30 Lymphoma in a hamster
CLINICAL EXAMINATION
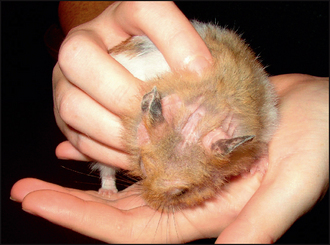
Dermatological examination revealed generalised erythema with multifocal areas of alopecia over the head and dorsum (Figs 30.1 and 30.2). There was also increased scaling of the skin in many areas. In addition, some erosions and excoriations were present on the face (Fig. 30.3).
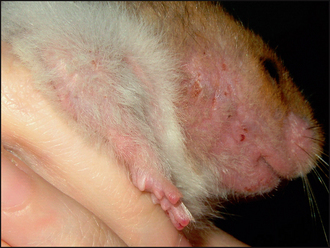
Figure 30.3 Facial alopecia, erythema and excoriation present on initial examination.
(Courtesy of N. Perrins.)
Demodicosis
Demodex is the most common ectoparasite of hamsters. They are susceptible to five different species, with D. aurati (in hair follicles) and D. criceti (in keratin and pits of the epidermal surface) being the most common (Fig. 30.4). Approximately 50% of hamsters may be asymptomatic carriers, so demonstration of mites in scrapings from healthy skin does not necessarily indicate disease. Clinical signs of demodicosis include alopecia, hyperkeratinization and scaling over the back, legs and abdomen. Pruritus is not usually a feature unless the infestation is complicated with a secondary infection. The presence of clinical signs invariably suggests an underlying disease, immunosuppression, stress or ageing. Diagnosis is made with skin scrapes, examined with light microscopy. The most effective treatment is amitraz (Aludex; Intervet) diluted to 100 ppm once weekly until 4 weeks after negative skin scrapes, although toxicity is a risk due to their small size and the difficulty of preventing grooming. Ivermectin injections (Panomec; Meriel) are useful (0.4 mg/kg subcutaneously) but will need repeating three or four times, or there is topical ivermectin (Xeno 450; Genetrix).
Dermatophytosis
This is relatively uncommon in the UK, but hamsters can be clinically affected, or asymptomatic carriers. The most common dermatophytes isolated are usually Trichophyton mentagrophytes or sometimes Microsporum canis; therefore, the disease is potentially zoonotic. Clinical signs include dry circular alopecic skin lesions, usually affecting the thoracic and abdominal areas, with the clinical disease often complicated by pyoderma. Diagnosis is made with standard fungal culture techniques (see the guinea-pig case in Chapter 10). Treatment is also very similar to other pets, although it can be challenging to stop the hamster licking after using topical antifungal drugs. Regular cleaning of the cage and use of proper bedding (avoid wood shavings – e.g. allergic dermatitis attributed to pine or cedar wood shavings has been reported) helps prevent this disease.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree