CHAPTER 11 Miscellaneous Conditions
Osteomyelitis
Osteomyelitis in the jaws most commonly arises from dental infections and persistent infected roots (Figure 11-1). Infection that has spread into the bone is more difficult to resolve due to the establishment of a bacterial biofilm with its inherent protective mechanisms. Acute osteomyelitis may exhibit no radiographic abnormalities. Established infection usually appears as an area of relative radiolucency with poorly defined margins (see Chapter 6).
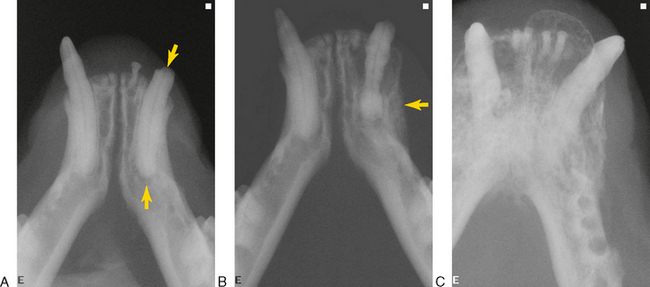
FIGURE 11-1 Osteomyelitis in cats. A, Fractured mandibular left canine tooth with pulp exposure (arrow). The periapical area is characterized by a periapical lucency of endodontic origin (open arrow) (see Chapter 6). The roots of multiple incisor teeth persist. B, The patient in A was not treated and returned 2 years later. The canine root tip is displaced coronally as the tooth is supererupted (a misnomer in carnivore dentition). The coronal periodontal ligament is widened due to marginal alveolar expansion, and there is periosteal reaction and bone deposition on the labial aspect of the left mandible (arrow). These are all signs of localized osteomyelitis. C, Osteomyelitis secondary to periodontitis. The considerable bony reaction and enlargement give the radiographic appearance of a neoplastic process.
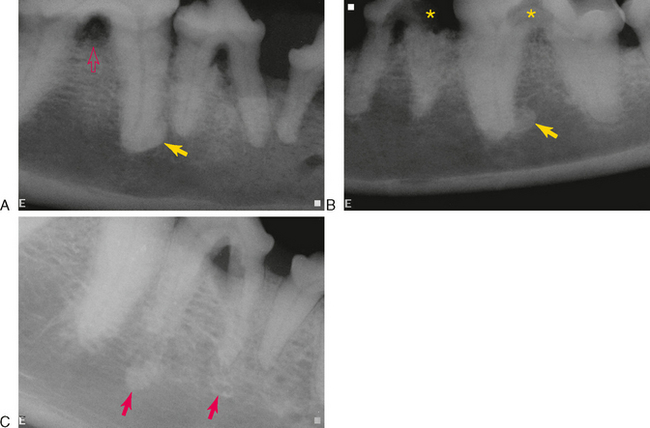
Sclerosing osteomyelitis (condensing osteitis, bony scar, sclerotic bone, focal periapical osteopetrosis) is an inflammatory condition believed to be a local bony reaction to a low-grade inflammatory stimulus or to bacteria of low virulence. Focal sclerosing osteitis appears radiographically as an opacity at, or in the vicinity of, the apex or lateral canal of a tooth that has had a long-lasting pulpitis (Figure 11-2). The periodontal ligament and root remain distinct from the opacity. The focal lesion may be uniformly opaque, may be peripherally lucent with an opaque center, or may be composed of confluent or lobulated opaque masses. The radiographic appearance can be similar to that of periapical cemental dysplasia, complex odontoma, osteoblastoma, and hypercementosis.
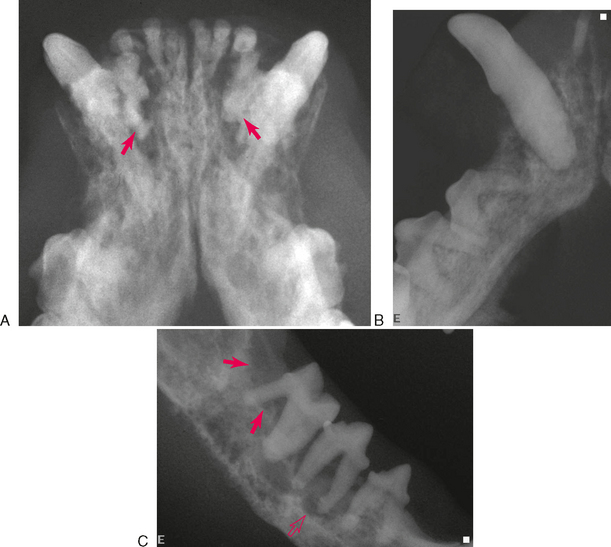
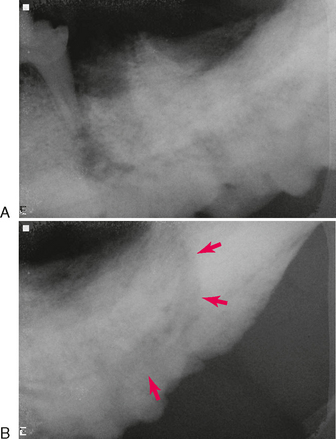
The diffuse form of sclerosing osteomyelitis affects a larger area of the jaw. Early in the course, there are lucent zones in association with sclerotic masses (Figure 11-3). In advanced stages, it is characterized by a generalized increased opacity (Figure 11-4).
Opacities Not Caused by Inflammation or Infection
Osteosclerosis can also occur in the absence of inflammation or infection (Figure 11-5). A common site in humans is the septal bone between premolar teeth. One theory suggests the cause is persistent fragments of primary teeth that become encapsulated by cementum.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree