33 Complicated crown fracture with periapical disease
ORAL EXAMINATION – CONSCIOUS
Conscious examination of this extremely aggressive dog was not possible.
ORAL EXAMINATION – UNDER GENERAL ANAESTHETIC
In summary, examination under general anaesthesia identified the following:
RADIOGRAPHIC FINDINGS
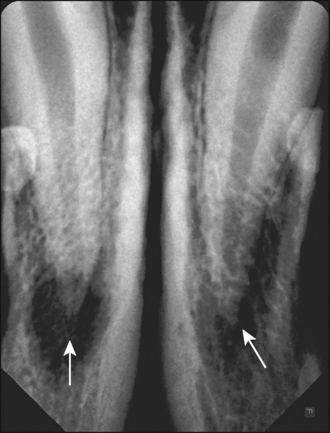
All four canines were mature teeth with closed apices. Periapical destruction and external root resorption were evident with all four canine teeth. The periapical lesions were more extensive in the lower jaw (Fig. 33.1), and had resulted in thinning and expansion of the ventral cortical bone.
THEORY REFRESHER
The crown fracture has exposed the pulp, resulting in pulpal inflammation. The teeth are mature, i.e. the apices are closed, so the injury must have occurred when the dog was more than 1 year old. The inflammatory response has spread to involve the periapical region, resulting in destruction of the periapical bone. This is evident as an apical rarefaction on a radiograph. The bone defect is filled with soft tissue, which may be granulation tissue (periapical granuloma), cyst (periapical or radicular cyst) or abscess (periapical abscess). Definitive differentiation between these three possibilities requires histopathology of the tissue. The periapical cyst usually occurs as a sequel to the periapical granuloma. It is a true cyst since the lesion consists of a pathological, often fluid-filled, cavity that is lined by epithelium. Periapical cysts enlarge due to the osmotic gradient set up between the lumen of the cyst and tissue fluids in the surrounding connective tissue. These lesions can become very large at the expense of the adjacent bone tissue, which is resorbed (due to pressure from the cyst). Periapical lesions may be entirely asymptomatic or excruciatingly painful. The periapical granuloma and periapical cyst rarely cause severe discomfort, but they may undergo exacerbation and develop into a periodontal abscess, which usually is an extremely painful condition.