34 Gastric ulceration
The horse, as a non-ruminant herbivore, evolved to ingest a high-fiber, low-starch diet through daily (up to 18 h) foraging. Saliva produced in response to chewing helps to buffer gastric acid. Modern management practices including meal feeding, low-fiber/high-concentrate diets, early weaning and intensive training programs with limited opportunity for free movement increases the risk for development of a poorly buffered, acidic gastric environment. These feeding and management practices have been associated with a high prevalence of the equine gastric ulcer syndrome (EGUS) (Vatistas et al 1999a, Lester 2004, Jonsson & Egenvall 2006). EGUS is the term used to describe ulcers in the terminal esophagus, nonglandular stomach, glandular stomach and proximal duodenum (Hammond et al 1986). All ages and breeds of horses are susceptible to EGUS (Luthersson et al 2009a).
Epidemiology of equine gastric ulcers
Prevalence of EGUS varies in adult horses, with Thoroughbreds the predominant breed evaluated. In Thoroughbred racehorses in intensive training, the incidence of gastric ulceration has been reported to be more than 90% in some subpopulations. Severity of ulceration is greatest in animals in training and lesions tend to worsen in severity and number during the training period, particularly at the beginning (Hammond et al 1986, Murray et al 1989, 1996, Vatistas et al 1999a, Jonsson & Egenvall 2006). Prevalence of gastric ulceration in a group of Standardbred racehorses was reported to be 87% (Rabuffo et al 2002). Another study of Standardbred racehorses showed a prevalence of 70% graded as EGUS ≥1 or 42% graded as EGUS ≥2 (Jonsson & Egenvall 2006). Prevalence of gastric lesions in actively competing 3-day event horses was 75% (Michael Murray, unpublished data), 58% in show horses (McClure et al 1999), and 67% in endurance horses after competition (Nieto et al 2004). Although most studies on performance horses report high prevalence of gastric lesions, a prevalence of 40% was found in a group of 156 Western performance horses under heavy use (Bertone 2000). Western performance horses may have fewer lesions due to differences in their management, training and feeding compared to the other groups of horses.
Only a few studies have been carried out on leisure horses and breeding mares. In a post mortem study of retired racehorses, 52% had lesions compared with 37% of pleasure horses (Murray et al 1996). In a study of 80 horses involved in a university riding program, there was a low prevalence of 11% (Chameroy et al 2006). In a study of 201 Danish pleasure/leisure horses 53% (107/201) were graded as having EGUS ≥2 (Luthersson et al 2009a). In a group of pregnant and nonpregnant mares (62) on pasture, an overall prevalence of gastric ulcers was 71% (Le Jeune et al 2009).
Limitations, when comparing studies of EGUS prevalence, include variations in the classification of the ulcers included (in particular the severity level), the number of animals investigated and how the lesions were graded. Slightly different scoring systems have been used in the literature to describe the ulcers. MacAllister et al (1997) reported on both the number of lesions (0–4) and their severity (0–5), whereas Furr and Murray (1989) combined the two to give an overall score value of 0–4. In a study of show horses (McClure et al 1999), the authors used a 0–6 system whereas the EGUS Council Scoring system (Andrews et al 1999) uses a 0–4 system. These differences can significantly affect the prevalence estimates of clinically relevant ulcers, since lower grades of gastric lesions, which reflect minor pathologies such as hyperkeratosis, may or may not be included in the definition of an ulcer. Additionally, some reports include all grades of lesions, while others define clinically significant ulcers and report on their prevalence e.g. ≥ grade 2 according to Luthersson et al in the Danish study (2009a).
Anatomical distribution of gastric ulcers
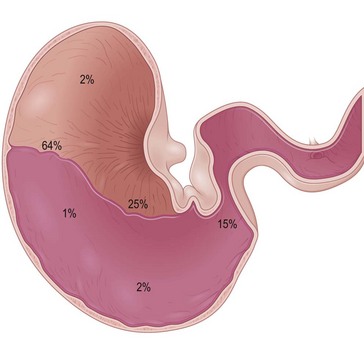
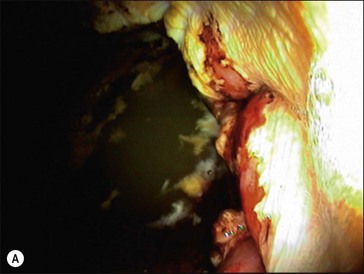
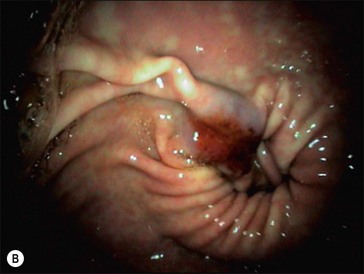
Ulcers have been identified throughout the stomach. The nonglandular stratified squamous mucosa along the margo plicatus is most commonly affected (Hammond et al 1986, Murray et al 1989, 1996). Prevalence of glandular mucosal lesions is slightly lower than for the squamous lesions, with the pyloric antrum most commonly affected, as illustrated by the Danish study (Luthersson et al 2009a). Ulcerations in the two main regions (squamous or glandular mucosa) might have different etiologies and therefore risk factors. It is the authors’ opinion that horses often develop lesions in either the non-glandular or the glandular part of the stomach depending on their “environment”. Glandular lesions may be missed by poor endoscopic technique; therefore, the incidence of pathology in this part of the stomach may be greater than previously reported (Andrews et al 2002). Current information on the prevalence of glandular ulcers is limited, but a study of 201 horses showed that 168 horses had visible ulcers (grade 1 and above). Of these, 29 had glandular lesions only, 53 had non-glandular lesions only and 86 had lesions in both regions of the stomach (Luthersson et al 2009a). The most severe lesions in each region were located as shown in Fig. 34.1. Examples of non-glandular and glandular lesions are depicted in Fig. 34.2.
Key Points –
Prevalence of EGUS
• In performance horse populations, the reported prevalence of gastric ulceration has ranged from 40% to more than 90%. Few studies have examined EGUS prevalence in leisure and breeding horses
• The nonglandular stratified squamous mucosa along the margo plicatus is the most common site for ulcer lesions
• Severity of lesions is greatest in horses in athletic training; an increase in lesion number and/or severity during training has been reported in Thoroughbred racehorses
Risk factors and pathophysiology
Risk factors for non-glandular and glandular lesions may differ. Lesions in the squamous mucosa mostly reflect peptic injury (HCl and pepsin) to the poorly protected surface of the non-glandular part of the stomach. The primary barriers to HCl in the squamous epithelium are intracellular secretion of bicarbonate ions and the intracellular tight junctions (Orlando 1991, Tobey & Orlando 1991, Orlando et al 1992). These tight junctions are located in the superficial layer of the epithelium, but they only provide a weak barrier as deeper in the epithelium, the cells transport hydrogen ions intracellularly, resulting in their death when exposed to HCl (Tobey & Orlando 1991). Since there is no surface barrier to HCl and the epithelium has limited ability to prevent peptic injury, there is a limited primary barrier to peptic injury, and prevention effectively relies on limited exposure to acidic gastric secretions (Murray 1999). The glandular mucosa’s epithelial cells, through a buffering layer of mucus containing bicarbonate, are protected from direct contact with low pH in the gastric juice. Glandular lesions are thought to result from impaired mucosal defense mechanisms rather than a primary peptic injury. This is supported by the observation that feed deprivation models used to create squamous injury do not produce glandular lesions. Also, when assessing the effect of exercise, only a few glandular lesions were found (Lester et al 2004, Jonsson & Egenvall 2006). Glandular lesions can be successfully induced in horses using excessive administration of nonsteroidal anti-inflammatory drugs (NSAIDs) and there is increasing evidence of a bacterial component to glandular ulcer development (Contreras et al 2007, Reed et al 2006). It might therefore be more relevant to divide EGUS into two distinct types: primary squamous ulceration due to increased acid exposure and primary glandular ulceration resulting from failed mucosal defences. Future studies should therefore describe the location of EGUS lesions and analyze non-glandular and glandular EGUS independently to enable the identification of unique risk factors for each anatomical type of lesion.
Age, breed, gender
Age has been identified as a risk factor in some studies. Some studies showed that risk was highest in younger horses, aged 2–6 years (Chameroy et al 2006), while other studies have shown that the risk increases with age (Rabuffo et al 2002). The latter study and its findings relate to racehorses in training and therefore perhaps only reflect a particular age range and use of horses. A study performed on leisure horses showed no association between age and risk of EGUS, nor any effect of breed or gender (Luthersson et al 2009b).
Exercise
Workload has been suggested to be one of the most important risk factors for EGUS. Recent work suggests that horses in light to heavy training for as short as 8 days may be at risk of developing gastric ulcers (White et al 2007). Furthermore, a study in Australia suggested that prevalence in racehorses increased 1.7 times for every week of training (Lester et al 2007). In an earlier study, horses running on a high-speed treadmill showed increased abdominal pressure and decreased stomach volume compared with resting values. It was suggested that contraction of the stomach during exercise allowed acid from the glandular mucosa to reflux up into the nonglandular mucosa resulting in injury to the relatively unprotected nonglandular mucosa – the “acid-splashing” hypothesis (Lorenzo-Figueras & Merrit 2002). Additionally it was found that gastric pH decreased rapidly to < 4 at the beginning of walking, continued to decrease during trotting and galloping, and remained low until the horses returned to a walk. Less marked changes were seen in animals that had been fed prior to being exercised. Horses in intensive training programs are exposed to a longer daily duration of more intense exercise and therefore, potentially an increased duration of acid exposure, possibly contributing significantly to the risk of gastric ulceration. However, all types of work do not necessarily increase the risk of gastric ulcers. A study of pleasure/leisure horses in Denmark showed no apparent effect of workload on the risk of EGUS. None of the animals evaluated were racehorses and even if they were used for equestrian training and competition (dressage or show jumping) exercise workload was less than that of a typical racehorse. This could indicate that only strenuous exercise results in acid injury of the non-glandular mucosa. However, an alternative explanation could relate to the association between starch intake and risk of EGUS (see below). Racehorses typically receive increased amounts of dietary starch in association with increased workload.
Fasting
Horses are continuous but variable gastric acid secreters, and feeding state affects the pH of gastric juice. When feed is withheld from horses before racing or due to the feeding regimen, gastric pH drops rapidly and the nonglandular mucosa is exposed to an acid environment (Vatistas et al 1999b). The pH of gastric juice in horses from which feed was withheld for several hours was 2.0 or less (Murray 1992). In horses fed free-choice timothy hay for 24 hours, mean gastric pH was significantly higher than in fasted horses (3.1 in hay fed vs. 1.5 in fasted) (Murray & Schusser 1989). Intermittent feeding has been shown to both cause and increase the severity of gastric ulcers and has been developed as a reliable model for induction of EGUS (Murray 1994, Murray & Eichorn 1996). Gastric ulceration was induced by alternating 24 hours periods of feed deprivation and ad libitum access to hay, for a total of 96 hours of feed deprivation. The result of this feeding protocol was erosions and ulceration of the nonglandular mucosa of each horse in this study. The non-glandular mucosa, as discussed above, is the most susceptible to this protocol due to its lack of mucosal protective factors.
Pasture turnout
Grazing horses, in general, appear to have a decreased prevalence of EGUS (Murray et al 1989, Hammond et al 1986). Due to a continuous flow of saliva and ingesta, stomach acid is buffered, with pH ≥ 4+ for a large portion of the day (Husted et al 2008). In Thoroughbred racehorses in training, horses with access to some turnout were less likely to have ulceration, and this risk was even lower if they were turned out with other horses (Lester et al 2007). Within seven days, squamous mucosal lesions were induced when horses were taken from pasture to stall confinement with free choice timothy hay and no training (Murray & Eichorn 1996).
Pasture turnout is considered to be advantageous in many reviews but in one study of 62 broodmares (33 pregnant and 29 nonpregnant) kept under similar management on pasture (no details of feeding program given) there was a relatively high ulcer prevalence of ~67% in the pregnant mares and ~76% in the non pregnant mares (Le Jeune et al 2006). This apparently high incidence may reflect dietary management. Additionally there was no effect on intragastric pH of horses housed in a grass paddock, a stall on their own or in a stall with an adjacent companion when fed ad libitum grass hay and grain twice a day (1 kg/100 kg/day), suggesting that housing may not affect gastric pH and that being in a paddock may not provide any benefit (Husted et al 2008). The study of Husted et al (2008) focused only on pH as the primary ulcerogenic factor, whereas other factors might be associated with ulceration. The amount of starch given to each horse per day, for example, was not described. As described below, a high intake of starch may enhance the influence of a low pH by compromising squamous mucosal integrity.
Starch intake
Starch/grain intake has been associated with an increased risk of EGUS in horses. Frank et al (2005) noted a marked increase in ulceration when nonexercising animals were stabled and fed grain at 1% of body weight (BW) (3.7 to 5.1 kg of grain per mare once daily), 1 hour before hay was fed. The remainder of the dietary requirement was met by feeding grass hay. The diet was designed to provide 1.5 times the digestible energy (DE) requirement for maintenance. Exceeding 2 g/kg BW of starch intake per day was associated with an approximately twofold increase in the likelihood of EGUS (severity grade ≥ 2 [out of 5]) and feeding more than 1 g/kg BW of starch per meal was associated with a 2.6 times increase in the likelihood of EGUS ≥ 2 in the non-glandular part of the stomach (Luthersson et al 2009b). In this population, starch intake was independent of workload and as increased level of work was not associated with increased risk the influence of starch on risk of gastric ulcers was significant. The influence of starch on ulcer risk was greatest for nonglandular mucosal lesions.
Vatistas et al (1999b) observed development of ulcers in horses within 14 days of their removal from pasture, stabling (fed 6 kg concentrate feed/day) and entering a simulated training regimen. In another study, dams were supplied with concentrate feed and foals were allowed to eat their dam’s food. When more concentrate feed was fed to the mares, lesions in the squamous mucosa were more prevalent and more severe (Taharaguchi et al 2004).
The stomach of the horse has a large, diverse population of microflora when the horse is fed a diet rich in starch or non-structural carbohydrates. The bacteria found in the stomach of the horse include Streptococcus bovis, Streptococcus equinus, Lactobacillus salivarius, L. mucosae, L. delbrueckii, and Mitsuokella jalaludinii (Al Jassim & Andrews 2009). Volatile fatty acids (VFAs) are produced when carbohydrates are fermented by the microflora within the gastrointestinal tract. VFAs (including acetic, butyric, propionic, and valeric acids), produced by the fermentation of starch/sugar by the gastric microflora, have been shown to reduce mucosal integrity and affect mucosal tissue bioelectric properties (Andrews et al 2006, 2008, Nadeau et al 2003a, b). An in vitro study found that acetic, butyric and propionic acids caused a decrease in barrier function of the squamous mucosa (Nadeau et al 2003a, b). This effect is due to the lipid solubility of these VFAs at pH ≤ 4.0, resulting in VFAs penetrating cells in the non-glandular gastric mucosa, acidifying the cellular contents, inhibiting sodium transport and leading to cellular swelling. Andrews et al (2006) also found that squamous mucosal cells are susceptible to VFA injury in a pH (increased injury with lower pH), dose (higher the dose, greater the damage), and time (longer the tissue is exposed the greater the damage) dependent manner. When the nonglandular gastric mucosa was exposed to lactic acid, tissue permeability was increased but sodium transport was not affected.
Forage feeding and type of forage
When fed hay and pasture, horses produced 400–480 g saliva per 100 g dry matter consumed whereas when a concentrate was fed, horses produced approximately half the amount of saliva (206 g saliva per 100 g dry matter consumed; Meyer et al 1985). This would be expected since chewing stimulates saliva production, and horses spend more time chewing forage than they do concentrate feeds. One theory is that saliva produced in sufficient quantities will contribute to the buffering of gastric acid. Without this salivary buffering effect, damage to the gastric mucosa is more likely to occur and lesions (gastric ulcers) may develop.
Free access to fibrous feed (grass or digestible forage) or frequent forage feeding may therefore help reduce the risk of gastric ulceration. Feeding alfalfa hay and grain, however, resulted in higher gastric pH and less peptic injury to the gastric squamous mucosa than feeding bromegrass hay or coastal Bermuda hay with no grain (Nadeau et al 2000, Lybbert et al 2007). This suggests that forage type may also be important. In a recent study (Luthersson et al 2009b
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree