Ryan A. Ferris
Mating-Induced Endometritis
Persistent mating-induced endometritis (PMIE), a noninfectious inflammatory condition of the uterus, is one of the most common reproductive abnormalities encountered by veterinarians who specialize in equine reproduction. Persistent mating-induced endometritis refers to the accumulation and retention of inflammatory fluid in the uterus for more than 48 hours after breeding. Failure to evacuate the intrauterine fluid and inflammation that follow breeding leads to reproductive inefficiency and economic loss to the mare owner.
Pathogenesis
Semen passes into the uterus during both artificial insemination and natural breeding. Spermatozoa induce a transient inflammatory response by activating complement and stimulating the innate immune system. The inflammatory response peaks 8 to 12 hours after breeding and is usually resolved within 24 hours. It has been proposed that the inflammatory response to spermatozoa is a normal physiologic event that is necessary to clear the uterus of defective, dead, and excess spermatozoa and other debris introduced during breeding.
Failure to resolve this normal inflammatory event is referred to as PMIE. In mares with PMIE, inflammatory fluid containing neutrophils, immunoglobulins, proteins, spermatozoa, and potentially bacteria accumulates in the uterus. This inflammatory fluid exacerbates the inflammatory response, resulting in additional inflammation. The result is a perpetual cycle of prolonged neutrophil migration into the uterine lumen, uterine inflammation, increased fluid accumulation, and further inflammation. When the embryo enters the uterus 5 to 6 days after ovulation, the inflammatory environment in the uterine lumen leads to impaired embryo survival.
Failure to clear fluid from the uterus following breeding is the result of a combination of factors such as delayed uterine clearance, cervical abnormalities, and alterations in production of inflammatory cytokines. Delayed uterine clearance is an alteration of the normal progressive uterine contractions that facilitate fluid clearance in normal mares. This change in uterine contractility is a major component of development of PMIE. Narrowing or occlusion of the cervical lumen is observed in mares with cervical adhesions or lacerations and in older (>15 years) maiden mares. Mares with these cervical defects can have normal uterine contractions, but because of reduced cervical opening, only a minimal volume of fluid is able to pass from the uterus through the cervix into the vagina. After an inflammatory response is initiated, immune-modulating cytokines such as interleukin-10 (IL-10) and IL-1Ra are produced to return the local tissue from an inflammatory condition back to homeostasis and, if ongoing inflammatory response is still warranted, to prevent the destruction of local cells and tissue. A significant reduction in immunomodulatory cytokines is found in mares prone to PMIE at all stages of the estrus cycle and after breeding. The combination of an inability to clear spermatozoa and the inflammatory fluid from the uterus, with reduced immune modulatory cytokines, creates an environment of chronic inflammation.
Clinical Signs and Diagnosis
Mares with PMIE typically appear normal (i.e., no intrauterine fluid is seen on ultrasound, and negative findings on endometrial culture and cytology) at presentation. Mares at risk for PMIE are often older (>15 years of age) and have a Kenny biopsy score of 2 or greater. A thorough history is often the most rewarding element of a diagnostic workup for identifying mares prone to developing PMIE. Typically, if a mare has developed PMIE in previous seasons, problems with fluid clearance will continue in the future.
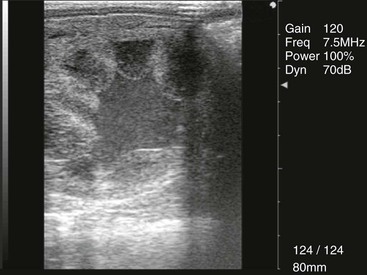
It is not uncommon for a mare to have no indication of uterine clearance problems until an ultrasound examination is performed 24 hours after breeding, when a large volume of fluid is observed (Figure 165-1). An endometrial cytology sample can be collected to confirm the nature of the fluid in the uterine lumen, in which neutrophils and spermatozoa may be observed (Figure 165-2). This is not often done in routine practice, however, because the fluid can be assumed to be from development of PMIE.
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


