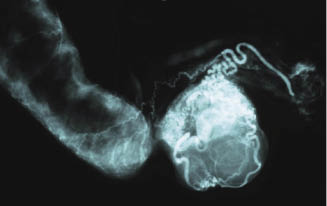
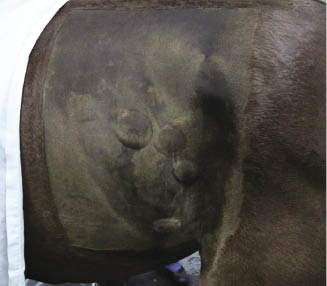
Figure 17.2 A mare with excessive internal body fat. Fat is bulging from the paralumbar fossa and the mesocolon.
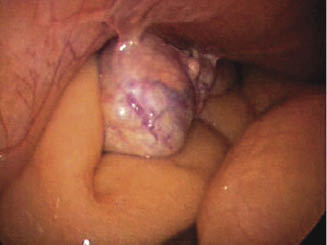
Mares that are anticipated to be nervous in the stocks prior to surgery are premedicated with acepromazine at about 0.03–0.06 mg/kg IM 30 minutes prior to loading into the stocks. Before laparoscopy, the horse is administered penicillin G potassium (22,000 U/kg [10,000 U/lb], IV), gentamicin sulfate (6.6 mg/kg [3 mg/lb], IV), and flunixin meglumine (1.1 mg/kg [0.045 mg/lb], IV).
The horse is led into a standing operating room, restrained in stocks, and positioned to gain access to the paralumbar fossae. Extra stall mats can be stacked at the rear of the stocks to achieve a 10- to 12-cm elevation of the pelvis to aid viewing of the caudal abdomen. Detomidine hydrochloride (0.015 mg/kg [0.0068 mg/lb], IV) and butorphanol tartrate (0.025 mg/kg [0.011 mg/lb], IV) are administered. Sedation is maintained with detomidine hydrochloride continuous rate infusion (CRI) and adjusted as needed (0.1 mg/kg/min). The hair over the caudal thorax, paralumbar fossae, and caudal flanks are clipped, and the sites are prepared for surgery with chlorhexidine surgical scrub solution alternated with sterile gauze soaked in saline (0.9% NaCl) solution. The rectum is manually evacuated and a urinary catheter is aseptically placed for the duration of the operation.
Instrumentation
| 1 | 57-cm 30° laparoscopic telescope |
| 1 | Video camera, monitor, light source, insufflator |
| 1 | 5-mm, 32-cm, 18-ga tip laparoscopic injection needle |
| 2 | 5- to 12-mm laparoscopic cannula assemblies |
| 2 | 10-mm laparoscopic cannula assemblies |
| 1 | 5- or 10-mm traumatic grasping forceps |
| 1 | 10-mm vessel-sealing device (LigaSure) |
| 1 | Morcellator |
Items to have available
- Ligating loops
- Hemoclips
- Staples
- Semm claw forceps
- Specimen bag
- 10-mm × 20-cm laparoscopic cannula assemblies
- 5-mm laparoscopic scissors
Surgery
The primary task of the operation is to achieve excellent hemostasis during transection of the ovarian pedicle (Figure 17.3) and removal of the ovary from the abdominal cavity. Practically every method available for use in operations has been applied to ovariectomy of the horse. An excellent review of these has been published (Lee & Hendrickson 2008; Shettko & Hendrickson 2008). This surgical description will focus on a two-portal technique utilizing vessel-sealing technology and morcellation.
After draping the surgical areas, 2% mepivacaine hydrochloride (20–40 mL) is infiltrated throughout the full thickness of the body wall with special attention to the skin at each of the four portal sites. Intradermal injection of the local anesthetic is performed, creating a 3- to 5-cm wheal over each portal site (Figure 17.4). An additional intradermal site can be injected at the ventral aspect of the drape fenestration to permit towel clamp application (Figure 17.5).
Figure 17.4 Local anesthetic injection creating a ∼5-cm intradermal wheal followed by deep infiltration to the peritoneum.
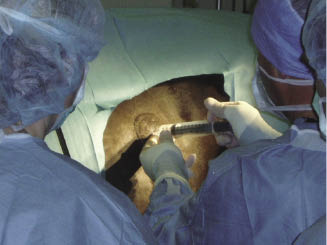
On the mare’s left side, the first portal (laparoscope) is located at the level of the ventral tuber coxae and between the last two ribs. To avoid possible penetration of the pleural space, it is important that the intercostal portal is not located dorsal to a horizontal line from the most ventral aspect of the tuber coxae (Figure 17.6). The second portal (instruments) is located 5 cm below the dorsal margin of the internal abdominal oblique muscle midway between the last rib and tuber coxae. On the right side, the first portal is located just dorsal to the internal abdominal oblique muscle and just caudal to the last rib. The second portal is located 5 cm distal and caudal to the first portal. A 15-mm skin incision is made over the first portal location on the left side. A 10- to 12-mm portal sheath with conical obturator is placed into the abdominal cavity (Figure 17.7). The obturator is removed and replaced with a 50-cm-long, 10-mm-diameter, 30° angle viewing laparoscope.
Figure 17.6 To avoid penetration of the left pleural cavity, a portal in the 17th intercostal space is placed below a horizontal line from the most ventral aspect of the tuber coxae.
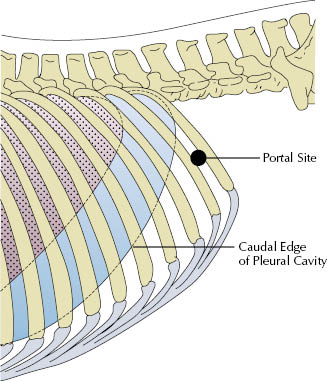
Figure 17.7 Depth of portal insertion to penetrate the peritoneum at the 17th intercostal space on a horse with normal internal body fat.
If the field of view is not adequate, insufflation is used. The amount of insufflation should be kept to the minimum amount to permit viewing. Not every horse will require the use of an insufflator for adequate viewing of the ovarian pedicles. When needed, the abdomen is insufflated with carbon dioxide (CO2) (7 L/min) for ∼4 minutes with adjustments as needed and then turned off, the goal being to allow clear viewing of the ovarian area and to provide an intra-abdominal pressure below 10 mmHg.
Once a field of view is established on the left side, the laparoscope is passed under the descending colon at the level of the bladder and then directed dorso-cranial, providing a view of the right paralumbar fossa area. A 15-mm skin incision is made over the first portal site, and a 5- to 12-mm sheath and obturator is inserted using the laparoscopic view to confirm placement into the abdominal cavity. The second portal on the right is placed using an identical technique. The laparoscope is withdrawn from under the descending colon and focused on the intra-abdominal location of the paralumbar fossa for the second portal on the left side; it again is placed under laparoscopic guidance to confirm cleanly entering the abdominal cavity.
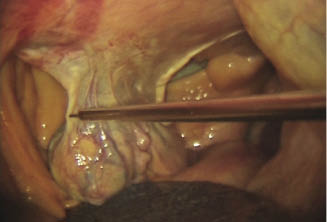
After all four portal sheaths are established, a long injection needle is placed in the newly established port and 30–60 mL of 2% lidocaine is infiltrated along the mesovarium of the ovary (Figure 17.8). The needle is withdrawn from the portal and a vessel-sealing device (LigaSure, Covidien, Mansfield, MA) is inserted to begin the removal of the ovary. The instrument is capable of both vessel sealing and transection of the mesovarium with each placement of the jaws. The cutting function is activated by a trigger on the instrument handle and should only be used when vessel sealing has been successful, as indicated by visual assessment of tissue reaction to the energy source and the correct audible signal from the unit. The maximum length of tissue that the jaws will accommodate is 20 mm. Transection can begin at the cranial or caudal aspect of the ovary. It is technically easier to begin at the cranial aspect as the angle of approach is straight and the mesovarium is a single-layer structure with a free leading margin at that point as compared to the double-layer structure (proper ligament and mesosalpinx) at the caudal attachments to the uterine horn. If the mare has excessive adipose tissue in the mesovarium, extra caution should be taken to assure hemostasis. When the pedicle becomes too thick due to fat to allow secure closure of the handle, the pedicle should be split sagittally using the jaws of the vessel-sealing instrument. This will reduce the thickness of the tissue placed between the jaws, allow transection of the pedicle to progress, and improve hemostasis. It is also possible to perform a double seal over the area of the ovarian artery by placing the first grasps of the jaws more dorsal on the mesovarium and releasing the jaws after sealing without triggering the scissors. The next placement of the jaws should be just ventral to the last seal, this time completing another sealing cycle and transecting. As the transection continues, a 5-mm band of attached mesovarium should be preserved to suspend the ovary for morcellation (Figure 17.9). Care should be taken to transect the robust proper ligament of the ovary and not use that structure for suspending the ovary for morcellation (Figure 17.10). There is risk of damage to the uterine horn by pulling it into the morcellator if the proper ligament of the ovary remains attached to the ovary. If at anytime during the operation an additional laparoscopic instrument would augment the viewing and dissection of the ovary, a 5-mm portal can be established. Depending on the individual anatomy of the mare, the extra portal can be located approximately 10 cm ventral or dorsal to the existing portal in the paralumbar fossae. If the extra 5-mm portal is used, then the ovary can be suspended from the 5-mm forceps for morcellation. Once the ovary is freed from all but the small band of mesovarium, the vessel-sealing instrument and associated portal are removed. The skin incision is slightly enlarged to accommodate the 15-mm diameter of the morcellator. The obturator is placed in the 15-cm insert length barrel of the morcellator, and the assembly is placed into the abdomen. The obturator is removed and a pair of 5- or 10-mm laparoscopic tenaculum forceps (Figure 17.11) is placed through the portal of the morcellator to grasp a leading edge of the ovary. The ovary is drawn to the morcellator, and the morcellator is activated either by foot pedal or handpiece, depending on the surgeon’s preference. The morcellator has a 12- to 13-mm blade consisting of a rigid inner tube that rotates within an outer tube. The blade connects to an electric motor drive unit. When activated, the blade extends 2–4 mm out beyond the tube except in a small guarded area that extends from the outer tube to permit cutting via a peeling action. The morcellator can also be set where the cutting blade is extended beyond the guard if a core cut is needed. For morcellation of the ovary, the adjustable guard is used and set in the 6 o’clock position so it can be rotated as needed to aid in the process of morcellation. It is important that excellent viewing of the morcellation is maintained. If the view becomes obscured, the morcellator blade should be immediately disengaged until the view is reestablished. The ovary is extracted in peeled sections and, depending on the size, consistency, and configuration of the ovary, it can be removed in typically three to seven segments (Figure 17.12). The small band of mesovarium that suspends the ovary is cut by the blade of the morcellator as the final portion of suspended ovary is pulled into the portal and the portal is angled to transect the band as it is stretched over the blade edge. Alternatively, the remaining piece of suspended ovary can be grasped with 5-mm tenaculum forceps, and a pair of 5-mm scissors can be placed alongside to cut the band. Any fragments of ovary that may become separated and free in the abdomen are located and removed through the morcellator portal. Although not a common practice in the horse, free transected ovaries have been left in the abdomen with little apparent negative effect (Shoemaker et al. 2004). At the conclusion of the operation on the left side, a final check of the ovarian pedicle is performed to confirm hemostasis (Figure 17.13). The laparoscope and morcellator are then removed, and the operation is repeated on the right side.
Figure 17.8 Laparoscopic injection needle positioned to infiltrate the mesovarium of the left ovary.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree