16 Canine chronic gingivostomatitis
ORAL EXAMINATION – CONSCIOUS
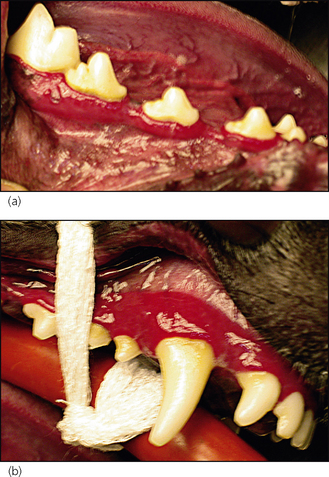
Conscious oral examination was allowed, which revealed intense halitosis and gingivostomatitis (Fig. 16.1a). The mandibular lymph nodes were enlarged and seemed painful on palpation.
ORAL EXAMINATION – UNDER GENERAL ANAESTHETIC
In summary, examination under general anaesthesia identified the following:
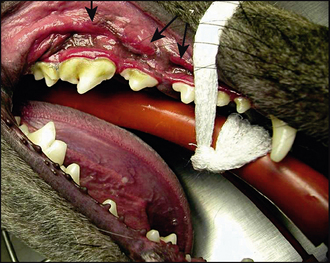
4. Moderate amounts of plaque and calculus were present on the buccal aspects of the upper premolars and molars (Fig. 16.2)
THEORY REFRESHER
It is thought to be an inappropriate response to oral antigens, namely bacterial plaque present on the tooth surfaces. While underlying vesiculo-bullous disease, e.g. pemphigus and pemphigoid or discoid lupus erythematosus (DLE), cannot be excluded, it is essential to have plaque control before these can be investigated.
In the dog, I approach CGS as follows:
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree