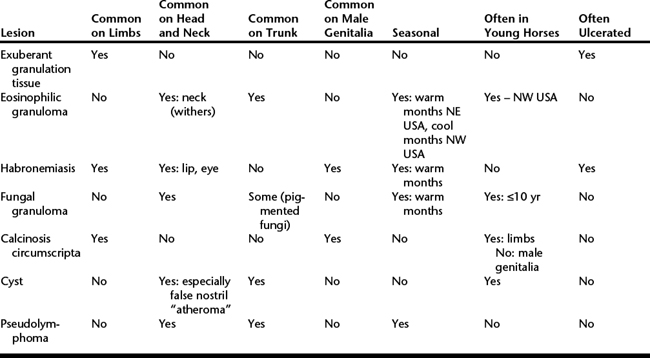
The primary differential diagnoses for persistent ulcerated lesions such as habronemiasis are squamous cell carcinoma, fibroblastic tumors (especially sarcoid), and melanocytoma. The differential diagnosis for nonulcerated nodular lesions is long and includes cutaneous lymphoma, melanocytic tumors, and benign epithelial tumors as well as a wide array of non-neoplastic disorders including eosinophilic granuloma, fungal granuloma, granuloma secondary to other causes, cyst, sterile panniculitis, and amyloidosis. In some instances, the age of the horse, location of the lesion, external appearance of the lesion, and season of occurrence can aid in diagnosis (Table 149-2). It is vital that this information be included in the history accompanying samples submitted for histologic assessment, as this will greatly aid the pathologist interpreting the sections. Cytologic evaluation of these lesions is not often diagnostic. In almost all cases, final diagnosis will rely on results of histologic evaluation. In instances involving multiple lesions, it is important to excise and submit more than one lesion, as it is possible for a horse to have cutaneous nodular lesions from more than one cause.
EXUBERANT GRANULATION TISSUE
Exuberant granulation tissue, so-called proud flesh, has no age, breed, or sex predisposition, and most commonly develops in wounds involving the lower portions of the limbs (Figure 149-1). This site predilection enables a tentative diagnosis to be made on the basis of history and physical examination findings in many instances. Exuberant granulation tissue is defined as cutaneous proliferative growth composed entirely of granulation tissue with no other underlying lesion. In the horse, sarcoid is a primary differential diagnosis. A prior history of a wound in the area is very useful in diagnosis of exuberant granulation tissue but is not available in all instances, and sarcoid can also develop at wound sites. Care must be taken to include deep areas during biopsy of any ulcerated proliferative lesion because this type of lesion, especially sarcoid, can include large zones of granulation tissue beneath the ulcerated surface. Exuberant granulation tissue was the most common non-neoplastic proliferative disorder diagnosed in donkeys in the Oregon State University survey.
EOSINOPHILIC GRANULOMA
These lesions are considered hypersensitivity reactions and are most common on the neck and dorsal aspect of the trunk. Eosinophilic granulomas are manifest as single to multiple, nonpainful, nonpruritic, firm nodules with normal overlying skin (Figure 149-2
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree