26 Demodicosis
CASE HISTORY
The history in this case was as follows:
CLINICAL EXAMINATION
Demodicosis usually presents as focal or multifocal patches of alopecia with variable crusting, scaling and pruritus. Canine localized demodicosis (CLD) is usually defined as involving up to five individual patches of alopecia, while generalized disease (CGD) involves six or more patches, an entire body region, or presents as pododemodicosis. Squamous demodicosis is characterized by patches of alopecia, scaling, erythema, folliculitis and comedone formation. Pustular demodicosis is diagnosed when secondary bacterial infection is present, and is characterized by lesions of deep pyoderma and cellulitis. Most cases of CLD are squamous, whereas CGD may initially present as squamous, but frequently progresses to the pustular form of the disease. Exten-sive pustular demodicosis is a severe, potentially life-threatening systemic disease. Secondary infection with Staphylococcus intermedius is common and more rarely Pseudomonas aeruginosa or Proteus mirabilis may be involved. Peripheral lymphadenopathy is usually present in pustular demodicosis.
Examination in this case revealed:
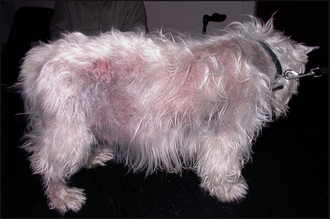
Figure 26.1 Adult-onset generalized demodicosis. Extensive truncal alopecia, erythema and hyperpigmentation.
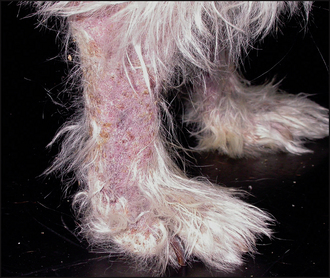
Figure 26.2 Close-up of the hind leg of the dog in Fig. 26.1, showing alopecia, scaling, crusting and erythema.
CASE WORK-UP
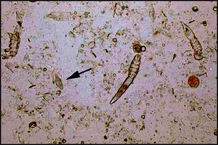
The diagnosis of demodicosis is generally made on the microscopic demonstration of mites or eggs. Skin scrapes are the most sensitive method of finding mites, although they may also be found on examination of exudate or on trichography (see Chapter 2). Skin scrapes and cytology should always be the first diagnostic tests performed where there is evidence of alopecia, crusting and scaling.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree