CHAPTER 182 Causes of Abortion
Abortions in horses are a common occurrence. A comprehensive study of causes of abortion, stillbirth, and perinatal death in horses over a 6-year period revealed that infection of the fetus or placenta caused by bacteria, equine herpesvirus, fungi, or placentitis of unknown cause was the most common cause of abortion and accounted for 34% of the diagnoses. The second most common cause involved birth complications, including asphyxia, dystocia, and trauma (19% of cases). Other common diagnoses were placental edema or premature separation of the placenta, twins, contracted foal syndrome, and other congenital and umbilical cord abnormalities. No diagnosis was made in 16% of the cases.
INFECTIOUS CAUSES OF ABORTION AND NEONATAL LOSS
Viral Infection
Equine Viral Arteritis
Equine viral arteritis usually arises as an outbreak of influenza-like illness in adult horses (see Chapter 35, Equine Viral Arteritis). Some outbreaks consist of only respiratory signs in the herd, but other outbreaks also include mares that abort because of the infection. Fetuses are usually aborted late in gestation, may be aborted in either an autolyzed or fresh state, and are infected by arteritis virus. Gross examination of the aborted fetuses may reveal pulmonary edema but usually no other lesions. Microscopically, aborted fetuses may have no lesions or there may be inflammatory changes in sections of brain, liver, spleen, heart, placenta, and other tissues. Lesions consist of a variable vasculitis with mononuclear cells and rare neutrophils seen within the vessel walls and forming small perivascular cuffs. Presumptive diagnosis can be made by detection of vasculitis in aborted fetuses during an outbreak of abortions. The diagnosis is confirmed by virus isolation from the fetal tissues and serum neutralization evidence of maternal seroconversion.
Bacterial and Fungal Infection
Bacterial and fungal infections of the fetoplacental unit are an important cause of abortion in horses. In one study in central Kentucky, fetoplacental infection caused approximately a third of abortions and neonatal deaths over a 6-year period, and bacterial infection caused almost three fourths of the abortions or deaths in which an etiologic agent was identified. These can be infections involving only the fetal membranes, or there can be concurrent spread to the fetal fluids and fetal organs. Most bacterial and fungal abortions are associated with placentitis, and the placentitis can be ascending or hematogenous in origin.
Placentitis
Ascending Placentitis
Gross lesions are usually present and include irregular thickening of the allantochorion in the area of the cervical star with brown or tan discoloration and mild surface exudate. Sometimes the affected area is hemorrhagic or congested, resulting in reddish black discoloration. The cranial extent of the placentitis is often sharply demarcated from the unaffected chorion, and there may be a hemorrhagic zone. The remainder of the allantochorion is usually grossly normal (Figure 182-1). If the infection has gained access to the fetal fluids or extraembryonic coelom, there may be concurrent hemorrhages, plaques, or roughening of the allantoic membrane, amnion, or umbilical cord. There may be petechial or ecchymotic hemorrhages on fetal organs and membranes. The lungs may be firm, and the liver is sometimes swollen, soft, and brown or brownish yellow (Figure 182-1).
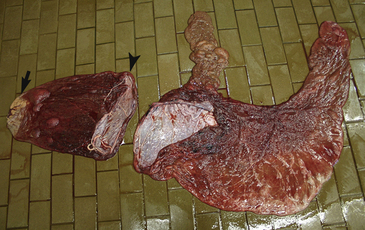
Figure 182-1 Placenta in two parts from an aborted equine fetus. The allantochorion has an area of thickening and discoloration indicative of ascending placentitis (arrow). Also notice the rupture and tearing of the body of the allantochorion resulting in premature placental separation (arrowhead). See Color Plate 20, following p. 832.
Atypical (Nocardioform) Placentitis
Nocardioform placentitis is not associated with a single bacterial species; rather, a group of similar organisms is commonly isolated. The most common nocardioform organisms that have been characterized and identified are Crossiella equi, Amycolatopsis kentuckyensis, Amycolatopsis lexingtonensis, and Amycolatopsis pretoriensis. Cases have been reported in which the gross appearance was identical to nocardioform placentitis but there was no evidence of nocardioform-type bacteria, although other species of bacteria were isolated, including Staphylococcus spp., Pantoea agglomerans, Cellulosimicrobium cellulans, Enterobacter
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


