15 Chronic gingivostomatitis with extraction leading to partial cure
ORAL EXAMINATION – UNDER GENERAL ANAESTHETIC
In summary, examination under general anaesthesia identified the following:
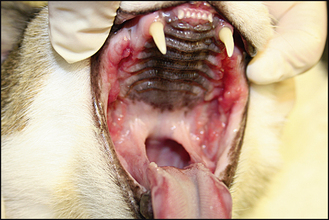
2. Gingivostomatitis (alveolar, buccal and glossopalatine mucosae) affecting the premolar and molar regions in all four quadrants (Fig. 15.1)