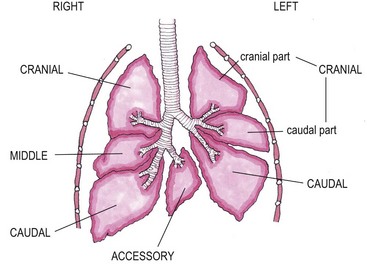
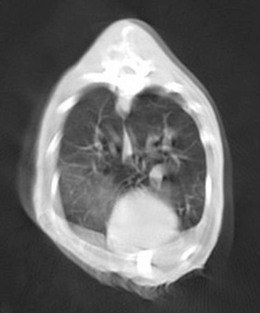
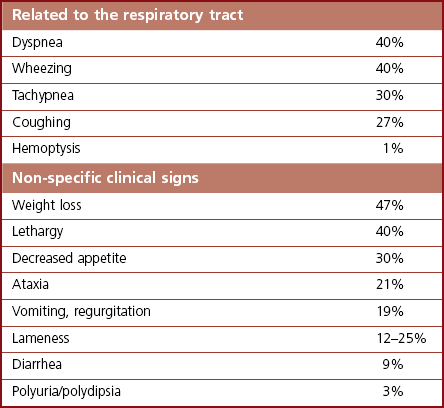
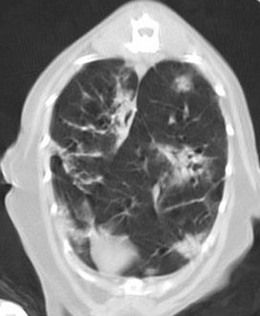
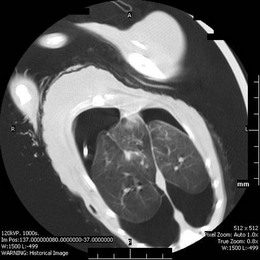
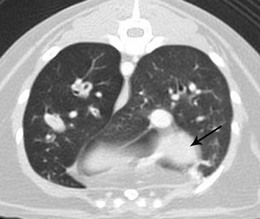
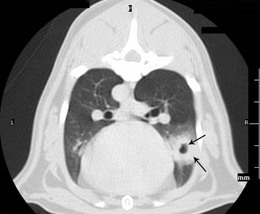
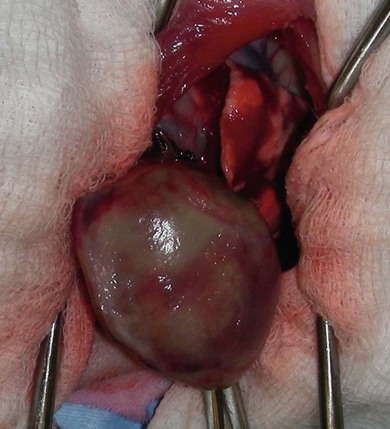
Chapter 47 The lungs expand to fill most of the thoracic cavity. The smaller left lung is divided into cranial and caudal lobes by interlobular fissures, with the left cranial lobe having a further partial division into cranial and caudal parts. The right lung is divided into cranial, middle, caudal, and accessory lobes (Fig. 47-1) and the hilus of the accessory lung lobe passes dorsal to the caudal vena cava to sit medial to the plica vena cava. Laterally the lungs are bordered by the thoracic wall and caudally by the diaphragm, separated by the pleura and the pleural space. Cranially the lungs are adjacent to the thymus when it is prominent in the younger cat. A full radiographic assessment of the lungs should ideally include left and right lateral projections. However, if the patient is unstable it is important that emergency procedures (e.g., thoracocentesis) are performed prior to radiography as the stress of handling and positioning for radiography could precipitate respiratory arrest. Inflated views taken under anesthesia are always preferable if possible as this provides additional information, such as a higher likelihood of identifying the presence of small primary or metastatic nodules. However, sedation and/or anesthesia are only advisable in patients who are clinically stable. If the patient is dyspneic a single dorsoventral radiograph may be the only possible view obtainable in the initial stages of assessment. However, it is always important to note that one limitation of radiography is that it is not always possible to correctly identify the anatomical location of disease or the primary disease focus (e.g., bronchial, interstitial, alveolar).1 Advanced imaging techniques such as ultrasound, computed tomography (CT), and scintigraphy may identify abnormalities not visible on radiography (e.g., lung metastases) and may also further facilitate surgical planning e.g., by identifying affected lung lobes to guide surgical approach.2 Some abnormalities may be seen with ultrasound, such as consolidation, atelectesis, and pulmonary masses.2 However, the technical difficulties of ultrasound of the lungs caused by the inability of ultrasound waves to pass through air limit its usefulness to lesions located in an entire lung lobe or at the periphery of lung lobes adjacent to the thoracic wall.3,4 CT is the preferred imaging modality for pulmonary disease and the CT findings in normal cats and those with pleural, pulmonary, and mediastinal diseases have been well described (Box 47-1).2,5,6 CT can be successfully performed without chemical restraint in cats by using a positioning device,7 but it is more usual to perform CT under sedation or general anesthesia. There will inevitably be some movement blur during CT as there is for radiography and MRI, but this can be minimized by hyperventilation prior to scanning and then undertaking the scan during the expiratory pause (Figs 47-2 and 47-3).6 Aspiration of any pleural fluid or air that may be present prior to CT will improve pulmonary parenchymal visualization by allowing increased lung inflation,8 while the administration of intravenous contrast agents can also improve the detection of pulmonary lesions.7,8 CT provided additional correct diagnoses in 28% of cats undergoing conscious CT compared to conscious radiography, as well as further additional information in 74% of cats. Overall, 40% of cats undergoing both techniques had a significant different disease or prognosis following CT imaging (Box 47-2). Figure 47-2 Conscious computed tomographic image (cat in dorsal recumbency) showing cortication of the lung lobes and thickening of the pleura. (© Alison Moores.) Fluid obtained by bronchoalveolar lavage (BAL) should always be examined cytologically for evidence of neoplastic or inflammatory cells and for evidence of active infection but samples are more likely to be diagnostic for neoplastic disease when there are large lesions involving central rather than peripheral lung.16 The limitations of BAL include failure to sample a representative area of disease, low cellularity, the difficulty sometimes encountered differentiating neoplasia from epithelial hyperplasia, the presence of marked inflammation obscuring and hindering identification of other cells, and the inability to analyze cells in relation to airway architecture.1 In addition, many different underlying diseases, including neoplasia and septic or non-septic inflammation can all lead to neutrophilic inflammation being present, thereby sometimes making it difficult to make a definitive diagnosis by cytology alone.1 Hemosiderosis on tracheal wash samples is common but a non-specific finding.17 Any fluid obtained by either BAL or tracheal wash techniques should always be submitted for culture, although there may not be a correlation between culture results from BAL and lung tissue obtained by biopsy if aspiration of oral and pharyngeal bacteria into the lower airways has occurred during the sampling procedure, so every care should be taken to avoid this if possible.1 Where radiography and cytology from BAL fail to establish a diagnosis, obtaining a biopsy for histologic analysis may be useful. Transthoracic fine needle aspiration can be performed blindly after a lesion has been identified on diagnostic imaging or, more preferably, using ultrasound, fluoroscopic or CT guidance.4,18,19 Ultrasound-guided aspiration can either be performed conscious or with sedation,4 but undertaking a biopsy procedure necessitates deep sedation or anesthesia. Aspirates can certainly help differentiate neoplastic from non-neoplastic disease and therefore guide clinical decision making, but biopsy is often required to determine exact tumor types.4 A solid tissue sample is also more likely to be diagnostic for diseases affecting pulmonary architecture, e.g., fibrosis, emphysema, bronchiectasis.20 Contraindications for obtaining biopsies include coagulopathies, pulmonary bullae, severely compromised pulmonary function, and pulmonary hypertension.4 Potential complications encountered after a biopsy procedure include pneumothorax or pulmonary hemorrhage,4,19 and it is important to counsel owners in this regard before such a procedure is performed. In most instances, obtaining a tissue sample for histology requires open thoracotomy (see Chapter 41), but where available, thoracoscopy in the cat is considered a less invasive technique than thoracotomy for examining the thoracic cavity and obtaining tissue for histologic evaluation21 and should always be considered (see Chapter 42). Primary pulmonary neoplasia is rare in cats, with a reported annual incidence in one study of 2.2 per 100 000 cats,22 while a further study reported an incidence of pulmonary neoplasia of 0.38% of cats examined at necropsy.23 Affected cats are generally middle to old-aged and tumor development is independent of feline immunodeficiency virus or feline leukemia virus infection.24 No predisposing causes of feline pulmonary neoplasia have been identified.24 Most tumors encountered are malignant and of epithelial origin (98–100%), of which adenocarcinomas are the most common (85–100%).10,12,25 Adenocarcinomas are not easily differentiated by topographic nomenclature (bronchial versus bronchiolar versus bronchioloalveolar) due to the extent of disease at diagnosis, and some are classified as adenosquamous carcinomas if there is significant squamous differentiation.26 It is therefore more common to describe them as differentiated or undifferentiated, which is more useful clinically as it relates to prognosis.10 Undifferentiated adenocarcinomas appear to occur most commonly (43–69%) and are more invasive and metastatic than the less frequently reported differentiated adenocarcinomas.10,25,26 Other epithelial malignancies such as anaplastic carcinoma and squamous cell carcinoma appear to be less common, while sarcomas and benign tumors are rarely reported.10,27,28 Other reported pulmonary tumors in cats are listed in Box 47-3. Additionally, there has been a report of a mediastinal mass in a cat, which was consistent with bronchogenic adenocarcinoma. The author suggested that it originated from an accessory embryonic lung.29 The reported clinical signs of cats with pulmonary neoplasia are summarized in Table 47-1. Interestingly, respiratory signs are reported to only occur in 33–62% of cats,10,12,25,27,28 and in some cats lameness was the only presenting complaint. Lameness may occur from metastatic spread to the digits, appendicular bones or skeletal muscles or, more rarely, hypertrophic osteopathy.34,39,47 Invasion of the esophagus may cause gastrointestinal signs such as vomiting or regurgitation.24,27 Significant changes on serum biochemistry and hematology are unusual.25 Paraneoplastic conditions are occasionally recognized, including hypercalcemia, thrombocytopenia and leukocytosis, and are most likely due to humoral factors produced by the tumor.41–43 Such paraneoplastic syndromes may resolve after tumor excision,41 but specific further medical management is still required in some cases. When diagnosing pulmonary neoplasia via radiography, a variety and sometimes a combination of patterns may be present including a solid circumscribed mass, lobar consolidation, a nodular interstitial pattern, or a diffuse alveolar/reticulonodular pattern (Figs 47-4 and 47-5).12 Solitary masses tend to be well circumscribed whereas multiple masses are usually more poorly circumscribed.12 Mass lesions may also be cavitated (0–22%) or calcified (6–12%) (Fig. 47-6).12,27 When comparing three large studies of feline primary pulmonary tumors, the radiographic presentations are found to vary (Table 47-2)12,25,27 with no recognized association between the radiographic findings and the tumor type.12,25 In a further study in which 79 of 86 cats with pulmonary neoplasia had radiographs taken, 53 cats had single or multiple masses and the remaining cats had a pleural effusion. The 86 cats subsequently had a postmortem or surgery and 40 cats were found to have a single well-circumscribed mass, 37 had lobar consolidation (Fig. 47-7), and nine had multiple masses.25 Further postmortem studies have shown that multiple lung lobes are often affected in cats with a diffuse radiographic pattern and radiography may fail to identify single or multiple masses subsequently found on direct visualization of the lungs.12,27 Table 47-2 Radiographic presentation of cats with primary pulmonary neoplasia12,27,28 Multiple radiographic findings were present in some cats.28 Figure 47-4 Transverse CT image of the thorax showing the presence of a mass in the accessory lung lobe just ventral to the caudal vena cava (arrow). Differential diagnoses include primary neoplasm and abscess. (© Alison Moores.) Figure 47-6 Transverse CT image of the thorax of a cat. Rounded area of dense alveolar infiltration with centrally located gas-filled cavity. Differential diagnoses include primary neoplasm with cavitation and abscess. (© Alison Moores.) Figure 47-7 A consolidated lung lobe seen via an intercostal thoracotomy. Histopathology of the lobe demonstrated a moderately differentiated adenocarcinoma. (© Alison Moores.) When evaluating the most common location for primary pulmonary neoplasia, one study showed an approximately even distribution of pulmonary tumors between left unilateral, right unilateral and bilateral disease, but another study reported a low incidence of bilateral disease.12,27 However, it does appear that the caudal lung lobes are more commonly affected than the cranial lobes.10,12,27 Squamous cell carcinomas and bronchioloalveolar carcinomas are reported to primarily affect the middle and peripheral parts of the lungs whereas focal adenocarcinomas may occur throughout any region of the lung lobe.12 Reported incidences of pleural effusion and lymphadenomegaly also vary, with 9–65% cats reported as having a concurrent pleural effusion.10,12,25,27 Rarely, non-neoplastic disease such as ectopic hepatic parenchyma mimics lung neoplasia on radiography.9 Further complication can arise from the fact that pulmonary neoplasia may look similar radiographically and histopathologically to fibrotic interstitial lung disease and both diseases may exist concurrently.44 Radiography may fail to detect neoplasia, either because it is not recognized or the radiographic changes are misinterpreted, and therefore it is not possible to ascertain estimates for false positive or false negative diagnoses based on radiographic studies alone.12 Ultrasonography can detect pulmonary masses that contact the thoracic wall, but the interposition of air in normal lung tissue will preclude visualization of many mass lesions. Ultrasonography can be useful for assessing regional lymph nodes but CT allows more accurate localization of masses and detection of smaller macroscopic disease than radiography.2 Cytology is a useful diagnostic tool for pulmonary neoplasia10,25 and samples can be obtained by transthoracic or transbronchial aspiration or by bronchial brushing. A correct diagnosis was obtained in 80–86% of the cats in which samples were obtained by blind or guided fine needle aspiration through the thoracic wall and assessed cytologically.10,25 However, as needle tract implantation of neoplastic cells on the thoracic wall after ultrasound-guided fine needle aspiration of a pulmonary adenocarcinoma has been reported,45 care should be taken to consider this possibility whenever fine needle aspirates are planned. Cytology can also be useful in the assessment of pleural fluid or BAL fluid for malignant cells, but as their presence is variable the absence of neoplastic cells does not rule out disease.1,25,27 Furthermore, as sarcomas do not typically exfoliate well, the diagnostic value of pleural fluid or a BAL for sarcomas may be less than that for carcinomas.1 False positive diagnosis of neoplasia on BAL cytology has been reported only rarely in cats with inflammatory disease, but care should always be taken with interpretation in the presence of marked inflammation.1 Immunohistochemistry of biopsy samples can be used to characterize the cell of origin.1,24 Inflammation and hemosiderosis is common in BAL samples from cats with confirmed or suspected pulmonary neoplasia (100 and 79%, respectively).17 Aerobic and anaerobic bacterial culture and fungal culture should always be performed to rule out pulmonary abscess as a differential diagnosis or to recognize concurrent infection associated with a neoplasm.17,46
Lung
Surgical anatomy
General considerations and diagnostic procedures
Diagnostic imaging
Biopsy and laboratory analysis
Surgical diseases
Primary pulmonary neoplasia
Imaging
Radiographic description
Incidence
Solid, circumscribed mass
39%
Lobar consolidation
23%
Diffuse alveolar or reticulo-nodular pattern
33%
Multiple diffuse nodules/nodular interstitial patterna
45%
Multiple small circumscribed nodules
15%
Normal
8%
Pleural effusion
49%
Cytology
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Lung