(1)
CNRS U MR5227 Laboratoire Mouvement Adaptation Cognition, Université Bordeaux 2, Bordeaux, France
(2)
Université Bordeaux 1, Bordeaux, France
Abstract
Among the different behavioral criteria used to discriminate substance dependence (or drug addiction) from other non-disordered forms of drug use, drug intake escalation presents a number of unique features that makes it particularly suitable for modeling in nonhuman animals. This criterion has stood the passage of time despite major revisions of diagnostic systems, it is common to all known drugs of abuse and it can be readily and unambiguously operationalized in laboratory animals. Here I exhaustively review evidence showing that escalation to heavy consumption of different drugs (except perhaps nicotine) can be rapidly induced in the majority of individual animals (i.e., rats) by increased drug availability. Such an escalation of drug use is probably paralleled by an authentic escalation to drug addiction, as it is associated with the co-occurrence of other addiction-like changes (i.e., increased motivation for drug use; increased difficulty to abstain from drug use; decreased sensitivity to negative consequences). In addition, during escalation of drug intake, most individual animals become increasingly responsive to drug- and stress-primed, but apparently not cue-primed, reinstatement of drug seeking after extinction. Finally, following increased drug use, most individuals present selective cognitive dysfunctions (e.g., deficits in executive functions) that may contribute to the establishment and/or persistence of addiction. Thus, the study of individuals with escalating patterns of drug use should provide a unique and valid approach to investigate, experimentally, the behavioral and neurobiological mechanisms that underlie the progression to addiction.
Key words
CocaineHeroinNicotineToleranceCompulsionSelf-regulationRewardPunishment1 Introduction
Psychiatrists have long been, and still are, striving to fine-tune their diagnostic criteria to distinguish substance dependence or drug addiction from other, non-disordered forms of substance use (1–4). Such a distinction has just begun to be imported into research on animal models of addiction (5–12). It is now acknowledged by a growing number of researchers that mere drug self-administration and/or drug reinforcement (i.e., in Skinnerian terms, the process by which a drug acts as a response-contingent stimulus that increases and/or maintains responding) is no longer sufficient evidence for an addiction-like profile in nonhuman animals. Animal “drug users” must also develop or present other behavioral signs to be considered a valid model of addicted humans. Among the different behavioral criteria of substance dependence that have been considered, escalation of drug use presents a number of unique features that makes it particularly suitable for modeling in nonhuman animals. It is indeed one of the rare behavioral criteria of dependence that has remained unchanged across successive revisions of diagnostic classifications (and thus probably has the least chance to be modified in future revisions), it is common to all known drugs of abuse and, finally, it can be readily and without ambiguity operationalized and induced in laboratory animals. In fact, as argued below, escalation to heavy drug consumption is probably an authentic escalation to addiction (or dependence), as it is associated in the majority of animals with the co-occurrence of other addiction-like changes. The study of individuals with escalating patterns of drug use should thus provide a unique and valid approach to investigate, experimentally, the behavioral and neurobiological mechanisms that underlie the progression to addiction.
2 Escalation of Drug Consumption as a Hallmark of Addiction
Drug intake escalation can be defined as a progressive increase in individual drug consumption over time that becomes excessive, overwhelming, and difficult to control. Everything happens as if drug use begets further drug use, a phenomenon dubbed “adjacent complementarity” by prominent economists interested in addictive behaviors (13). There is a large and long-standing consensus across many scientific disciplines for considering escalation of drug consumption as a core feature of addiction or even as constitutive to this behavioral disorder. There are several reasons for this consensus. First, it is simply difficult to conceptualize the transition to addiction without postulating a progression toward heavy drug use. For instance, it would be odd to speak of tobacco addiction in so-called tobacco “chippers” who continue to smoke a few cigarettes a week as during their first encounters with cigarettes (14). Indeed, without escalation to exaggerated levels of drug use, there would be no harm (except those accidentally caused by acute intoxication) and no motivated attempts to stop or to reduce drug use. Second, escalation of drug use is one of the few diagnostic criteria common to all known forms of addiction, including addictions that involve licit or illicit drugs and so-called behavioral addictions that do not involve a substance (e.g., pathological gambling). In contrast, other symptoms of addiction are specific to some drug categories and/or legal status (i.e., licit or illicit). For instance, the criterion “a great deal of time spent in activities necessary to obtain the substance, use the substance or recover from its effects” is not currently applicable to tobacco addiction, though this will probably change with the application of more strict regulation (15). Finally, among the different behavioral criteria being used to define or diagnose addiction, as opposed to recreational drug use or drug abuse, escalation of drug intake has stood the passage of time despite several successive major revisions in diagnostic classifications. This formidable resistance to change suggests that this criterion is unlikely to change in future diagnostic revisions, except perhaps to further increase its operationality (4).
3 Escalation of Drug Consumption Is Not a Surrogate of Tolerance
To prevent confusion, it is important from the outset to establish a clear conceptual distinction between escalation of drug use and drug tolerance. For historical reasons, drug intake escalation has always been associated with drug tolerance in diagnostic systems. In fact, escalating drug use is often presented as one of the definitions of, or a surrogate for, drug tolerance. In the current edition of the Diagnostic and Statistical Manual for Mental Disorders (DSM), tolerance is defined as either a “markedly diminished effect with continued use of the same amount of the substance” or a “need for markedly increased amounts of a substance to achieve intoxication or desired effect” (3). However, as defined above, escalating drug use is an individual behavioral process that can and should be conceptually separated from pharmacodynamic tolerance (16). Indeed, depending on the theoretical framework considered, one can conceive of a wide array of different underlying mechanisms – not necessarily mutually exclusive. Certainly, under some conditions, escalation of drug use can directly arise from tolerance to some of the effects of the drug (e.g., tolerance to the drug’s rewarding or aversive effects) brought about by molecular adaptations within drug receptor signaling pathways and other cellular mechanisms. However, many alternative mechanisms operating at different, higher levels of neurobiological organization can also be envisioned. Here is a short, certainly not exhaustive, list of potential mechanisms that could account for escalating patterns of drug use. First, within an affective self-medication or self-regulatory framework, drug use is maintained by relief of a preexisting affective condition. Escalation of drug use then arises, not because the drug progressively loses its efficacy in ameliorating the affective condition, but because this condition worsens with extended drug use, either as a direct or indirect consequence of drug use (e.g., through “reward allostasis” or “disuse atrophy”) (16, 17). Second, in a multisystems learning framework, escalation of drug use could result from a shift from goal-directed to habitual drug-taking behavior (18). Specifically, goal-directed drug use is intrinsically limited by deliberation over potential alternative courses of actions. With extended experience, however, drug use becomes habitual and thus less limited by time-consuming deliberative decision-making processes. One can predict, however, that such a mechanism will only account for drug intake escalation in stationary and highly predictable environments (e.g., drug self-administration chambers for laboratory animals). In more variable, uncertain environments that require strategic decision-making, such a mechanism is unlikely to be recruited. Third, in a behavioral economics framework, drug consumption is influenced by microeconomic factors, including drug availability, prices and accessibility to substitutes or alternative commodities (19). Thus, escalating drug use can result from increased drug availability, decreased drug price and/or reduced accessibility to nondrug substitutes. Finally, from a psychosocial perspective, drug use is limited in a specific society or culture by cultural norms, taboos, and/or overarching value systems (20). Here escalation of drug consumption can result from a progressive loss of influence of prevailing social or cultural norms on drug taking due, for instance, to social exclusion or marginalization processes that are directly or indirectly related to drug use. Within the same framework, escalating drug use can also arise from a progressive depletion in the individual’s social capital brought about by extended drug use. Thus, to sum up, the historical link established between drug intake escalation and tolerance has no apparent conceptual necessity. It is an empirical question to determine whether escalation of drug use is more often than not driven by drug tolerance and/or other mechanisms. In the remaining text, I will focus on drug intake escalation as a behavioral process without theoretical commitment to a specific underlying mechanism.
4 Experimental Induction of Drug Intake Escalation
As suggested above, several different factors can precipitate – at least in principle – escalation to higher levels of drug consumption. Despite such potentially diverse etiology, however, research on laboratory animals (i.e., rats) has so far been limited, mainly, to investigating the role of increased drug accessibility in promoting the progression toward excessive drug use (see Sect. 9, for additional information regarding this limitation). Specifically, escalation of drug consumption is induced reliably and rapidly by increasing the length of daily sessions of drug self-administration, as compared to much shorter daily sessions. The aim of this section is to summarize this research, but before proceeding, some comments on several relevant methodological issues are in order.
A first, obvious issue concerns the method for distinguishing the escalation process per se from the increase in behavior related to the acquisition of the instrumental response (i.e., positive reinforcement). At least two different approaches can be used to achieve this goal. In a within-subjects design, subjects can be pre-trained before having long access to drug self-administration. For instance, in some published studies, animals were first trained to acquire the drug self-administration response before increased drug availability. In this approach, escalation of drug self-administration manifests as a gradual increase in drug consumption over time above the pre-escalation level of consumption. In a between-subjects design, at least two groups of untrained animals are tested: one group has a short, daily access (ShA) to drug self-administration while the other group has a much longer daily access (LgA). In this approach, drug intake escalation appears in the LgA group as a gradual increase in the rate of drug consumption above the control level of the ShA group. This between-subjects design is less time consuming than the first approach because it does not require pretraining. Of course, these two approaches can be combined to better assess the development and maintenance of drug intake escalation following increased access time to the drug.
Another important methodological issue concerns the minimization of potential experimental restrictions on drug consumption. Obviously, to assess changes in drug consumption as a function of drug availability, individuals should be relatively free to regulate their drug intake (21). Thus, the response ratio requirement to obtain a fixed drug dose should be reduced to the minimum as in the continuous reinforcement (CRF) schedule. In addition, the postinjection time-out period should be selected to allow for the highest possible number of injections while protecting animals from the risk of overdose (which increases with the unit dose available). Finally, limiting the maximum number of injections per session should be avoided as this may interfere with the escalation process (22–24).
A final issue concerns the choice of the dependent variable for assessing the effects of drug access time on drug self-administration in the between-subjects design (i.e., ShA versus LgA). Specifically, the problem is to select a dependent variable with the highest degree of between-subjects comparability (obviously, this choice is not a problem in the within-subjects design because the assessment of drug intake escalation only involves within-subject comparisons). The most comparable dependent variable is the number of drug injections during the time period common to all access durations (e.g., during the first hour when comparing 1-h versus 6-h sessions of drug self-administration). Inversely, the least comparable variable is the total number of injections simply because it is directly influenced by the independent variable. Another potential dependent variable could be the average hourly number of injections obtained by dividing the total number of injections by the length of the self-administration session. However, this variable may be a source of inaccurate comparisons when there are pronounced within-session variations in drug self-administration – which is often the case for intravenous cocaine or heroin self-administration (e.g., initial drug loading). Thus, whenever possible, it will be preferable to compare drug use during the time period common to all access durations.
4.1 Stimulants
Steven Dworkin and his colleagues (25) were the first to suggest that different access time to intravenous cocaine self-administration is associated with different levels of intake in rats. In their initial experiment, rats had daily access to cocaine (0.5 mg/kg) during 12 (N = 4) or 24 (N = 7) hours for several days. Rats with the longest access time to the drug self-administered more cocaine than the other rats (3.5 versus 1.7 infusions/h). However, this early experiment involved a very limited number of rats and provided little information about initial levels of drug intake and how they eventually changed over time. Thus, from this study alone, it is not possible to determine whether the differences in cocaine consumption observed, as a function of drug access time, directly resulted from differential drug intake escalation or from some other, uncontrolled factor (e.g., preexisting individual differences) (26).
More recently, controlled experiments have addressed these shortcomings. It is now clearly established that the length of daily access to cocaine can profoundly alter the rate and pattern of drug self-administration. In one series of independent experiments (7, 21, 27), rats were first trained to self-administer food and then intravenous cocaine under a CRF schedule during several daily 1-h sessions. After stabilization in the rate of cocaine self-administration, rats were assigned in a counterbalanced manner to two access conditions: in the ShA condition, rats continued to have access to cocaine during daily 1-h sessions while in the LgA condition, rats had their daily access to the drug increased to 6 h. As expected, ShA rats maintained the same rate of cocaine self-administration throughout the duration of the experiment, though they were free to take more (Fig. 1a). In one study, this stability of intake was shown to last at least 5 months (21). In contrast, with longer daily sessions to the drug, rats steadily escalated both their first hour and total intake of cocaine (Fig. 1a, c). Importantly, during the first hour of drug access, cocaine self-administration by LgA rats rose to a level much higher than the stable level of intake maintained by ShA rats (Fig. 1a).
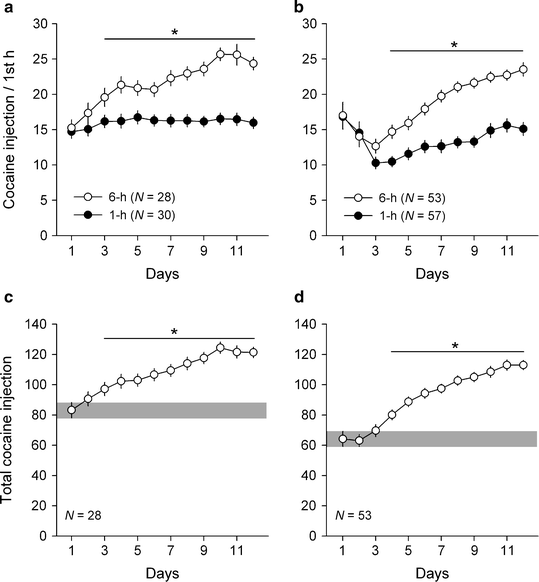

Fig. 1.
Effects of access time to cocaine on the pattern of self-administration. Data represent the mean number ± SEM of cocaine injections during the first hour of the session (top panels) or during the whole session (bottom panels). Rats had access to cocaine (unit dose = 0.25 mg, i.v.) for either 1 h (ShA rats) or 6 h/day (LgA rats). In the first set of experiments (a and c), rats were first allowed to self-administer cocaine during 1 or 2 h/day for at least 10 days before having differential access to the drug. In the second set of experiments (b and d), rats were initially trained to press a lever for food on a fixed-ratio 1 schedule of reinforcement before having differential access to cocaine self-administration. The horizontal gray box indicates the mean total number ± SEM of drug injections during the first day. * Different from ShA rats or from the first day (P < 0.05).
These basic findings were reproduced in a separate series of experiments in rats with a different behavioral history (28–31). In these experiments, rats were first trained to self-administer food under a CRF schedule after which they were tested during one single 1-h session of cocaine self-administration. The goal of this screening phase was to measure the initial level of operant responding before assignment of individuals to the ShA or LgA condition. Thus, in these experiments, rats had minimal experience with cocaine before differential drug exposure. Under these circumstances, the day-to-day pattern of cocaine self-administration is typically biphasic: cocaine intake slightly decreased within the first 5 days, reached a minimum and then began to increase to eventually level off at a stable level (Fig. 1b). The origin of the initial decrease in cocaine consumption has not been directly studied, but it probably corresponds to a transitional period during which initially cocaine-naïve animals progressively adapt to the change of reinforcers (from food to intravenous cocaine) and learn to titrate the effects of cocaine. This biphasic pattern was equally observed in both ShA and LgA rats. In LgA rats, however, the initial decrease in consumption was briefer and milder than in ShA rats and was followed by a much steeper increase in cocaine self-administration. As a result, the first hour of cocaine intake by LgA rats escalated within a few days above that of ShA rats (Fig. 1b). In addition, regardless of behavioral history, there was also a robust and parallel escalation in total cocaine consumption (Fig. 1d). Thus, regardless of initial training and pharmacological history, short versus long access time to cocaine self-administration induces two distinctive patterns of cocaine consumption: a stable pattern of moderate cocaine use versus an escalating pattern of excessive cocaine use.
Over the past 10 years, this basic observation has been reproduced several times by other teams or laboratories. Currently, these two patterns of drug use have been replicated in dozens of independent experiments (7, 21, 27–61). The metaanalysis of these studies clearly demonstrates that the relationship between increased drug access time and cocaine intake escalation holds true across a wide range of subjects and experimental conditions (Fig. 2), despite the occurrence of negative data from some laboratories (33, 34, 46, 47, 55). Furthermore, this relationship also extends to other stimulant drugs (Fig. 2). Increased access time to the drug precipitates an escalation of both amphetamine and methamphetamine self-administration (23, 24, 62–64) (Fig. 2).
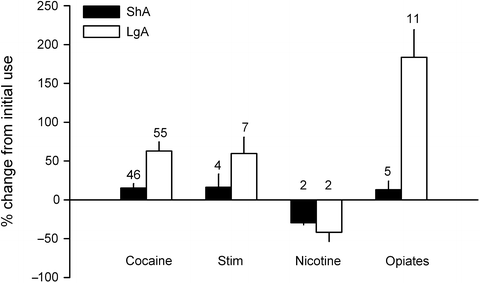

Fig. 2.
Metaanalysis of published studies on drug intake escalation in rats. A total of 49 separate studies have looked at the effects of drug access time on the pattern of self-administration. These studies amount to a total of 74 independent experiments (cocaine, 55; amphetamine, methamphetamine, 7; nicotine, 2; heroin, morphine, fentanyl, 11). Most, though not all, experiments compared the effects of access to 1 (ShA) versus 6 h (LgA) to the drug on subsequent changes in drug use. For each experiment, changes in drug use over the first 2 weeks were estimated using the digitizer software XYit3.1.4 (Geomatix Ltd, UK) and were expressed as percent change from the first day of drug access. The number above each bar corresponds to the number of experiments performed for each drug and each access condition (ShA versus LgA). In this set of experiments, the LgA condition was sometimes tested alone, which explains why the number of experiments corresponding to this access condition is generally higher than that corresponding to the ShA condition. Stimulant drugs (i.e., amphetamine and methamphetamine).
There is, however, one intriguing exception: nicotine. Increased access time to nicotine decreased, rather than increased, drug intake (Fig. 2) (Shelley Watkins, Serge Ahmed, George Koob and Athina Markou, 1999, unpublished data) (53, 65). This decrease in nicotine intake is paradoxical and may point to some unsuspected differences in abuse liability between nicotine and other stimulant drugs. Consistent with this interpretation, Kenny and Markou (65) recently reported that extended exposure to nicotine self-administration induced opposite changes in brain reward function compared to those seen following escalation of cocaine (29) or even heroin self-administration (66). Alternatively, the lack of escalation in nicotine self-administration may also reflect inappropriate access conditions. For instance, dramatic escalation to high levels of ethanol consumption can be rapidly triggered by forced periods of withdrawal between LgA sessions (67–69), whereas it takes dozens of weeks for a minority of animals to escalate their ethanol consumption with unlimited, continuous access to the drug (5, 6). Thus, it is possible that a more intermittent access to LgA sessions of nicotine self-administration would be more favorable to nicotine intake escalation, as suggested by recent studies on the nicotine deprivation effect (70, 71).
4.2 Opiates
Previous research has clearly established that continuous access to opiate self-administration is associated with a gradual escalation to higher levels of drug consumption in rats (72–74). However, until very recently, little research has been conducted to systematically assess the relationship between the length of drug access and the pattern and rate of opiate self-administration (66, 75–78). Nevertheless, the few studies published to date consistently extend most of the findings obtained with stimulant drugs to heroin, apart from the exception of nicotine (but see (79)). As with cocaine and regardless of initial training and pharmacological history, short versus long access time to heroin self-administration induces two different patterns and levels of consumption: a stable pattern of moderate heroin use versus an escalating pattern of excessive heroin consumption (Fig. 3a–d). Intriguingly, as revealed by a metaanalysis of the literature (22, 73–79), the severity of drug intake escalation appears to be higher with opiates (heroin, morphine, fentanyl) than with stimulants (Fig. 2). This relatively unexpected finding may suggest that opiates have a higher “dependence liability” than stimulants. Further comparative research is needed to confirm this interpretation.
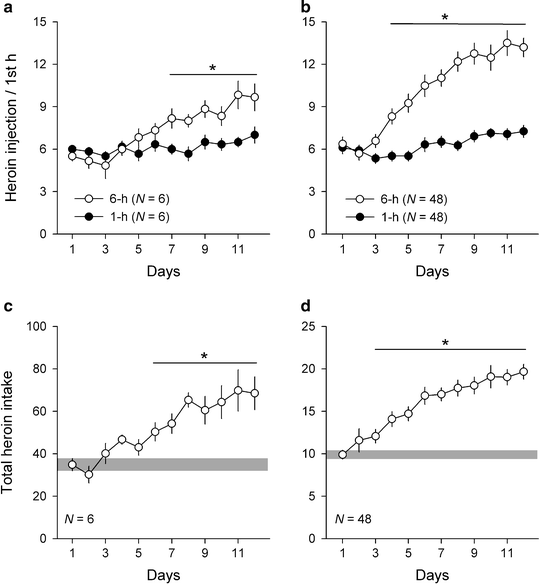

Fig. 3.
Effects of access time to heroin on the pattern of self-administration. Data represent the mean number ± SEM of heroin injections during the first hour of the session (top panels) or during the whole session (bottom panels). Rats had access to heroin (unit dose = 0.015–0.02 mg, i.v.) for either 1 h (ShA rats) or 6 (or 11) h/day (LgA rats). In the first experiment (a and c), rats were first allowed to self-administer heroin during 2 h/day for at least 10 days before having differential access to the drug (for additional information, (75)). In the second set of experiments (b and d), rats had no prior training history before having differential access to heroin self-administration (for additional information, see (77, 78)). In these experiments, the unit dose of heroin available during the last 5 h of each LgA session was increased to 0.06 mg. Data in (d) represent the mean number ± SEM of heroin injections during the last 5 h. The horizontal gray box indicates the mean total number ± SEM of drug injections during the first day.* Different from ShA rats or from the first day (P < 0.05).
4.3 Ethanol
It is notoriously difficult to incite naïve animals to spontaneously drink high amounts of ethanol to become dependent (80). For instance, as mentioned earlier, with unlimited access to ethanol in the home cage, it takes dozens of weeks for a minority of rats to escalate their ethanol consumption (5, 6). However, following the lead of a seminal, though neglected, study by Roy Wise in the early 1970s (68), a recent series of experiments from different laboratories has now clearly demonstrated that most rats can rapidly escalate their ethanol consumption to high levels if given a long and intermittent access to a highly-concentrated ethanol solution (i.e., 24-h access every other day to 20% ethanol) (67, 69). Note that in those studies, rats also had access to water, so ethanol drinking was not forced or driven by thirst. In addition, as with cocaine or heroin intake escalation, ethanol intake escalation was associated with a dramatic increase in ethanol loading early in the 24-h session (i.e., within the first hour). It remains to be seen, however, whether short versus long access to intermittent ethanol drinking can induce two patterns of ethanol consumption, as seen with many other drugs of abuse.
5 Drug Cross-Escalation
As described above, drug intake escalation is observed across a broad spectrum of drugs of abuse, including stimulants, opiates, and ethanol. Whether there is cross-escalation between different drugs of abuse or within the same drug class (e.g., the opiates) has not yet been tested systematically. Drug cross-escalation is defined here as an increase in the consumption of a newly encountered drug after intake escalation of a different drug. The systematic study of the phenomenon of drug cross-escalation may provide critical information, not only about neuropsychopharmacological commonalities in the escalation process, but also for better understanding polydrug abuse and addiction. To begin to address this issue, it was determined whether there is a cross-escalation between cocaine and heroin consumption – two highly addictive drugs with both common and different neuropsychopharmacological effects. Two separate groups of rats were first allowed to self-administer either cocaine or heroin for 1 h/day and then, after stabilization of drug intake, escalation of cocaine or heroin self-administration was precipitated by increasing drug access time to 6 h/day (Lenoir and Ahmed, submitted). For each group, a dose-injection function for drug self-administration was generated both before and after increased drug access time. As shown in Fig. 4, there was virtually no cross-escalation between cocaine and heroin. Specifically, as shown previously, after prolonged access to one drug (cocaine or heroin), rats escalated their consumption of this drug, which resulted in a characteristic vertical shift of the corresponding dose-injection function. However, the same rats did not increase their intake of the alternative drug, regardless of the available dose. The lack of cross-escalation to heroin self-administration in cocaine-escalated rats was confirmed in another study. In this study, rats (N = 8) were initially trained to self-administer both cocaine and heroin during 1 h on alternate days until stabilization of cocaine and heroin intake. Then, access to cocaine was increased to 8 h/day during several days. As expected, rats escalated their cocaine intake during extended access to cocaine but again, regardless of the dose available, there was no cross-escalation between cocaine and heroin. In fact, there was even a nonsignificant trend for decreased heroin consumption compared to prior cocaine intake escalation (Guillem and Ahmed, unpublished data). The lack of cross-escalation to cocaine self-administration in heroin-escalated rats is consistent with previous research showing no change in cocaine intake in rats with frequent heroin use under a discrete-trials procedure of drug self-administration (81, 82). Future research is clearly required to better assess the generality of these findings across a wider range of drugs of abuse, both between and within drug classes.
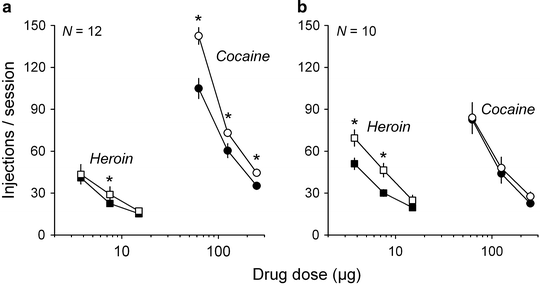

Fig. 4.
Drug cross-escalation in cocaine-trained (a) and heroin-trained (b) rats. Circles and squares represent the number of cocaine and heroin injections per session, respectively. Dose-injection functions for both cocaine and heroin self-administration (means ± SEM) were generated before (closed symbols) and after (open symbols) prolonged access (i.e., 6 h/day) to either cocaine (0.25 mg) or heroin (0.015 mg). Drug doses were tested in a between-session manner.* Different from the phase before escalation (P < 0.05).
6 The Dynamics and Stability of Drug Intake Escalation
As illustrated above, escalation of drug consumption is clearly a transient and negatively accelerating process, which eventually levels off at a new, higher level of consumption. This process can thus be characterized by different dynamic and state parameters, such as, its shape, speed, and final, post-escalation steady-state. So far, comparatively little research has been conducted to study how these different features systematically vary as a function of drug access condition. In one systematic study, Wee and colleagues (57) showed that the final, post-escalation level of cocaine intake increases with the length of daily sessions of cocaine self-administration: the longer the self-administration session, the greater the steady-state level. Whether the final, post-escalation level of drug consumption can also be influenced by other factors is less clear. In two studies from the same laboratory, the level of escalated cocaine or methamphetamine intake decreased with the training dose (57, 62) while in another study, the level of escalated cocaine self-administration remained unchanged (61). Clearly, additional parametric research is needed to better quantify the dynamics of the escalation process. This research will eventually prove useful for future pharmacological and neurocomputational modeling approaches to drug addiction (83).
Knowledge about the maintenance of escalated levels of drug consumption is even more limited. In one study, the maintenance of escalated levels of cocaine self-administration was shown to depend on the session duration (21). In this experiment, after inducing cocaine intake escalation, the daily session duration was reduced from 6 to 1 h. As a result, escalated levels of cocaine intake significantly decreased over time and progressively, though very slowly, returned toward pre-escalation levels of consumption. Indeed, even after 2 months of reduced drug access, the de-escalation of cocaine self-administration was still incomplete. In contrast, in another, related experiment, escalated levels of cocaine self-administration completely de-escalated to pre-escalation levels after only 1 month of forced abstinence (7). This differential outcome shows that compared to total abstinence, intermittent, brief exposure to cocaine self-administration can considerably retard, without preventing, drug recovery. This finding may have important clinical implications.
7 Association of Drug Escalation with Other Addiction-like Changes
There is now considerable evidence showing that increased access time to a variety of drugs of abuse can precipitate a rapid escalation to higher levels of drug consumption – a hallmark of addiction. More recent research now indicates that animals with escalating drug use also present other major behavioral signs of addiction, compared to animals with a more stable pattern and moderate level of drug use. These behavioral signs of addiction include: (1) an increased motivation to self-administer the drug, (2) greater difficulty in abstaining from drug use, and (3) a relative indifference to negative consequences. Finally, converging evidence from different laboratories shows that animals with increased drug use also become more sensitive to drug-induced and stress-induced reinstatement of drug seeking after extinction. Reinstatement of extinguished drug seeking is a well-validated animal model of craving and/or relapse (84). Though drug-induced craving is not a current diagnostic criterion of addiction, it nevertheless represents a selective marker of addiction since it is not seen in nondependent individuals (85, 86). Thus, as a whole, the differences between stable/moderate and excessive/escalating patterns of drug self-administration induced by differential drug access time in rats recapitulate the major behavioral differences between controlled and compulsive drug use in humans.
7.1 Association with Increased Drug Value and/or Motivation
Post-escalation upward shifts in the dose-effect function for cocaine self-administration first suggested an increase in the reinforcing value of and/or motivation for the drug following extended drug use (7, 32, 55, 57, 61). To understand why, the dose-effect function for cocaine self-administration must be reinterpreted within a behavioral economic framework (16, 87–89). Within this framework, the drug dose is inversely equivalent to the response requirement (or price) for maintaining the drug effects within the preferred range of the individual: the lower the dose, the higher this requirement. Thus, an upward shift in the peak rate of self-administration, as observed following drug intake escalation, reflects an increased willingness to pay a higher maximum price to defend drug consumption (i.e., a more inelastic drug demand), which betrays an increase in drug value and/or motivation. Christensen and coworkers (89) have reached the same conclusion using a more general mathematical approach for assessing the inelasticity of drug demand from dose-intake curves. Finally, an increase in the inelasticity of drug demand was directly observed following heroin intake escalation (78). As a whole, these studies suggest that escalation of drug consumption is associated with an increase in the reinforcing value of and/or motivation for the drug (but see (52)).
More conventional evidence for increased drug value and/or motivation following drug intake escalation was also obtained using the progressive ratio (PR) procedure (90, 91). Paterson and Markou (92) reported that following cocaine intake escalation, LgA rats maintain a higher breakpoint than ShA rats. This initial observation was later confirmed by other teams or laboratories (33, 57, 59) and was recently extended to other drugs of abuse, including methamphetamine (93) and heroin (78). Two independent studies, however, failed to reproduce this finding (33, 94). In fact, in one of these studies, escalation of cocaine self-administration – which was induced by passive administration of cocaine – was associated with lower, not higher, breakpoints (94). The origin of this discrepancy is currently unknown.
< div class='tao-gold-member'>
Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


