CHAPTER 143 Enucleation
Horses frequently develop serious ocular diseases that result in loss of function of the eye and chronic pain. Effects of injury or inflammation on the equine eye can be catastrophic. In addition to blindness, chronic equine ocular diseases can lead to permanent cosmetic defects. The cosmetic appearance of the eye, although not important to the horse, can be of serious concern to many owners. Enucleation has been the conventional treatment for these conditions and is indicated in horses with irreparable trauma, intraocular neoplasia, glaucoma causing blindness and pain, panophthalmitis, and intractable uveitis.
ENUCLEATION AND ORBITAL PROSTHESIS
Transconjunctival Enucleation
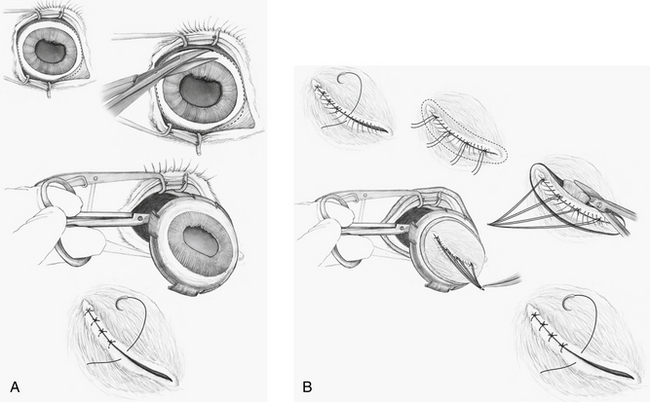
After placement of an eyelid speculum and creation of a lateral canthotomy, the transconjunctival enucleation is started by making an incision through the conjunctiva, 1 to 2 mm behind the limbus, 360 degrees around the eye (Figure 143-1, A). Using a combination of blunt and sharp dissection, the conjunctiva and overlying fibrous tissue are dissected off the globe. The opening is extended posteriorly and the extraocular muscles are identified and resected adjacent to the globe. The large retrobulbar muscles are then resected along with the optic nerve. A clamp or forceps should never be placed on the optic nerve; simple resection is all that is required. The globe is removed; if necessary, the orbit may be temporarily packed with sterile surgical gauze until hemorrhage ceases (usually within 1 to 2 minutes). The third eyelid and associated conjunctiva are removed, followed by the remaining tarsal conjunctiva. The eyelid margins are excised ensuring that the meibomian glands, which generally extend 5 mm into the eyelid margins, are removed. It is important also to remove all glistening conjunctiva to help prevent formation of mucoceles. The orbit is irrigated with sterile saline, but, to minimize irritation, other materials such as antimicrobials should not be infused into the orbit. Care must be exercised to ensure that the medial canthus is completely excised and that the angularis oculi vein, which lies near the medial canthus, is avoided.