Chapter 44The Tarsus
Anatomical Considerations
Anatomical aspects of the gastrocnemius and calcaneal bursae and the tarsal sheath are discussed elsewhere (Chapters 76, 79, and 80). The distal tendon of the long digital extensor muscle is enclosed within a synovial sheath as it passes over the dorsolateral aspect of the tarsus. This sheath is compressed by transverse retinacular bands, resulting in a loculated appearance if the sheath is distended. Such longitudinal swelling is a quite common incidental finding in both sound and lame horses either unilaterally or bilaterally and is only rarely associated with pain and lameness. Focal lesions of the long digital extensor tendon have been identified ultrasonographically, but usually unassociated with lameness.
Diagnosis
Clinical Signs
Swelling is a variable feature of hock-related lameness. There are numerous common swellings of the tarsus. but the presence of swelling is not pathognomonic for tarsal region pain (see Chapter 6, page 58, and Figure 6-28Figure 6-29Figure 6-30Figure 6-31Figure 6-32). Swellings include capped hock, which must be differentiated from lateral dislocation or luxation of the superficial digital flexor tendon and swelling of the calcaneal bursae; tarsal sheath–associated or, less commonly, non–sheath associated thoroughpin; bog spavin (effusion of the tarsocrural joint); bone spavin (bony prominence of the dorsal and medial aspects of the distal tarsal region); curb (see Figure 78-1), a collection of soft tissue injuries involving the distal plantar aspect of the hock; and diffuse soft tissue swelling in the distal aspect of the crus and dorsal aspect of the tarsus associated with injury of the fibularis (peroneus) tertius. Rapid development of diffuse periarticular swelling may follow trauma of the tarsus or may herald periarticular cellulitis. Distention of the tarsocrural joint can be an incidental finding but may reflect primary joint pathology. Distention of the distal hock joint capsules is rarely detectable clinically, but if it occurs in association with OA, there may be firm enlargement on the medial aspect of the limb reflecting periarticular new bone and overlying fibrous tissue. The presence of this swelling, bone spavin, is neither required for horses to be lame as a result of distal hock joint pain nor pathognomonic for distal hock joint pain in horses in which it is found. Swelling restricted to the medial or lateral aspect of the tarsus may reflect CL injury and malleolar fractures of the distal aspect of the tibia.
Some horses with tarsal region pain resent passive flexion, but exaggerated lifting of the limb to avoid maximal flexion is more likely to reflect stifle pain. Although there are many advocates of the Churchill test for the detection of distal hock joint pain (see Chapter 6), we do not find this test particularly useful because there are many false-positive and some false-negative responses. This may reflect the degree of pressure applied, because one author (SJD) is rarely able to induce pain, whereas the other (MWR) frequently does elicit a pain response. Some horses with distal hock joint pain do manifest a positive reaction to palpation of the medial soft tissue structures and the proximal medial metatarsal region, likely reflecting the presence of periarticular soft tissue pain associated with OA. Horses often manifest a positive response to compression of the distal medial aspect of the tarsus and proximal medial aspect of the metatarsal region statically, and lameness can often be exacerbated with compression of this region followed by trotting, a dynamic test; yet pain in these horses is localized with diagnostic analgesia to the distal portion of the hindlimb. Proximal suspensory desmitis and lameness associated with the metatarsophalangeal joint are common diagnoses in these horses. It is possible that horses with distal hindlimb pain move abnormally and have coexistent pain in the region compressed using the Churchill test (see Figure 6-33Figure 6-34Figure 6-35). The absence of a positive Churchill test result should not lead the examiner to conclude the horse does not have tarsal region pain, a false-negative response. Unless clinical signs are diagnostic or a horse is suspected to have a fracture, diagnostic analgesia should always be used to confirm the presence of tarsal region pain.
Shoe wear can be excessive in horses with chronic tarsal region pain. Shoes are often worn on the toe or, most commonly, on the dorsal and lateral aspects (see Figure 6-38). Often, the fullering and toe grab, if present, are worn completely through, a finding that is most prominent in horses shod in aluminum shoes. Horses with pain causing lameness from other sources in the distal aspect of the hindlimb can manifest similar shoe wear, so this finding is not pathognomonic of distal hock joint pain. Horses with chronic tarsal region pain often have coexistent signs of pain on palpation of the gluteal and thoracolumbar area. Concurrent back and gluteal pain is likely secondary to chronic abnormal limb carriage causing muscle pain.
Horses with tarsal region pain often respond positively to an upper limb flexion test (see Chapter 8, page 84 and Figure 8-8). This test has erroneously been called the spavin test and a positive response should not be interpreted as pathognomonic for tarsal region pain. When it is suspected that a horse has tarsal region pain, this test often gives false-positive results. The most marked response to an upper limb flexion test may indeed be observed in horses with tarsal region pain, but a positive response can be seen with pain originating from the stifle, the hip region, and even the distal aspects of the limb. The upper limb flexion test is not specific, nor is the “hock extension test” (see Figure 8-10), a test used to exacerbate lameness in horses with tarsal region pain. There is no substitute for accurate diagnostic analgesia.
Diagnostic Analgesia
Perineural analgesia of the fibular and tibial nerves is well tolerated by most horses (see Chapter 10). One of us (SJD) deposits a subcutaneous bleb of local anesthetic solution at both injection sites using a 25-G needle before performing the blocks. Although a 3.7-cm needle is adequate for most horses, to reach the deep branch of the fibular nerve requires a 5-cm needle in large (700 kg) horses. These nerves are large, and it takes longer for analgesia to develop than with more distal limb blocks. Do not be in a hurry to move proximally in the limb and perform intraarticular analgesia of the stifle or hip joints, because these blocks may take a full hour to work. We usually first evaluate the horse 20 minutes after injection and for up to an hour. It is important to recognize that successful blocks may increase or create a toe drag; improved stride length, rhythm, and symmetry of the hindquarters must therefore be used to evaluate improvement in lameness. Occasionally a horse will stumble slightly after fibular and tibial nerve blocks, but we commonly see horses ridden before and after and do not believe there are undue risks.
Diagnostic Imaging
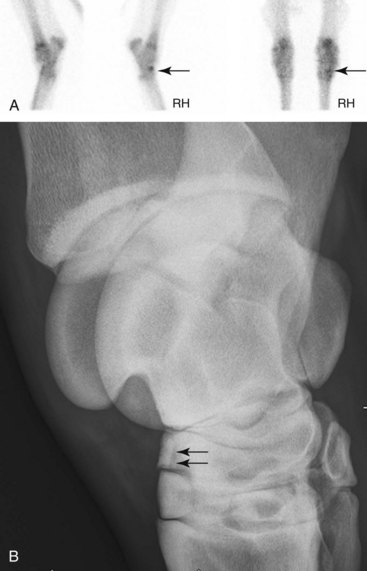
Nuclear scintigraphy is most useful when pain causing lameness has been localized to the tarsus but no radiological or ultrasonographic abnormalities are detected to explain the lameness.19 The identification of increased radiopharmaceutical uptake (IRU) may prompt acquisition of additional radiographic images that yield a diagnosis. Scintigraphy may also be useful in horses that are difficult to nerve block or those that are examined for poor performance rather than overt lameness. It is important to recognize that RU in the distal tarsal bones can be influenced by the type of work history. For example, there is greater RU in the dorsal aspect of the central and third tarsal bones in elite show jumpers compared with horses from other disciplines.5 In a plantar scintigraphic image of the tarsus it is common and considered normal to have greater RU in the subchondral bone of the lateral aspect of the tarsometatarsal joint and the proximal aspect of the MtIV compared with medially.20 This finding should not be interpreted as supportive of a diagnosis of distal hock joint pain. In young racehorses with early OA of the centrodistal and tarsometatarsal joints, focal moderate-to-intense IRU is found most often in the dorsal and lateral aspects of these joints, corresponding to radiological abnormalities detectable on the dorsomedial-plantarolateral radiographic image.21 The most common location for fractures of the central and third tarsal bones is on the dorsolateral aspect, and fractures can most reliably be seen in the dorsomedial-plantarolateral oblique radiographic image (Figure 44-1). These findings differ somewhat from most anecdotal reports, suggesting that it is the medial aspect of these joints that show early radiological changes and may be a reflection of a difference between racehorses and sports horses. In older racehorses with advanced OA and sports horses, scintigraphic and radiological evidence of OA is commonly found on both the medial and lateral aspects of the distal hock joints.
Articular Diseases of the Tarsus
Osteoarthritis of the Distal Hock Joints and Distal Hock Joint Pain
Distal hock joint pain is common in horses from all disciplines and is often associated with OA. Distal hock joint pain is known colloquially as bone or jack spavin or occult or blind spavin in the absence of radiological abnormalities. The term juvenile spavin has been used to describe early OA that had a prevalence of 20% in a group of horses younger than 2 years of age.26 Although it is usually seen in mature horses used for sport or pleasure, distal hock joint pain can occur in young Thoroughbred (TB) and STB racehorses and Western performance horses (see Chapter 120). Distal hock joint pain may be a sequela to incomplete ossification of the central and third tarsal bones (see page 517). Certain conformational abnormalities (such as sickle-hock, in-at-the-hock, or cow-hock conformation) or excessive straightness of the hindlimbs may predispose to distal hock joint pain, although this condition frequently occurs in normally conformed horses. Traditionally it has been proposed that OA of the distal hock joints is caused by excessive compression and rotation of the distal tarsal joints as the horse jumps or stops, which results in abnormal tension on the intertarsal ligaments. However, this theory is not consistent with the common recognition of distal hock joint pain in pleasure horses or its high incidence in Icelandic horses, a breed in which OA is thought to be a heritable condition.27 Distal hock joint pain is classically thought to begin on the dorsomedial aspect of the joints and to progress dorsally. However, it is our experience that in OA, scintigraphic or radiological abnormalities are frequently first identified only on the dorsolateral aspect of the joints, a region of high compressive strain. Previous exercise history and thus loading of the joints may be influential.28 Nuclear scintigraphic studies of clinically normal mature horses in active work has shown mild greater uptake of radiopharmaceutical on the lateral aspect, which is consistent with increased modeling, presumably the result of a relative increased loading laterally compared with medially.7
The centrodistal and tarsometatarsal joints are most commonly affected, either individually or together, but OA of the proximal intertarsal joint does occur, usually in association with OA of the more distal joints. The condition may be unilateral but is often bilateral. Occasionally OA of the talocalcaneal joint occurs either in isolation29,30 or together with OA of the centrodistal and tarsometatarsal joints31 (see page 516).
History
Clinical signs of distal hock joint pain vary considerably among horses, ranging from a moderate-to-severe unilateral lameness to subtle changes in performance without overt lameness (see Chapter 97Chapter 106Chapter 107Chapter 108Chapter 109Chapter 110Chapter 111Chapter 112Chapter 113Chapter 114Chapter 115Chapter 116Chapter 117Chapter 118Chapter 119Chapter 120Chapter 121Chapter 122Chapter 123Chapter 124Chapter 125Chapter 126Chapter 127Chapter 128Chapter 129). These signs include the horse becoming disunited in canter, being unwilling to canter with a particular lead, and being reluctant to turn or decelerate with proper engagement of the hindlimbs. The owner may comment that the farrier has experienced difficulties when shoeing the horse. Frequently a horse with bilateral distal hock joint pain has low-grade stiffness that wears off (warms out of pain) with work. Lameness frequently improves or resolves with rest but recurs when work is resumed. Treatment with nonsteroidal antiinflammatory drugs (NSAIDs) usually results in an improvement in lameness unless it is severe.
Clinical Signs
In many horses no abnormalities are detectable by visual inspection or palpation of the hock region. In horses with more chronic distal hock joint pain there may be enlargement over the medial or dorsomedial aspects of the distal hock joints, which is the result of periarticular soft tissue thickening. Distention of the tarsocrural joint capsule may occur either coincidentally or reflect involvement of the proximal intertarsal joint. Frequently there is secondary soreness of the epaxial muscles in the lumbar region and sometimes caudal gluteal muscle soreness. The toe and branches of the shoe of the lame limb, or both limbs, may wear abnormally. In our experience, shoe wear in this location, however, is not pathognomonic of distal hock joint pain. Some horses, if not properly trimmed, develop lateral flare of the hoof and mediolateral foot imbalance, with the foot higher medially. Lameness may worsen when shoe additives such as toe grabs and heel calks are applied, an observation that can be useful in therapeutically shoeing a horse with distal hock joint pain (see later). Flexion of the limb may be resisted slightly, but marked lifting of the limb during flexion is more likely to reflect stifle pain. The Churchill test (see Chapter 6) is helpful in identifying distal hock joint pain in some, but by no means all, horses. Soreness associated with specific acupuncture points (see Chapter 92) can also be suggestive of distal hock joint pain.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree