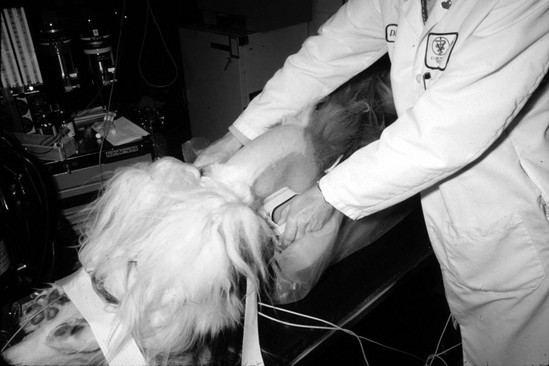
Web Chapter 60 DC cardioversion done as an elective procedure is useful for restoring sinus rhythm in dogs with sustained atrial fibrillation or atrial flutter. By improving hemodynamics (reducing ventricular filling pressures, augmenting cardiac output, decreasing ventricular rate, and providing atrioventricular synchrony), rhythm control generally is beneficial for dogs with congestive heart failure and secondary atrial fibrillation (Deedwania and Lardizabal, 2010; Sisson et al, 1995). Furthermore, restoration of sinus rhythm eliminates the need for pharmacologic control of heart rate using drugs that often have a negative inotropic effect, such as β-blockers and diltiazem (McNamara et al, 2003). In the absence of underlying heart disease, restoration of sinus rhythm in dogs with atrial fibrillation diminishes the risk of secondary thromboembolism and tachycardia-induced cardiomyopathy. In athletic dogs exercise tolerance also may improve. In dogs with atrial flutter, pharmacologic control of the ventricular rate frequently is difficult, and DC cardioversion often is the authors’ initial treatment of choice. As discussed later in this chapter, the quality of life and heart failure status of dogs are improved greatly following successful cardioversion of atrial fibrillation to sinus rhythm. However, the likelihood of maintenance of normal sinus rhythm after successful cardioversion is affected adversely by the presence of structural heart disease as well as by chronicity of atrial fibrillation, and these factors should be taken into account by both the clinician and dog owner when considering cardioversion in a dog with congestive heart failure (see the later section on the duration of sinus rhythm after cardioversion of atrial fibrillation). Although cardioversion may be accomplished by delivery of energy through either preplaced adhesive cardioversion pads or cardioversion paddles held against the thorax, the authors prefer paddles to achieve optimal positioning of electrodes and minimal transthoracic impedance. Immediately following induction of anesthesia, the dog is positioned in dorsal recumbency in a foam trough placed on a padded table. The forelimbs are secured cranially, and the rear limbs are secured caudally (Web Figure 60-1). Care must be taken to ensure that neither the dog nor the operator is in contact with any metallic surface.
Cardioversion
Indications and Contraindications for Direct Current Cardioversion
Cardioversion Procedure
< div class='tao-gold-member'>
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree