Chapter 1 Surgical instrumentation
Design of ophthalmic instruments
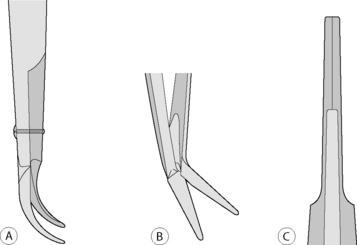
Thumb forceps and scissors for corneal and intraocular procedures are usually hinged with different mechanisms to facilitate their opening. The three most common hinges include the X-hinge, the vertical pin hinge, and the bar hinge (Fig. 1.1). The common X-hinge for scissor blades or needle holder tips is usually joined by small screws or pins, and often the handles converge to become spring mechanisms that maintain the instrument in an open position. With vertical pin hinges, as in iris scissors, the hinge pin is deformed as the scissor blade is closed to act as a spring device to open the blades upon release. The bar hinge is typical of most thumb forceps, and consists of the junction of the base of both handles; tension of these handles closes the forceps blades and release results in the forceps tips opening. All of these hinges are very delicate and, if extended too far, can easily bend or break.
Ophthalmic surgical instruments
• Table 1.2 – instruments for orbital surgeries
• Table 1.3 – instruments for eyelid surgeries
• Table 1.4 – instruments for conjunctival and corneal surgeries
• Table 1.5 – instruments for intraocular and cataract surgeries
Table 1.2 General surgical instruments for orbital surgeries
| Instrument | Purpose |
|---|---|
| Allis tissue forceps | Hold and position tissues |
| Bard–Parker™ handle and blades | Incise the eyelids |
| Bishop–Harmon forceps, toothed | Grasp the conjunctiva and nictitans |
| Cannula: 19 g | Irrigation of the external eye |
| Enucleation scissors, large, curved | Incise the optic nerve |
| Eyelid speculum, wire | Retract the lids and maintain the palpebral fissure |
| Wet field or disposable cautery | Hemostasis |
| Jameson muscle hook | Manipulate the extraocular muscles |
| Metzenbaum scissors, medium | Incise and separate the orbital tissues |
| Mosquito forceps (2 curved, 2 straight) | Grasp tissues and for hemostasis |
| Needle holder, medium | Grasp and manipulate needle |
| Saline cup, small | Hold saline for moistening of tissues |
| Silicone bulb for irrigation | Irrigate the external eye |
| Tenotomy scissors, curved | Incise the conjunctiva and nictitans |
| Towel clamps (4 large, 4 small) | Maintain the surgical drapes |
Table 1.3 Surgical instruments for eyelid surgeries
| Instrument | Purpose |
|---|---|
| Towel forceps (4 large, 4 small) | Secure the drapes to the patient |
| Wire eyelid speculum (Barraquer) | Retract the lids and expose the conjunctiva/nictitans |
| Small curved Mayo scissors (Mayo/Metzenbaum) | Perform lateral canthotomy |
| Stainless steel cup | Hold saline/lactated Ringer’s solution for ocular irrigation |
| Silicone bulb and cannula | Periodically moisten the eye |
| Entropion/chalazion forceps | With an oval-to-round ring and solid base plate. Designed to clamp and stabilize the lid |
| Cilia forceps | With smooth tips designed to epilate the cilia |
| Bishop–Harmon forceps | Both serrated and 1 × 2 teeth tips. Good general tissue forceps |
| Lid plate | Plastic or stainless steel. Holds the lids taut and protects the cornea from surgical manipulations |
| Beaver™ scalpel handle | Use Beaver No. 6400 or 6700 microsurgical blade to incise eyelid skin/conjunctiva |
| Standard needle holder (Castroviejo/Barraquer) | Standard size recommended to accommodate the larger needles and suture sizes. Some prefer holders with a lock device |
| Tenotomy scissors (Steven’s) curved/straight | Two different sizes recommended. Blunt tips preferred |
Table 1.4 Surgical instruments for conjunctival and corneal surgeries
| Instrument | Purpose |
|---|---|
| Instruments for both surgeries | |
| Towel clamps (8) | Secure surgical drapes |
| Small curved Mayo scissors (Mayo/Metzenbaum) | Lateral canthotomy |
| Stainless steel cup | Hold saline/lactated Ringer’s solution |
| Silicone bulb and cannula | Periodically moisten the eye |
| Wire lid speculum (adult/pediatric: Barraquer) | Retract eyelid/expose cornea |
| Small needle holder | Suture lateral canthotomy |
| Tissue forceps: tooth/smooth (Adson) | Grasp conjunctiva/cornea |
| Beaver™ scalpel handle (Nos 6400 and 6500 microsurgical blades) | Incise cornea |
| Tenotomy (Steven’s) scissors | Cut conjunctiva/sutures |
| Castroviejo needle holder | Use with 5-0 to 10-0 sutures |
| For corneal surgeries | |
| Corneal section scissors (right/left pair) | Cut cornea/limbus/sclera |
| Martinez or Gill dissector | Bluntly separate corneal stromal layers |
| Calipers | Operative measurements |
| Cyclodialysis spatula | Manipulate iris, lens, vitreous |
| Disposable ophthalmic cautery | Hemostasis/cut iris |
| Corneal trephines (5–9 mm) | For keratoplasty |
| Microsurgery needle holder | For keratoplasty |
Table 1.5 Surgical instruments for intraocular surgery in animals
| Instrument | Purpose |
|---|---|
| Towel clamps (4 large, 4 small) | Secure surgical drapes |
| Small curved Mayo scissors | Lateral canthotomy |
| Saline cup | Hold saline/lactated Ringer’s solution |
| Silicone bulb and cannula (cannula: 19 g/25 g) | Periodically moisten the eye |
| Eyelid speculum (adult/pediatric) | Retract eyelid/expose cornea |
| Small needle holder | Suture lateral canthotomy |
| Tissue forceps: toothed/smooth (Adson) | Grasp conjunctiva/cornea |
| Tying forceps with teeth | Grasp cornea/sutures |
| Beaver scalpel handles (Nos 6400, 6500, and 6700 microsurgical blades and keratome) | Incise cornea/limbus/sclera |
| Tenotomy scissors (Steven’s) | Cut conjunctiva |
| Utility scissors (Steven’s tenotomy) | Cut sutures |
| Corneoscleral scissors (right/left pair) | Incise cornea/limbus/sclera |
| Iris scissors | Incise iris |
| Extracapsular lens forceps | Grasp anterior lens capsule |
| Capsulectomy forceps (Utrata) (capsulorhexis) | Tear/remove anterior lens capsule |
| Lens loop | Slide lens from eye |
| Cyclodialysis spatula | Separate tissues |
| Muscle hook (Jameson) | Rotate globe/cataract surgery |
| Needle holder (standard/microsurgery) | Suturing |
| Other | |
| Calipers | Operative measurements |
| Disposable cautery (sterile) | Hemostasis/cut iris |
| Intraocular forceps | Grasp/remove lens capsule/fragments |
| Intraocular scissors | Cut anterior lens capsule |
| Vannas capsulotomy scissors | Cut anterior lens capsule |
| Intraocular lens forceps/hook | Position or dial intraocular lens |
Box 1.1 Recommended instruments and materials for vitreoretinal surgeries*
General
• Good quality operating microscope.
• Viewing system for the posterior segment: Machemer irrigating lens, other sew-on ring sets, or non-contact BIOM system. A more expensive wide-angle system is available. Both systems can be used in dogs. These systems use indirect ophthalmoscope principles (which invert the ocular fundus appearance) and may require an inverter for use.
• Vitrectomy system with light-illuminating sources, electrocautery, and air infusion. Newer units may also have ultrasonic fragmentation and silicone oil pumps. The vitrectomy unit is usually a guillotine-type cutter on the side of a 20 g blunt tube.
Instruments
These instruments are presented in further detail.
Eyelid specula
Eyelid specula are used to retract the eyelids and enhance exposure of the conjunctiva, cornea, and globe. The ideal eyelid speculum should be strong enough to retract the eyelids to the maximal amount possible, but sufficiently lightweight to prevent direct pressure on the cornea and globe. The most versatile eyelid speculum for small animals is the wire type. For most breeds of dogs and cats, the Barraquer wire speculum is preferred with 14 mm blades and an overall length of 40 mm (Fig. 1.2). The pediatric size Barraquer speculum may be useful in young and smaller animals; its blades are 11 mm and overall length is 34 mm.
In large dogs and large animals a heavier eyelid speculum may be necessary. Eyelid specula, such as the Guyton–Park (14 mm blades and overall length of 85 mm), Castroviejo (15 or 16 mm blades and overall length of 75–82 mm), and Williams (10 mm blades and overall length of 90 mm) can provide maximum exposure of the palpebral fissure (Fig. 1.3). Sometimes for the lid speculum to conform to the eyelid and palpebral curvatures of the horse and cow, the arms of the specula are bent slightly. With all eyelid specula, the blades should extend beneath the eyelid margins for several millimeters to adequately retract the eyelids and reduce the possibility of dislodgement. In some species, like the avian species, the palpebral fissures and eyelids are very small, and a single 4-0 to 6-0 silk suture is placed in each eyelid to keep the lids open.
Tissue forceps
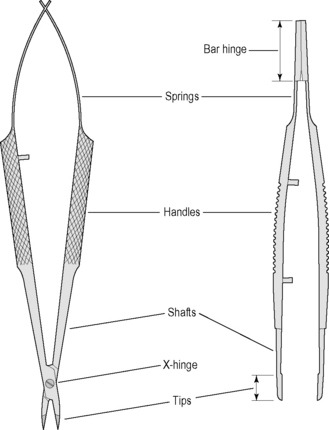
The different types of ocular tissue have resulted in the development of a large selection of tissue forceps with specialized tips. These tissue forceps vary by tips, shaft, handles, springs, and bar hinge (Fig. 1.4). The handles of these forceps are usually flat with serrations or knurling on the handles to facilitate their grasp. Microsurgical forceps usually have angled tips, and are about two-thirds the total length of standard ophthalmic instruments. The arms of these forceps are hinged at the base, and this hinge provides sufficient tension to maintain the tips about 5–10 mm apart. Upon digital compression, the tissue forceps tips should completely and perfectly contact each other. The tips of many forceps are angulated to prevent blockage of the surgeon’s view during surgery.
The major difference of the ophthalmic tissue forceps is their tips, which have highly specialized indications (Table 1.1). In selecting these tissue forceps, one should handle them individually and use those forceps that ‘feel’ the most comfortable.
Table 1.1 Tips of tissue forceps used for corneal and intraocular surgery
| Tip design | Designated tissue(s) or use | Appearance |
|---|---|---|
| Von Graefe | Conjunctiva/nictitans | 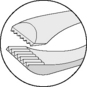 |
| 1 × 2 teeth | Cornea/conjunctiva | |
| Splay | 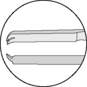 | |
| Dog-toothed | 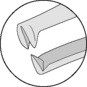 | |
| Colibri style tip angulation | Cornea/conjunctiva | 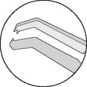 |
| Serrations | Cornea/conjunctiva | 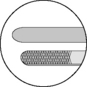 |
| Tying platforms | Tying small sutures | 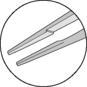 |
| Lens capsule | ||
| Extracapsular | Grasp/tear anterior lens capsule | 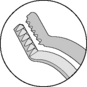 |
| Intracapsular | Grasp/hold anterior lens capsule | 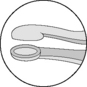 |
| Utrata | Anterior capsulorhexis | 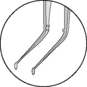 |
| Intraocular | Grasp/remove lens capsule and fragments | 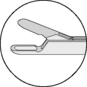 |
| Combination 1 × 2 teeth tying platform | Cornea/conjunctiva and tying sutures | 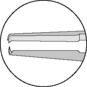 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree