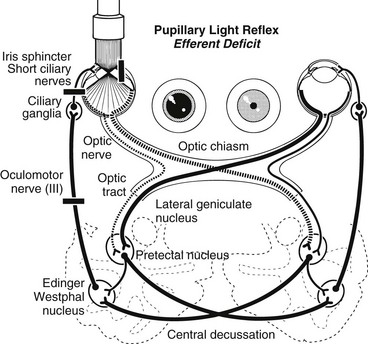
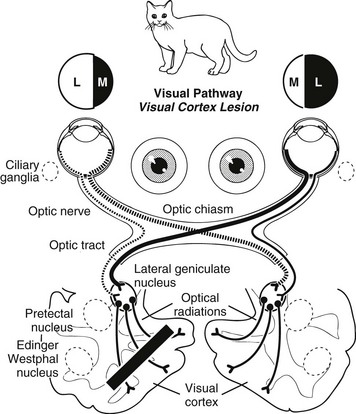
Chapter 243 Evaluation of a patient brought to the veterinarian because of vision deficits or blindness can be a diagnostic challenge. Both ocular and neurologic causes must be considered. As with central nervous system disease, localization of an ophthalmologic lesion is imperative to formulate the differential diagnoses, diagnostic approach, and therapeutic plan, and to advance a prognosis. This chapter, in conjunction with Web Chapter 80 on the neuro-ophthalmic examination, provides a blueprint for the assessment of a blind patient. Once the history has been obtained, the pet’s behavior and confidence navigating around the clinic and examination room should be assessed. Additional methods of assessing vision include menace response testing, cotton ball tracking, visual placing, maze testing, evaluation of the pupillary light reflexes (PLRs), and assessment of dazzle responses (see Chapter 242). Electroretinography, although it does not directly assess vision, also may be useful for assessing retinal function. It is important to evaluate the vision in each eye independently as well as to assess the visual fields of each eye. Visual fields are assessed by covering one eye and checking menace responses in the other by advancing a fist toward the tested eye from both the nasal and the temporal sides of the globe. Baseline pupil symmetry, the presence or absence of anisocoria, and the PLRs should be evaluated in both a brightly lit and a dimly lit room and the findings recorded. Any abnormality of the PLRs should be characterized (ranging from a mild decrease to complete absence) and qualified as an afferent or efferent deficit. Afferent PLR deficits are associated with vision deficits. The pupillomotor fibers split off from the optic tract just before the lateral geniculate nucleus; therefore lesions involving the Edinger-Westphal nucleus (the parasympathetic nucleus of cranial nerve III) and the efferent arm of the PLR pathway are not associated with loss of vision (Figure 243-1). Lesions that involve the visual pathway from the lateral geniculate nucleus to the optic striations in the visual cortex do not cause abnormalities of the PLR or anisocoria (Figure 243-2).
Evaluation of Blindness
Assessing the Patient
< div class='tao-gold-member'>
Evaluation of Blindness
Only gold members can continue reading. Log In or Register to continue

Full access? Get Clinical Tree