Chapter 18 Ultrasonography and Orthopedic (Nonarticular) Disease
The use of diagnostic ultrasonography for evaluation of tendons, ligaments, tendon sheaths, bursae, and joints is discussed in Chapters 16, 17, and 82, and horse preparation for other musculoskeletal uses is similar.
Skeletal Muscle
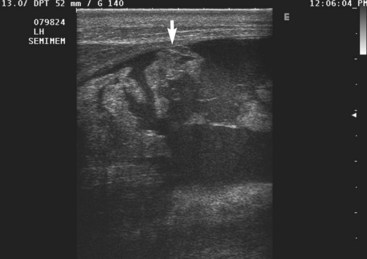
Traumatic muscle injuries, myositis, and masses infiltrating the muscles usually can be differentiated from one another by ultrasonography.1 Muscle tears in horses most frequently are seen in the hindlimb and shoulder musculature. In neonatal foals, muscle tears are most commonly seen in the hindlimb.3 The affected muscle or muscles can be identified by tracing the involved muscle from its origin to insertion. Fluid-filled anechogenic areas with hypoechogenic loculations are located within the muscle belly, associated with areas of hemorrhage and muscle fiber tearing (Figure 18-1).1,3-6 As the muscle injury becomes more severe, large areas of interfascial and subcutaneous hemorrhage are detected. The free edge of a completely disrupted muscle may be imaged floating in the anechogenic loculated fluid in the hematoma. Echogenic areas of clot are often imaged within the intramuscular, interfascial, or subcutaneous hematoma. As these echogenic clots become more organized, they may cast an acoustic shadow from the far surface. Rupture of the gastrocnemius muscle should be considered as a cause of recumbency in neonatal foals that are unable to rise and have soft tissue swelling in the hindlimb. Rupture of the gastrocnemius muscle has been reported as a complication of dystocia.3 Partial muscle tears are more difficult to diagnose because the ultrasonographic abnormalities are more subtle.1 The normal striated muscle pattern is lost with increased echogenicity of the injured muscle.1 Swelling of the affected muscle usually is present. Tears in the muscle fascia or thickening of the muscle fascia or fasciitis also may be detected ultrasonographically.1