6 Natural progression of disease
ORAL EXAMINATION – UNDER GENERAL ANAESTHETIC
See the front page of the dental record for details of findings (Fig. 6.1a) and the back page of the dental record for details of the treatment performed (Fig. 6.1b).
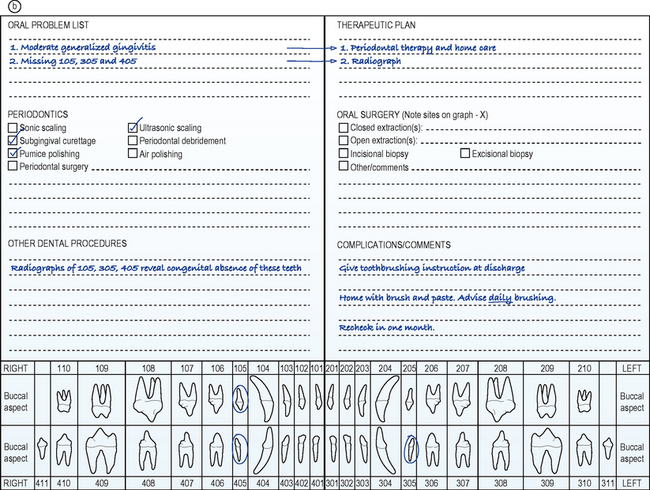
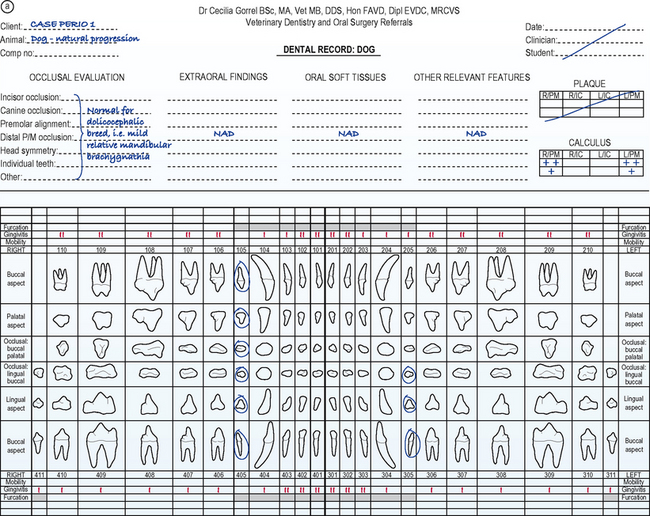

Figure 6.1 Front page (a) and back page (b) of the dental record.
After Gorrel C, Derbyshire S (2005): Veterinary Dentistry for the Nurse and Technician, with permission of Elsevier. After Gorrel C, Derbyshire S (2005): Veterinary Dentistry for the Nurse and Technician, with permission of Elsevier.
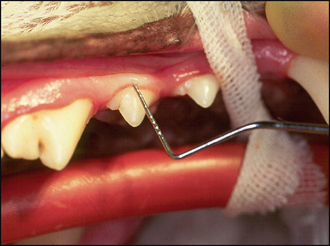
In summary, examination under general anaesthesia confirmed the moderate generalized gingivitis (Fig. 6.2a, b). There was no evidence of periodontitis, i.e. no gingival recession and no increased periodontal probing depth at any site (Fig. 6.3). There was moderate accumulation of calculus, especially on the buccal aspect of the upper fourth premolar and first molar bilaterally (Fig. 6.2a).
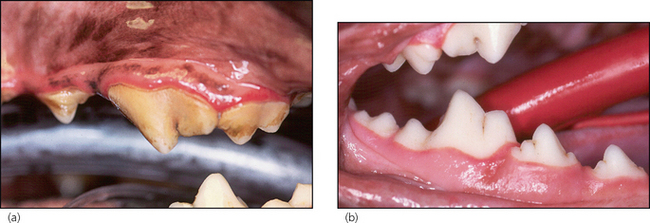
Figure 6.2 Lateral photographs of the left upper premolar and molar region (a) and of the right lower jaw (b).
THEORY REFRESHER
In gingivitis, the plaque-induced inflammation is limited to the soft tissue of the gingiva. Sulcus depths are normal (i.e. periodontal probing depths are 1–3 mm in the dog and 0.5–1 mm in the cat). As periodontitis occurs, the inflammatory destruction of the coronal part of the periodontal ligament allows apical migration of the epithelial attachment and the formation of a pathological periodontal pocket (i.e. periodontal probing depths increase). If the inflammatory disease is permitted to progress, the crestal portion of the alveolar process begins to resorb. Alveolar bone destruction type and extent are diagnosed radiographically. The resorption may proceed apically on a horizontal level. Horizontal bone destruction is often accompanied by gingival recession, so periodontal pockets may not form. If there is no gingival recession, the periodontal pocket is supraalveolar, i.e. above the level of the alveolar margin. The pattern of bone destruction may also proceed in a vertical direction along the root to form angular bony defects. The periodontal pocket is now intra- or subalveolar, i.e. below the level of the crestal bone.
The following parameters need to be assessed and recorded for each tooth in all patients:
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree