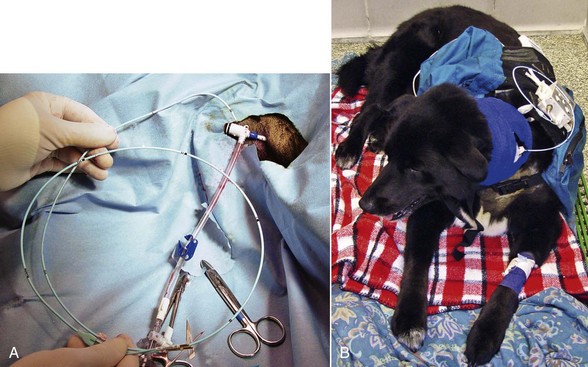
Web Chapter 4 During cardiopulmonary arrest (see Chapter 5) early identification of bradycardia and rapid initiation of a temporary pacing may supplement standard cardiopulmonary resuscitation (CPR) and may be beneficial for some patients. Arrhythmias that may benefit from cardiac pacing include severe sinus bradycardia, advanced AV block, slow ventricular escape rhythms, and asystole. Cardiac pacing is usually not effective in animals with pulseless electrical activity (e.g., electromechanical dissociation) or for ventricular fibrillation. During CPR, pacing is usually attempted when atropine and repeated doses of epinephrine administration fail to increase ventricular firing to a rate that is capable of providing adequate perfusion for the patient. The right or left jugular vein, the femoral vein, or the saphenous veins can be used for placement of the pacing lead, depending on patient size and vascular access. In some dogs, a 4 or 5 French pacing wire may be successfully advanced up the lateral saphenous vein. Jugular vein access is easier, and the lead is less likely to migrate or dislodge. The right jugular vein is the more direct route to the right atrium and ventricle and avoids any issues related to a persistent left cranial vena cava, but the left jugular vein or femoral vein should be used for temporary lead wire placement if a future permanent transvenous pacemaker implantation is anticipated (as the right jugular vein is generally chosen for permanent pacing). The skin over the target vein is first clipped, quickly cleaned, and infiltrated with 2% lidocaine, after which the skin is aseptically prepared. The vessel can be accessed via a cut-down technique or by vascular puncture using a catheter sheath introducer system (5 to 8.5 French percutaneous introducer) and a modified Seldinger approach (Web Figure 4-1, A). Once vascular access is secured, the pacing lead is passed into the vessel and toward the heart. Some operators prefer to insert the pacing catheter into a telescoping plastic sleeve that can later be advanced to cover the catheter and interlocked with the vascular access sheath; this allows for repositioning with less risk of contamination. Continuous electrocardiographic monitoring is performed during lead insertion to identify correct pacing lead placement, ventricular capture, or ventricular ectopy that might require repositioning of the catheter. Difficulties in lead advancement can be encountered with variations in vascular anatomy (e.g., persistent left cranial vena cava). Web Figure 4-1 A percutaneous sheath introducer is placed within the jugular vein via a modified Seldinger technique, and the pacing lead can be inserted through the non-bleedback port of the introducer as shown in A. The pacing lead is then connected to an external pulse generator to initiate cardiac pacing (B). The external pulse generator should be well secured to the patient to prevent lead dislodgment or migration as a result of movement.
Pacing in the ICU Setting
Indications for Temporary Pacing
Cardiopulmonary Arrest
Temporary Transvenous Pacing
Transvenous Pacing Technique
Patient Preparation and Sedation
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Chapter 4: Pacing in the ICU Setting
Only gold members can continue reading. Log In or Register to continue
