CHAPTER 145 Acute Care of Soft Tissue Injuries Involving the Eyelids, Ears, and Face
The horse is prone to traumatic injury of the head. Environmental conditions, a heightened flight response, and equipment and tack used for horses all contribute to injury occurrence. Despite the impressive volume of bleeding and very concerned owners that often accompany horses with a head injury, few incidents are truly life threatening to the horse; depression fractures of the cranium, resulting in cerebral trauma, are one exception. However, an injury can have substantial impact on the horse’s athletic performance or appearance, and hence on its consequent value to the owner. Successful surgery of the head is facilitated by the region’s extensive blood supply and by close attention to surgical technique on the part of the surgeon. There is often limited soft tissue to work with, and wounds may be contaminated at the time of initial injury or when paranasal sinuses or nasal passages are penetrated. Wounds that are left to heal by second intention may appear cosmetically unacceptable because of scar contracture or tissue loss and attendant misshapen anatomic features. In some instances, chronic medical conditions (e.g., exposure keratitis when an upper eyelid laceration heals and contracts) can result from open-wound management.
EYELIDS
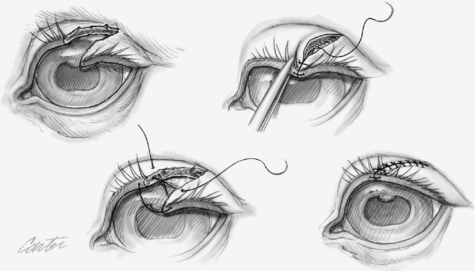
Full-thickness lacerations that involve the eyelid margin are more common and necessitate two-layer closure. Again, debridement of the wound margins should be very conservative to preserve the maximum possible amount of tissue and result in the best chance for normal functional outcome. The eyelid margin should be accurately realigned with a figure-of-eight, cruciate, or mattress suture using 4-0 to 6-0 absorbable suture material, with the knot protruding externally and distant from the margin, so it does not rub on the cornea. This suture can be preplaced before the deep-layer closure or placed after the deep layer closure. The deep, tarsal plate layer of the eyelid is closed in a simple continuous pattern with 5-0 or 6-0 absorbable suture that does not penetrate the conjunctiva. Lastly, the skin is carefully apposed, starting adjacent to the eyelid margin suture, with simple interrupted, 3-0 to 6-0 nonabsorbable sutures (Figure 145-1). No suture tags or knots should be able to contact the cornea. Blepharoplasty procedures are necessary with defects involving more than 30% to 40% of the lid margin tissue. Impaired eyelid function can be managed with temporary tarsorrhaphy or a third-eyelid flap to protect the globe. Injury to the cornea must be concurrently treated, and this may include placement of a subpalpebral lavage catheter for medication administration.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree