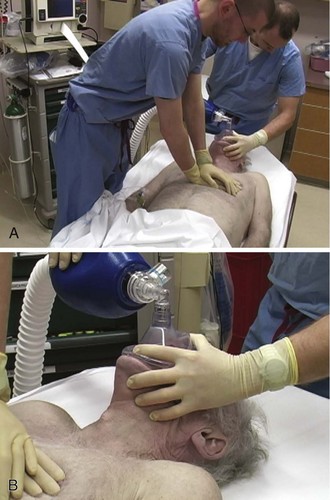
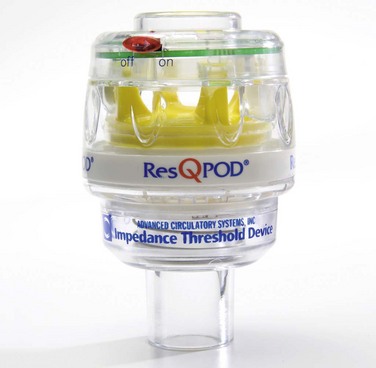
Chapter 17 Cardiopulmonary resuscitation (CPR) can be lifesaving for a patient in cardiac arrest, particularly in conjunction with other therapies such as defibrillation or delivery of medications. In several large clinical studies, data have shown that prompt delivery of CPR serves as an important predictor of successful outcome and increases the chance of survival by up to twofold. Each minute without treatment, on the other hand, is associated with a 10% to 15% decrease in the probability of survival.1,2 The quality of CPR is an important technical issue and has a direct effect on patient outcome. For example, shallow chest compressions have an adverse impact on the success of defibrillation.3 Because of these and related data, emphasis has recently been placed on improving the quality of CPR, and such priority has been codified in consensus CPR guidelines promulgated by the American Heart Association. These guidelines are formulated through a formalized data evaluation process and are updated every 5 years.4 Worrisome data have shown that the quality of CPR during actual resuscitation is endemically poor.5,6 Specifically, chest compressions are often administered too slowly with inadequate depth. In addition, pauses in chest compressions are too long, and hyperventilation of arrest patients is common. These deficiencies may be due to a variety of factors, including infrequent training, lack of awareness of the quality of CPR during resuscitation, and inadequate team leadership during resuscitation efforts.7 Although CPR is widely taught to health care personnel and reassessed periodically, the importance of high-quality CPR cannot be stressed enough. High-quality CPR immediately before defibrillation increases the chance of successful restoration of circulation.3,8 Although another recent multicenter investigation of out-of-hospital arrest did not support this claim,9 it is generally believed that for unwitnessed arrest or arrest events with a long downtime, early CPR and defibrillation have a significant impact on patient survival and recovery.10,11 Quality chest compression also increases the efficacy of drugs administered during resuscitation, whereas inadequate circulation leads to minimal effects from peripherally delivered drugs.12 Hyperventilation is also widely prevalent and dramatically compromises hemodynamics. In animal studies, hyperventilation leads to reduced survival from arrest. In this section we review the key procedural aspects of manual CPR. The 2010 resuscitation guidelines emphasize the importance of quality chest compression4 by recommending that clinicians focus on maintaining proper chest compression depth and rate. Compress the sternum to a depth of at least 2 inches with a rate of at least 100 compressions/min. Box 17-1 provides a summary of procedural recommendations for CPR. If possible, place a backboard under the victim to ensure appropriate thoracic compression. In addition, adjust the height of the bed or have the rescuer stand on top of a stepstool so that the entire weight of the rescuer above the waist is directed onto the patient’s sternum (Fig. 17-1A). This enhances the depth of compressions and helps prevent leaning on the patient’s chest between compressions, which is another key deficiency that has been widely observed. Extend the arms fully and place them perpendicular to the patient’s chest while making sure to pull away from the chest sufficiently between compressions to allow full chest recoil. Rotate rescuers aggressively (approximately every 2 to 3 minutes) to avoid deteriorating quality of compressions because of exhaustion. Properly delivered compressions are highly fatiguing, and rescuer bravado often interferes with the realization of declining CPR quality over time. Minimize pauses in chest compressions because even short pauses have profound effects on coronary perfusion pressure and outcomes.13 As stated earlier, long pauses in chest compressions before delivery of a shock are associated with failure of defibrillation.3 Do not stop CPR to deliver medications because the drugs can be administered at the same time as the compressions. Keep pauses in chest compressions to a minimum (e.g., for procedures such as intubation or pulse checks). Deliver ventilations at a rate of 8 to 10 breaths/min (see Fig. 17-1B). Hyperventilation (e.g., ventilation rates greater than 30/min) is common during resuscitation. To prevent unwittingly hyperventilating the patient, ask the rescuer who is providing ventilations to remove his or her hand completely off the bag-valve-mask apparatus between ventilations. The team leader should be vigilant in the observation of delivery of ventilations and should be ready to verbally prompt rescuers to ventilate the patient at the appropriate rate if hyperventilation is performed. Monitoring end-tidal CO2 pressure (Petco2) also affords an opportunity to detect a pulse during CPR. During ongoing resuscitation of a pulseless patient, capnography will generally remain low (often less than 20 mm Hg), which is indicative of low blood flow. If the patient achieves return of spontaneous circulation (ROSC), a sharp increase in the Petco2 value (usually greater than 25 to 30 mm Hg) is consistent with return of adequate perfusion.14 Cardiac arrest resuscitations are often crowded, chaotic events filled with stress and anxiety. To maximize calm and efficiency and to ensure quality of care, establish a team protocol. Designate someone to be the leader of the resuscitation, and make sure that all participants are clearly aware of this designation. The designated team leader should be responsible for monitoring the rhythm, for giving orders to initiate and terminate chest compressions, and for delivery of drugs and other therapies. The team leader should be situated either at the head of the bed or at a place where you can direct the resuscitation. As the team leader, it is important that you do not actually perform compressions, ventilations, or other specific procedures unless absolutely necessary because you may quickly lose control of the resuscitation. Since most rescuers are unable to detect when their own quality of compressions is diminishing, observe CPR closely and order rescuer rotations throughout the duration of the resuscitation.15 Chest compression–only cardiopulmonary resuscitation (CC-CPR) has been shown in a number of investigations to be as effective as standard CPR in resuscitation efforts initiated by members of the lay public.16,17 Give compressions at a rate of at least 100/min. Because of its simplicity, CC-CPR minimizes pauses in chest compressions while maintaining proper rate and depth. Lay rescuers in the community may be less experienced with standard CPR and uncomfortable with the performance of mouth-to-mouth resuscitation. The simplicity of CC-CPR makes it relatively easy for first responders to initiate resuscitation efforts and for emergency medical dispatchers to guide lay rescuers remotely. The American Heart Association’s 2010 guidelines have shifted emphasis from “ABC” (“airway, breathing, compressions”) to “CAB” (“compressions, airway, breathing”) for lay rescuers. Their endorsement of “hands-only CPR” (a synonym for CC-CPR) educational programs reflects additional evidence that a focus on chest compressions during CPR may lead to an increase in bystander CPR, as well as improvements in patient outcomes.18 Recent investigations have shown that CC-CPR is associated with improved survival of patients with out-of-hospital cardiac arrest when performed by lay bystanders. A period of CC-CPR before intubation and rhythm evaluation also improves outcomes when used by emergency medical service (EMS) personnel.19,20 The EMS community is likely to see more widespread adoption and use of CC-CPR by lay public educational programs in the upcoming years. Active compression-decompression cardiopulmonary resuscitation (ACD-CPR) is a variant of CPR in which the passive relaxation phase of CPR is converted into an active phase by means of a handheld or mechanical suction device, which can theoretically improve both myocardial and cerebral circulation when compared with traditional CPR.21,22 However, data on these devices are mixed; there have been studies on out-of-hospital cardiac arrest using this technique that did not find any improvements in either initial outcome or survival to discharge, and as with many devices, there are instances when its application is impractical.23,24 The impedance threshold device (ITD) optimizes chest compression hemodynamics via manipulation of intrathoracic pressure. From a practical standpoint, the ITD is a relatively simple device that is placed between the endotracheal tube and the bag-valve apparatus, much like a colorimetric Petco2 detector, which is familiar to most ED clinicians (Fig. 17-2). The ITD contains a valve that prevents air from flowing through the device that is less than 10 cm H2O in pressure. During resuscitation, the ITD prevents air from entering the thorax during recoil of the chest wall after each compression by generating a small but hemodynamically significant negative pressure within the chest. In laboratory studies this negative pressure enhances venous return to the heart and results in increased cardiac output with each subsequent chest compression.
Artificial Perfusion during Cardiac Arrest
Conventional CPR
Compressions
Ventilations
Pulse Checks
Leadership and Teamwork
New Directions: CC-CPR
Adjuncts to Improve the Quality of CPR
ACD-CPR
ITD
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Artificial Perfusion during Cardiac Arrest