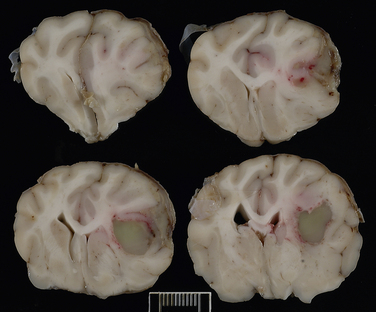
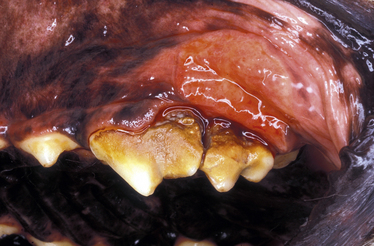
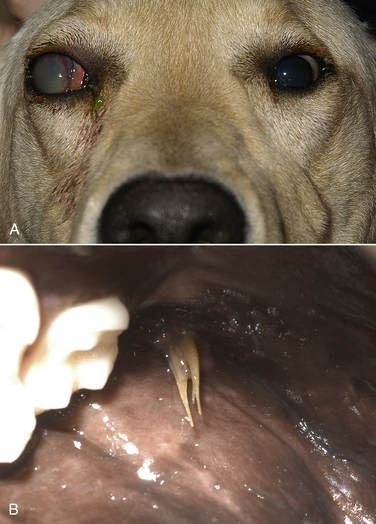
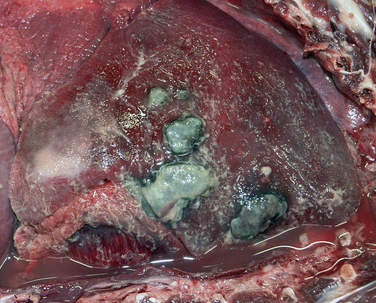
Chapter 37 Anaerobic bacteria can cause disease when they gain access to normally sterile sites. This occurs when mucosal barriers are disrupted, or when anaerobes gain access to subcutaneous tissues as a result of a contaminated penetrating wound. Anaerobic bacterial infections are often mixed infections owing to the concurrent presence of other anaerobes, as well as aerobes and facultative bacteria such as Pasteurella spp., Escherichia coli, streptococci, or staphylococci. Although there are hundreds of anaerobes that comprise the normal flora, the anaerobic bacterial species most often identified in disease are the gram-negative anaerobes Fusobacterium spp., Bacteroides spp., Prevotella spp., and Porphyromonas spp., and the gram-positive anaerobes Clostridium spp. and Peptostreptococcus spp. (Box 37-1).2 An accurate understanding of the epidemiology of anaerobic bacterial infections in dogs and cats has been hampered by difficulties associated with culture of anaerobes. The use of molecular methods such as PCR has begun to shed more light on this topic. The reader is referred to Chapters 48 and 54 for information on gastrointestinal Clostridium perfringens and Clostridium difficile infections, and disease caused by the toxins of Clostridium tetani and Clostridium botulinum, respectively. Plant awn migration in dogs and cats can lead to abscess formation in a variety of tissues, including retroperitoneal tissues and the brain. These abscesses usually contain a mixed population of aerobes and anaerobes, especially Fusobacterium, Actinomyces, and Bacteroides species. Brain abscessation can follow direct extension of anaerobic bacterial infection from otitis or tooth root infection. Alternatively, hematogenous spread may occur (Figure 37-1). FIGURE 37-1 Abscess in the white matter of the right frontal lobe of a 2-year-old female spayed Chihuahua that had a 1-month history of difficulty chewing food and lethargy and a 3-week history of progressive obtundation, neck pain, and tetraparesis. Signs initially improved following treatment with prednisone, but then recurred as the prednisone dose was reduced. The abscess in the frontal lobe communicated with the overlying meninges, which were expanded by a chronic and fibrosing suppurative inflammatory infiltrate. Another abscess was present in the midbrain, which suggested hematogenous spread of infection. Although no bacteria were seen within the lesions with special stains, Actinomyces canis and Fusobacterium nucleatum were cultured from the lesions. (Courtesy of the University of California, Davis Veterinary Anatomic Pathology Service.) Periodontal disease is one of the most common disorders seen by small animal veterinarians and may result in chronic pain, decreased appetite, and loss of teeth. It begins with formation of dental plaque as a result of poor oral hygiene and other host factors. Dental plaque is a bacterial biofilm composed primarily of gram-positive facultative anaerobes. Subsequently there is proliferation of pathogenic bacteria, which include gram-negative rods and especially anaerobes. These secrete toxins and incite an inflammatory response. Anaerobes implicated in canine and feline periodontal disease (such as Porphyromonas gulae) differ from those implicated in human periodontal disease (Porphyromonas gingivalis).3–6 Periodontal disease is manifested as gingival erythema, edema, gingival bleeding, and halitosis, with accumulation of calculus, gingival recession, alveolar bone loss, and sometimes the presence of purulent exudate (Figure 37-2). FIGURE 37-2 Periodontitis in a dog. There is significant gingival inflammation, plaque and calculus accumulation, and purulent exudate. Gingival recession and contact ulceration of the buccal mucosa are also present. (Courtesy of Dr. Frank Verstraete, University of California, Davis Dentistry and Oral Surgery Service.) Retrobulbar or orbital abscesses can result from tooth root abscessation, penetrating foreign bodies such as grass awns, or penetrating trauma to the orbit. Clinical signs include unilateral exophthalmos, protrusion of the nictitans, conjunctival hyperemia, serous to mucopurulent ocular discharge, inappetence, fever, and pain on opening the mouth (Figure 37-3). A fluctuant swelling or draining tract posterior to the last ipsilateral molar may be present on examination of the oral cavity. In one study, Bacteroides spp. and Clostridium spp. were the most frequent anaerobes isolated from 34 dogs with retrobulbar abscesses; other frequently isolated bacteria were Staphylococcus spp., Pasteurella spp., and Escherichia coli. In cats, the most frequent anaerobe was Bacteroides vulgatus, and the most common nonanaerobe was Pasteurella spp.7 FIGURE 37-3 Retrobulbar abscess and endophthalmitis secondary to a migrating grass awn foreign body in a 10-month-old intact male Labrador retriever. A, Note the mucopurulent ocular discharge from the right eye, as well as buphthalmos (enlargement of the eye) and exophthalmos. The nictating membrane and conjunctiva are hyperemic, and there is diffuse corneal edema. Hypopyon and iris bombe were also present. Globe retropulsion was reduced and painful on the right side. B, Multiple grass awns were present all over the dog’s haircoat, and an awn (shown) was removed from the gingiva posterior to the last right maxillary molar tooth. The right eye was subsequently enucleated. No additional grass awns were found. Histopathology of the globe showed severe chronic fibrinosuppurative panophthalmitis with focal, 0.3-cm scleral rupture in the caudal sclera near the optic nerve, regional orbital granulation tissue, and rupture of the lens. (Courtesy of the University of California, Davis Veterinary Ophthalmology Service.) Cat bite abscesses are one of the most common reasons that cats are brought to small animal clinics. Clinical signs include fever, lethargy, inappetence, pain, and firm or fluctuant subcutaneous swellings that may rupture and drain purulent material. Oral anaerobes and Pasteurella multocida are frequently isolated from these abscesses.8 Anaerobic species involved include Peptostreptococcus anaerobius, Porphyromonas spp., Clostridium villosum, Fusobacterium spp., Bacteroides spp. (especially Bacteroides tectum), and Prevotella spp.9 Despite the widespread occurrence of cat bite abscesses, studies that use molecular methods to identify the types and relative prevalences of anaerobes in cat bite abscesses are lacking. Other skin and soft tissue infections associated with a variety of anaerobes include foreign body penetrating wounds and dog bite wounds (see Chapter 57). Anaerobes such as Fusobacterium spp., Peptostreptococcus anaerobius, Prevotella spp., and Porphyromonas spp. are frequently isolated from dogs and cats with aspiration pneumonia, foreign body pneumonia (especially that due to plant awn migration), and pyothorax.10 Dogs with plant awn migration develop multifocal necrotizing pneumonia with abscess formation. In some cases, aspiration pneumonia is followed by lung abscess formation (Figure 37-4). In human patients, a period of 6 to 7 days is required for necrosis and abscess formation to occur after aspiration, and so aspiration pneumonia with lung abscess formation is generally a chronic disease process. FIGURE 37-4 Necropsy findings in an 11-year-old male neutered Labrador retriever with severe aspiration pneumonia secondary to laryngeal tie-back surgery for laryngeal paralysis, which occurred 2 months before death. Aspiration led to bronchopneumonia with multifocal abscessation, pleural rupture, pyothorax, and pneumothorax. There are multiple to coalescing black to dark gray, soft, irregular foci in the lungs that measured up to 4.5 cm in diameter. On cut surface, dark gray to black material oozed from the parenchyma. Aerobic bacterial culture yielded large numbers of bacteria that included Streptococcus canis, nonfermenter group 3 organisms, and Pasteurella canis. Anaerobic culture yielded large numbers of Peptostreptococcus anaerobius. (Courtesy of the University of California, Davis, Veterinary Anatomic Pathology Service.)
Anaerobic Bacterial Infections
Etiology and Epidemiology
Clinical Features
Periodontal Disease
Retrobulbar Abscesses
Skin and Soft Tissue Infections
Pneumonia and Pyothorax
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Anaerobic Bacterial Infections
Only gold members can continue reading. Log In or Register to continue
