Chapter 123 The goals of antisecretory therapy are to reduce gastric acid secretion, prevent damage to the gastric mucosa, and allow regenerative mucosal mechanisms to prevail (Box 123-1). H2 receptor antagonists (H2RAs) differ in their potency (famotidine > ranitidine = nizatidine > cimetidine); however, clinically increased potency does not necessarily correlate to increased efficacy. In developmental studies using the dog model, H2RAs have been shown to have an effect on canine gastric pH, where they produce an effect on gastric acidity for 6 to 7 hours. Cimetidine, the first H2RA, because of its increased frequency of administration and its interaction with the cytochrome P450 system, has been replaced by later-generation H2RAs. Unfortunately, in the last decade, several veterinary studies have demonstrated underwhelming acid suppression with later-generation H2RAs in dogs. In one veterinary study investigating the effects of different H2RAs on gastric pH in healthy dogs, ranitidine at a clinically recommended dose (2 mg/kg IV q12h) offered no change in gastric pH compared with saline (Bersenas et al, 2005). Results using famotidine at 0.5 mg/kg IV (q12h) were also underwhelming. Famotidine’s ability to raise substantially intragastric pH in dogs is limited (Tolbert et al, 2011). Clinically, oral famotidine has been shown to be efficacious for reducing the severity but not the prevalence of gastric lesions in racing sled dogs when used as a preventive (Williamson et al, 2007). Attempts at increasing the dose or dosing frequency of famotidine also have failed to show an improved outcome. It is unlikely that famotidine at the commonly used dose of 0.5 mg/kg q12h is very effective, and the once-daily dosing that has been recommended previously may not be as effective as suggested. Overall, the acid suppression provided by H2RAs at current veterinary doses is low. Some evidence suggests that famotidine should be selected over ranitidine for improved effect (Bersenas et al, 2005). Famotidine appears to help primarily animals that are at lesser risk for gastric lesions or are at risk for less severe gastric lesions. Famotidine remains an excellent drug for routine prophylaxis when cost is a concern or when an injectable drug is preferred.
Antacid Therapy
Pathogenesis of Ulcer Disease
Gastric Acid Suppressants
H2 Receptor Antagonists
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


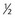 -1 tablet q6h PO (dog),
-1 tablet q6h PO (dog), 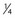 tablet q6h PO (cat)
tablet q6h PO (cat)