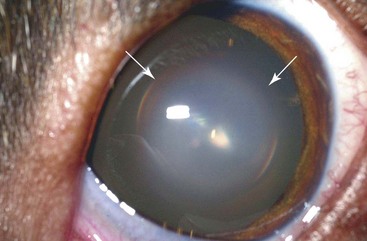
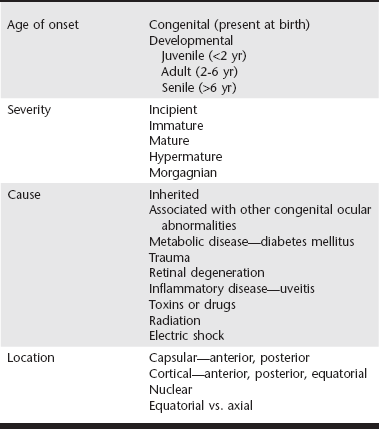
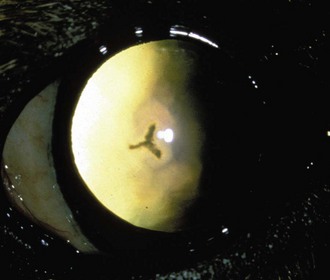
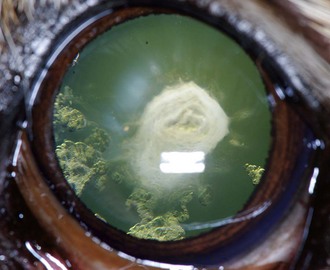
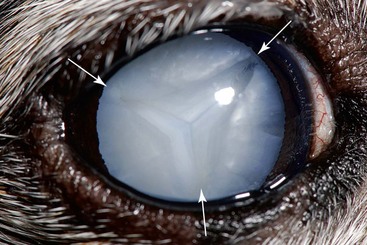
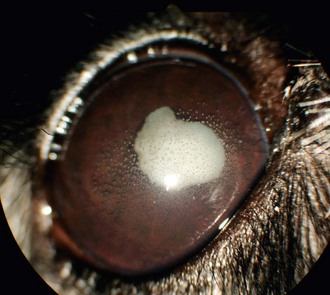
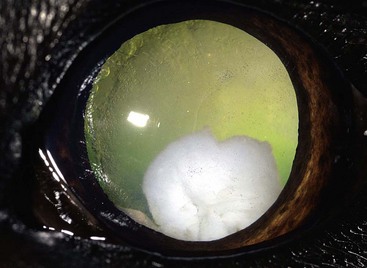
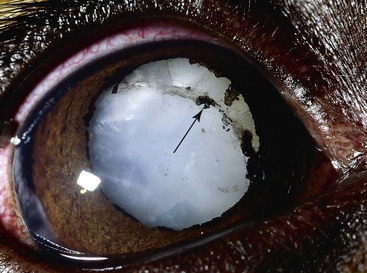
Chapter 253 New lens fibers are added throughout life, but the lens is restricted in the size to which it can grow. As a result, rather than increase in size, the lens increases in density and the central lens becomes compressed. This results in lenticular sclerosis, a zone of change in transparency between the central and peripheral lens. Clinically this becomes apparent at the age of 6 years in most dogs and cats and increases with age (Figure 253-1). A cataract is defined as an opacity of the lens or its capsule regardless of size. Cataracts are classified by age of onset, location, severity, and cause (Table 253-1). Cataracts may be congenital (present at birth), juvenile (appearing at <2 years of age), adult (appearing at 2 to 6 years of age), or senile (appearing at >6 years of age). Cataract locations are described as nuclear, cortical (anterior, posterior, equatorial), capsular, and axial versus peripheral. With respect to severity and the amount of lens affected by a cataract, the terms used are incipient (does not affect vision significantly; Figure 253-2), immature (interferes with vision but does not completely prevent it; Figure 253-3), mature (obscures an image entirely; Figure 253-4), and hypermature (liquefactive degeneration of the lens proteins has occurred). Liquefaction of lens protein results in lens-induced uveitis that may lead to globe hypotony, iris hyperpigmentation, aqueous flare, miosis, synechia, keratic precipitates, lens instability, secondary glaucoma, vitreous degeneration, or retinal detachment (Figure 253-5). Hypermature cataracts are characterized clinically by irregularity of the lens surface, a deeper anterior chamber, capsule wrinkling, and mineralization. Hypermature cataracts occasionally may undergo substantial or complete resorption in which the cortex liquefies and the nucleus shifts and are then termed morgagnian cataracts (Figure 253-6). In some of these cases, the patient may regain vision as the cataract resorbs, although retinal detachment often occurs during rapid resorption. Figure 253-2 Incipient axial posterior cortical cataract involving the posterior suture in a 2-year-old Labrador retriever. Figure 253-3 Immature cataract involving the posterior, anterior, and equatorial cortex in a 2-year-old golden retriever. The equatorial involvement shows cortical vacuoles suggestive of more recent and rapid cataract progression. Figure 253-4 Mature intumescent (swollen) cataract with suture clefting (arrows) secondary to diabetes mellitus. Figure 253-5 Hypermature cataract with secondary lens-induced uveitis. The uveitis has resulted in posterior synechia, dyscoria, and keratitic precipitates. Figure 253-6 Hypermature morgagnian cataract. Because the majority of the cataractous lens cortex has been resorbed, the remaining lens nucleus has settled ventrally in the capsular bag. Most canine cataracts are inherited or caused by diabetes mellitus. Inherited cataracts are seen in most breeds of dogs and in mixed-breed dogs. Inherited cataracts may be congenital or acquired and vary by breed in age of onset, location, severity, and progression. Affected animals should not be used for breeding regardless of the severity of the cataract. Metabolic causes of cataracts include diabetes mellitus and, less commonly, hypocalcemia. In dogs affected with diabetes mellitus, 50% will develop cataracts within 170 days of diagnosis of diabetes and 80% will have cataracts by 470 days. Diabetic cataracts begin with vacuoles or “bubbles” in the equator of the lens that progress, often rapidly, to swelling and rupture of lens fibers with subsequent complete opacification and clefting of the lens fibers at the suture junctions due to fluid accumulation (see Figure 253-4). Diabetic cataracts result when the enzyme aldose reductase catalyzes the reduction of glucose to sorbitol. The intracellular accumulation of sorbitol in the lens leads to an osmotic shift and swelling and disruption of lens fibers. Due to rapid and dramatic swelling of the lens, subsequent spontaneous lens capsule rupture has been described in dogs with diabetes mellitus as well as in nondiabetic dogs with rapidly progressive cataracts (Figure 253-7). Spontaneous lens capsule rupture is both a medical and a surgical emergency, with phacoclastic uveitis expected within days of the rupture. Additional causes of cataracts in dogs include trauma, uveitis, retinal degeneration, nutritional deficiencies, electrical shock, and radiation. Feline cataracts most commonly occur secondary to anterior uveitis. Inherited cataracts have been described in cats, but cataracts secondary to diabetes are not typically seen in the cat. Figure 253-7 Spontaneous lens capsule rupture secondary to diabetes mellitus. The lens capsule has ruptured equatorially with retraction of the anterior lens capsule (arrow) and exposure of the lens cortex.
Disorders of the Lens
Cataract
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree