CHAPTER 34 The Respiratory System
Normal Respiratory System Development
In some scenarios when assisted mating and elective cesarean section delivery are planned, there may be uncertainty regarding adequate development of surfactant. Inadequate surfactant in the neonate will complicate peripartum management. While the puppies are still fetal and before delivery, the presence of surfactant can be indirectly documented using the “foam stability test.” This technique was originally used in human obstetric medicine as a rapid test to determine the timing of a cesarean section. One milliliter of amniotic fluid is collected (via ultrasound-guided centesis or laparotomy) and is mixed with 1 ml of 100% ethanol in a glass tube. The solution is then vigorously shaken for 15 seconds. If surfactant is present, a ring of bubbles will form at the fluid-air interface and remain for at least 15 minutes (Figure 34-1). In human obstetrics, this method was used as a surgery room test to indicate fetal readiness for delivery. Results of this test in elective cesarean section delivery of canine fetuses have indicated that adequate surfactant production is not present until 62 days past the luteinizing hormone (LH) surge for female canine fetuses and 63 days past the LH surge for male canine fetuses. This sex difference is consistent with observations in human obstetrics, as female fetuses begin surfactant production earlier than males.
Clinical Examination of the Respiratory System
Respiratory Patterns
Definition of the phase of the respiratory cycle showing the greatest alteration in respiratory effort can be helpful in defining an initial list of differential diagnoses and formulating a diagnostic plan. The general characteristics of the two main pathological respiratory patterns, obstructive and restrictive, are summarized in Table 34-1. Respiratory diseases that lead to restriction of the airway diameter typically present with an obstructive breathing pattern. In a patient presenting with a typical obstructive breathing pattern, respiratory rate is mildly to moderately increased, and the depth of respiratory excursions is usually increased. Obstructive breathing patterns may be seen with conditions affecting either the extrathoracic or intrathoracic airways. With obstructive lesions in the upper airways, inhalation tends to cause worsening obstruction as a result of decreasing airway diameter. Therefore patients with upper airway obstruction tend to show increased respiratory effort on inhalation. The reverse applies in lower airway obstructive diseases, as the diseased airways are more likely to collapse during exhalation, leading to increased expiratory effort. Respiratory diseases that limit the ability of the lungs and airways to expand lead to a restrictive breathing pattern. Inability to expand the lung parenchyma leads to a reduction in respiratory excursions. Patients presenting with restrictive breathing patterns show a shallow depth of respiration and increased respiratory rate in an attempt to maintain adequate ventilation. Restrictive breathing patterns may be seen with diseases affecting either the lung parenchyma or the pleural space. In particular, space-occupying lesions of the pleural cavity (e.g., pleural effusion, diaphragmatic hernia, pneumothorax, and pleuroperitoneal or peritoneopericardial hernias) may severely restrict the ability of the lungs to expand during inflation.
TABLE 34-1 Characteristics of obstructive and restrictive breathing patterns
| Pattern | Obstructive | Restrictive |
|---|---|---|
| Respiratory depth | Increased | Shallow |
| Respiratory rate | Normal to mild increase | Markedly increased |
| Inspiratory dyspnea | Extrathoracic airways | Not typically distinguished |
| Expiratory dyspnea | Intrathoracic airways | Not typically distinguished |
Thoracic auscultation is an integral part of the physical examination of animals with respiratory disease. The thorax of the neonate and very young puppy and kitten is much smaller than in adults. Auscultation with specific neonatal and pediatric stethoscopes is recommended to increase accuracy when attempting to localize respiratory sounds. The neonatal puppy has a normal respiratory rate at rest between 25 and 35 breaths/min for the first 2 weeks of life. Between 3 and 4 weeks of age, the normal respiratory rate decreases to between 15 and 25 breaths/min. After 4 weeks, most puppies show respiratory rates appropriate for adult dogs, including the onset of panting for thermoregulation. In theory, animals with upper airway obstructive disease have louder respiratory sounds on inhalation. Lower airway obstructive diseases (e.g., feline asthma) will tend to have louder respiratory noise on exhalation. In practice, it is often difficult to localize respiratory pathology with this degree of certainty. Even when signs of the respiratory pathology are localized to one area, this does not rule out the presence of disease in other regions. Animals with restrictive pulmonary diseases tend to have an overall reduction in the volume of breath sounds. Pleural effusions tend to settle to the ventral pleural cavity; therefore lung sounds may be muffled ventrally and prominent dorsally. In patients with pneumothorax, on the other hand, the lungs may settle ventrally, leading to muffled lung sounds dorsally. Although the lung sounds overall are decreased with restrictive diseases, auscultation directly over the partially collapsed lung tissue may reveal harsh respiratory sounds and pleural friction rubs. Common differential diagnoses of obstructive and restrictive breathing patterns are summarized in Box 34-1.
Congenital Anomalies of the Respiratory System
Brachycephalic Airway Syndrome
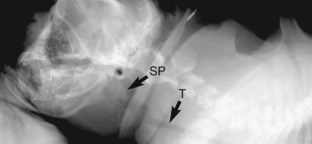
A diagnosis of brachycephalic airway syndrome should be suspected in any brachycephalic animal presented for respiratory distress. Diagnosis of the component disorders of this syndrome typically requires a combination of clinical examination, upper airway examination via laryngoscopy, and diagnostic imaging. Stenotic nares are readily visible during physical examination. Elongation of the soft palate can be documented via visual examination of the distal pharynx or radiographic examination of the upper airways (Figure 34-2). The normal soft palate should just overlap the epiglottis, whereas in brachycephalic airway syndrome the soft palate extends more than 3 mm caudal to the tip of the epiglottis and may completely occlude the epiglottic opening. In symptomatic individuals, early resection of the elongated soft palate is associated with a better long-term prognosis. Although the technique for surgical resection of an elongated palate is relatively simple, these patients represent a significant anesthetic risk and must be managed aggressively in the perioperative period to avoid swelling of the surgical site and acute upper airway obstruction. Placement of a temporary tracheostomy may be required in some patients.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree