Chapter 17 Ultrasonographic Examination of Joints
Fetlock
Dorsal Aspect
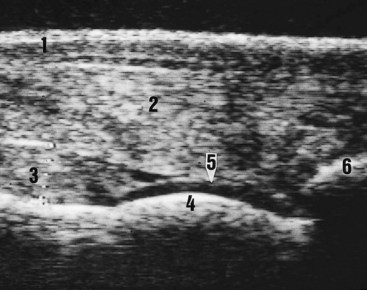
Figure 17-1 shows normal ultrasonographic anatomy.4,5 In normal fetlock joints the articular capsule is echogenic (except if too relaxed), and the articular margins of the proximal phalanx and the condyles of the third metacarpal bone (McIII) are smooth.
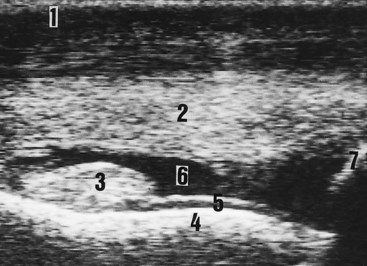
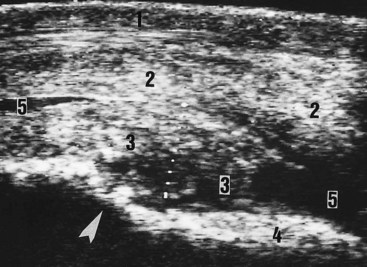
Ultrasonography is a useful technique for the differential diagnosis of soft tissue injuries on the dorsal aspect of the fetlock joint. These lesions include subcutaneous swelling or abscess, bursitis of the subtendonous bursa of the extensor tendons, extensor tendonitis, capsulitis, synovial fluid distention of the dorsal recess of the metacarpophalangeal joint (Figure 17-2), and chronic proliferative synovitis of the proximodorsal synovial fold of this joint (Figure 17-3). Thinning, fibrillation, and fissures of the articular cartilage of the dorsal and distal aspects of the condyle of the McIII can be identified with high-resolution transducers. Subchondral bone lesions can sometimes be detected before they are visible radiologically. Ultrasonography may be more sensitive than radiography for detection of the site and number of osteochondral fragments.7
Medial and Lateral Aspects
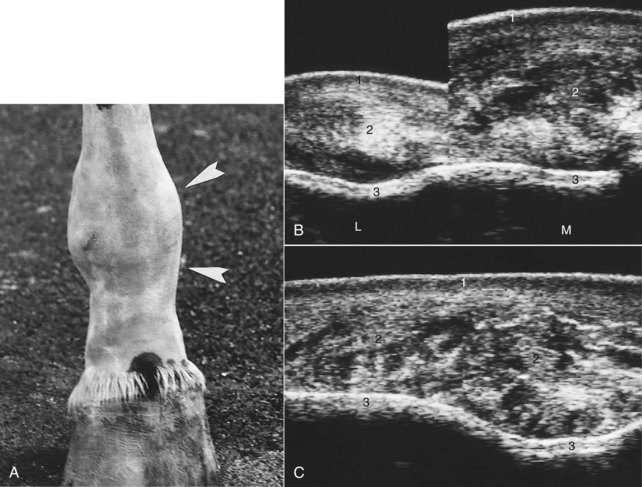
The medial and lateral collateral ligaments have superficial and deep layers.4 If the transducer is parallel to the skin (the ultrasound beam is perpendicular to fiber interface), the superficial layer of the collateral ligament is echogenic and the deep layer is hypoechogenic. Either layer may be damaged (Figure 17-4). If both layers are affected, joint instability, subluxation, or luxation occurs.