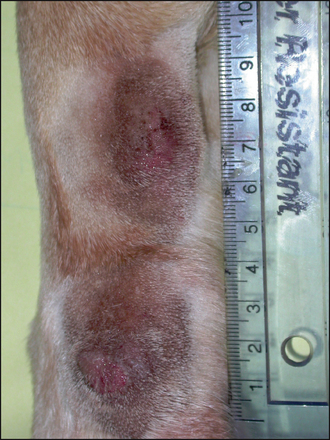
45 Acral lick dermatitis
CASE HISTORY
The relevant history in this case was:
• Nine months previously, the dog had started to lick the left forelimb and, despite topical antibacterial and glucocorticoid therapy (sodium fusidate and betamethasone), the licking had persisted, resulting in two eroded and exudative plaques.
• The licking behaviour would not occur when the dog was being observed. It had become evident that licking occurred whenever the dog was left unattended.
• Both owners worked full time. They had moved house two and a half years previously. Prior to that, one or other of them had been able to return home during the day to exercise the dogs, but this had not been possible since the move. The dogs were in a kennel with a dog flap and a large outside run from 7.30 a.m. until 6.00.p.m. 5 days a week.
• Routine flea control consisted of monthly applications of fipronil spot-on during the summer and every 6–8 weeks during the winter.