Chapter 2 Basic Approach to Veterinary Care
Restraint and Physical Examination
Restraint
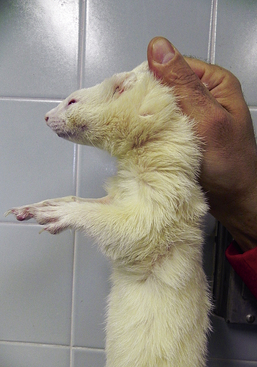
Depending on the ferret’s disposition, several basic manual restraint methods can be used for physical examination. For tractable animals, lightly restrain the ferret on the examination table. Examine the mucous membranes, oral cavity, head, and integument. Then pick the ferret up and use one hand for support under its body while using the second hand to auscultate the thorax and palpate the abdomen. The ferret can be scruffed at any time for vaccination, ear cleaning, or other procedures that may elicit an attempt to escape or bite. For a very active animal or one that bites, scruff the ferret at the back of its neck and suspend it with all four legs off the table (Fig. 2-1). Most ferrets become very relaxed with this hold, and the veterinarian is able to examine the oral cavity, head, and body; auscultate the chest; and palpate the abdomen easily. However, this method may not work for very fractious animals.
To manually restrain a ferret for procedures such as venipuncture or ultrasound, hold it firmly by the scruff of its neck and around the hips without pulling the legs back. Most ferrets struggle if their legs are extended by pulling on the feet. Some animals can be distracted during a procedure by feeding a meat-based canned food (a/d Prescription Diet, Hill’s Pet Nutrition, Topeka, KS; Eukanuba Maximum-Calorie, The Iams Company, Dayton, OH) or a small amount of a supplement such as FerreTone (8-in-1 Pet Products, Islandia, NY) by syringe. Avoid products containing sugar, which can affect blood glucose values, particularly in ferrets with insulinoma.
For very fractious or anxious animals or for procedures requiring lengthy restraint, light tranquilization or sedation may be indicated (see Chapter 31).
Physical Examination
Most ferrets strenuously object to having their temperature taken with a rectal thermometer. If a ferret struggles during the examination, the temperature taken at the end of the examination may be artificially high. Therefore measure the rectal temperature early in the physical examination with a flexible digital thermometer that is well lubricated. The normal range of rectal temperature of a ferret is 100.5°F to 102.5°F (38.0°C to 39.2°C); a mean of 102°F (38.8°C), with a wider range of 100°F to 104°F (37.8°C to 40.0°C), is also reported.21 Interestingly, in normal ferrets housed outdoors at a fur farm in very cold ambient temperatures (21°F [−6.1°C]), the mean 24-hour mean core body temperature measured by sterile thermosensitive data loggers implanted in their abdomens was 99.3°F (37.4°C), with a range of 97.3°F to 101.1°F (36.3°C to 38.4°C).41
The teeth of ferrets should be clean and the gingiva pink. Dental tartar is commonly present in pet ferrets. The amount of plaque may be exacerbated by the feeding of soft foods or sugary treats, such as raisins, and is possibly related to a dry kibble diet.14 Tartar most commonly accumulates on the first and second maxillary premolars. Excessive dental tartar should be removed by dental techniques used in dogs and cats, and measures to prevent tartar buildup should be implemented. As a preventive, a pet dentifrice or tartar control toothpaste25,32 can be applied to the teeth to decrease formation of calculus. Gingivitis, which manifests as erythematous gingival tissue that sometimes bleeds, is a common sequela of excessive dental tartar.
Ferrets often break off the tip of one or both canine teeth; however, they rarely exhibit clinical signs of sensitivity or pain associated with a fractured canine. If the tooth turns dark or the ferret exhibits sensitivity when eating, recommend a root canal or extraction, depending on the degree of damage to the tooth (see Chapter 32). Rarely, an infected root of a fractured canine can cause swelling of the ipsilateral submandibular lymph node. If swelling is present, dental radiographs, canine tooth extraction, and possibly lymph node biopsy are indicated.
Observe the symmetry of the face. Although uncommon, salivary mucoceles occur in ferrets and are noticeable as a unilateral swelling on the side of the face, usually in the cheek or temporal area (see Chapter 3).
Auscultate the heart and lungs in a quiet room. Ferrets have a rapid heart rate (180 to 250 beats/min) and often a pronounced sinus arrhythmia. If a ferret is excited and has a very rapid heart rate, subtle murmurs may be missed. Valvular disease, cardiomyopathy, and congestive heart failure are seen in ferrets, and any murmur or abnormal heart rhythm should be investigated further (see Chapter 5).
Palpate the abdomen while holding the ferret off the table, either by scruffing the neck or supporting the ferret with one hand. This allows the abdominal organs to displace downward, facilitating palpation. If the history is consistent with an intestinal foreign body or urinary blockage, palpate gently to avoid causing iatrogenic injury, such as a ruptured stomach or bladder. Palpate the cranial abdomen, paying particular attention to the presence of gas or any irregularly shaped mass in the stomach area, especially in ferrets with a history of vomiting, melena, or chronic weight loss. The spleen is commonly enlarged in ferrets; this may or may not be significant, depending on other clinical findings (see Chapter 5). Palpate a large spleen gently to avoid iatrogenic damage. A very enlarged spleen may indicate systemic disease or, very rarely, idiopathic hypersplenism, and further diagnostic workup is warranted. Always note any degree of splenic enlargement in the medical record so that this finding can be rechecked at future examinations.
Check the fur coat for evidence of alopecia. Alopecia of the tail tip is common in ferrets and may be incidental and transient or an early sign of adrenal disease. Symmetric, bilateral alopecia or thinning of the hair coat that begins at the tail base and progresses cranially is a common clinical finding in ferrets with adrenal disease. Examine the skin on the back and neck for evidence of scratching or alopecia. Pruritus may be present with adrenal disease (common) or with ectoparasites (fleas, Sarcoptes scabiei). Check closely visually and by searching through the hair coat with your fingers for evidence of skin masses. Mast cell tumors are common and can range in diameter from a few millimeters to over a centimeter. Often, the fur around a mast cell tumor is parted and matted with dark blood from the animal’s scratching. Other types of skin tumors, such as sebaceous adenomas and basal cell tumors, are also common (see Chapter 9). Perform an excisional biopsy of any lump found on the skin.
Preventive Medicine
Young, recently purchased ferrets need serial distemper vaccinations until they are 13 to 14 weeks of age.2 Rabies vaccines should be given annually beginning at 3 months of age.15 Ferrets should be examined annually until they are 4 or 5 years of age; middle-aged and older animals should be examined twice yearly because of the high incidence of metabolic disease and neoplasia. Annual blood tests (consisting of a complete blood count and plasma or serum biochemical analysis) are recommended for older animals. Measure the blood glucose concentration twice yearly in healthy middle-aged and older ferrets; more frequent monitoring is needed in ferrets with insulinoma. An endocrine panel is indicated in ferrets with hair loss on the tail or other clinical signs suggestive of early adrenal disease (see Chapter 7). Testing for infectious diseases may be warranted, especially in new ferrets that will be introduced into a multi-ferret household or those that are taken to ferret shows. Currently, ferrets can be tested for Aleutian disease virus and ferret enteric coronavirus by polymerase chain reaction (PCR) testing (Michigan State University, Diagnostic Center for Population and Animal Health, www.animalhealth.msu.edu; Veterinary Molecular Diagnostics, www.vmdlabs.com). Serologic tests for Aleutian disease by enzyme-linked immunosorbent assay (ELISA) and counterimmunoelectrophoresis (CIEP) are also available (see Chapter 5).
Vaccinations
Canine Distemper
Ferrets must be vaccinated against canine distemper virus. Currently, one vaccine is approved by the U.S. Department of Agriculture for use in ferrets: PureVax (Merial, Athens, GA). Because PureVax is a canarypox-vectored recombinant vaccine it does not contain adjuvants or the complete distemper virus; thus many of the postvaccination risks have been reduced. This product has a wide safety margin and has proved effective in protecting ferrets against canine distemper infection.58 Another distemper vaccine that was widely used previously (Fervac-D, United Vaccines, Inc., Madison, WI) is no longer available. Fervac-D was a modified live virus vaccine propagated in avian cell lines. Another modified live canine distemper vaccine (Galaxy D, Merck/Schering-Plough Animal Health, Whitehouse Station, NJ) has been studied for safety and efficacy in ferrets. This product, derived from the Onderstepoort distemper strain and attenuated in a primate cell line, proved effective in preventing canine distemper in young ferrets challenged after serial vaccination.64 However, duration of immunity with this product is not known, and its use in clinical animals is extralabel, requiring informed owner consent. Although no vaccine reactions were reported in the study, the incidence of vaccine reactions with Galaxy D is unknown because experience with repeated long-term use in ferrets has been limited.64 Because of the possibility of vaccine-induced disease, especially in immunosuppressed or sick ferrets, do not use combination canine vaccines or vaccines of ferret cell or low-passage canine cell origin.
In young ferrets, the half-life of maternal antibody to canine distemper virus is 9.43 days.2 Vaccinate young ferrets for distemper at 8 weeks of age, then give two additional boosters at 3-week intervals for a total of three vaccinations. Give booster vaccines annually.
Rabies
All ferrets should be vaccinated against rabies.15 A killed rabies vaccine is approved for use in ferrets (Imrab-3 or Imrab-3 TF, Merial, Duluth, GA) and is effective in producing immunity for at least 1 year.55 Current recommendations are to vaccinate healthy ferrets at 3 months of age at a dose of 1 mL administered subcutaneously. Give booster vaccinations annually. Titers develop within 30 days of rabies vaccination.55
In ferrets that were experimentally inoculated intramuscularly with skunk-origin rabies virus, the mean incubation period was 33 days and the mean morbidity period was 4 to 5 days.42 Clinical signs were ascending paralysis, ataxia, cachexia, bladder atony, fever, hyperactivity, tremors, and paresthesia. Virus antigen was present in the brain tissue of all ferrets with clinical signs of rabies, and virus was isolated from the salivary gland of one ferret. In a similar study of ferrets inoculated with a raccoon rabies isolate, the mean incubation period was 28 days. Virus was isolated from the salivary glands of 63% of rabid ferrets, and 47% shed virus in saliva. Virus excretion began from 2 days before until 6 days after the onset of illness.43 In an earlier study of ferrets with experimentally induced rabies, only mild clinical signs were observed before death.7 Infected ferrets exhibited restlessness and apathy, and some showed paresis. Sick animals did not attempt to bite when threatened, and virus was not excreted in the submaxillary salivary glands of animals that died. In this study, the authors concluded that ferrets are 50,000 times less susceptible to rabies than fox and 300 times less susceptible than hares. In another study, ferrets that were fed up to 25 carcasses of mice infected with rabies did not develop the disease; in contrast, skunks become fatally infected after the consumption of only one carcass.4
Ferrets are considered currently immunized 28 days after the initial rabies vaccination and immediately after a booster vaccination.15 If a healthy pet ferret bites a person, current recommendations of the Compendium of Animal Rabies Prevention and Control are to confine and observe the animal for 10 days; the ferret should not be vaccinated during this period.15 If signs of illness develop, this should be reported to the local health department and a veterinarian should evaluate the animal. If signs suggest rabies, the ferret must be euthanized and protocols for rabies evaluation should be followed. If a stray ferret bites a person, the ferret must be euthanized and submitted immediately for rabies testing. For a vaccinated ferret exposed to a possible rabid animal, recommendations are to revaccinate the ferret immediately and quarantine for 45 days. An unvaccinated animal that is exposed to a rabid animal should be euthanized immediately and submitted for rabies testing. See the website of the Centers for Disease Control and Prevention (www.cdc.gov/mmwr/preview/mmwrhtml/rr5702a1.htm) or the National Association of Public Health Veterinarians (www.nasphv.org/) for specific guidelines.
Vaccine-Associated Adverse Events
In ferrets, adverse events associated with vaccination are primarily type I hypersensitivity reactions or anaphylaxis.37 Type I hypersensitivity reactions involve lymphoid tissue associated with mucosal surfaces (skin, intestines, and lungs) and result from the interaction of antigen and immunoglobulin E in mast cells or basophils. Ferrets with mild reactions may exhibit pruritus and skin erythema. More severe reactions are typified by vomiting, diarrhea, piloerection, hyperthermia, cardiovascular collapse, or death.
Vaccine reactions are most common after distemper vaccination but may also occur after rabies vaccination. In a study of vaccine reactions in 3,857 ferrets, the incidence of adverse events associated with rabies vaccine alone, distemper vaccine alone, and rabies and distemper vaccines together were 0.51%, 1.0%, and 0.85%, respectively. The incidence of adverse events did not differ significantly among these three groups; however, the cumulative number of distemper vaccinations received was significantly associated with the occurrence of an adverse event. The distemper vaccines used in this population of ferrets were PureVax and Fervac D; however, the two distemper vaccines were grouped collectively in the analysis, and the incidence of adverse events associated with the individual distemper vaccines was not reported. Sex, age, and body weight were not associated with occurrence of an adverse event. All reactions occurred immediately after vaccination and most commonly consisted of vomiting and diarrhea. In another study of 143 ferrets, the incidence of adverse events after administering distemper (5.9%) (Fervac D), rabies (5.6%) (Imrab-3), or both vaccines (5.6%) was not significantly different. In a 2001 report of vaccine reactions in ferrets reported to the United States Pharmacopeia Veterinary Practitioners’ Reporting Program, 65% (54 of 83) of reports involved administration of FerVac D; 24% (20 of 83) involved concomitant administration of FerVac D and Imrab; and 11% (9 of 83) involved administration of Imrab alone (PureVax was not approved for use at the time these data were collected).37 According to Merial’s product information, the incidence of vaccine reactions with PureVax is 0.3%. No data are available for products not licensed for use in ferrets. Veterinarians are not required to report vaccine-associated adverse events, and surveillance of these events is passive, relying on voluntary reporting by practitioners.37 Vaccine-associated adverse events can be reported to the Center for Biologics, U.S. Department of Agriculture (1-800-752-6255; www.aphis.usda.gov/animal_health/vet_biologics/vb_adverse_event.shtml).
Vaccine injection-site sarcomas have been described in ferrets.39,40 In one report, 7 of 10 fibrosarcomas in ferrets were from locations used for vaccination.39 Fibrosarcomas from injection sites had a high degree of cellular pleomorphism and similar histologic, immunohistochemical, and ultrastructural features as those reported for feline vaccine-associated sarcomas. In the reported cases in ferrets, no definitive association could be made between the fibrosarcoma and the type of vaccine. In cats, adjuvanted vaccines are most likely to be involved in tumor development. However, although injection-site sarcomas may occur in ferrets, ferrets appear less prone than cats to tumor development. In a study of vaccine reactions in ferrets, mink, and cats, cats had more lymphocytes at the injection site than either ferrets or mink after vaccination with three different rabies vaccines.11 Results of this study suggest a lower species susceptibility to vaccine-associated sarcomas in ferrets than in cats.
Parasites
Endoparasites
Coccidiosis (Isospora species) is seen infrequently, usually in young ferrets, which shed oocysts between 6 and 16 weeks of age.3 The infection is usually subclinical; occasionally, however, ferrets may have loose stool or bloody diarrhea. Treatment of ferrets with coccidiosis is similar to that of other small animals and should be continued for at least 2 weeks. Coccidiostats, such as sulfadimethoxine and amprolium, are effective and safe. The Isospora species that infect ferrets may cross-infect dogs and cats; therefore other pets in the household should be checked for coccidia and treated as needed.
Giardiasis is occasionally seen in ferrets. Results of a recent study on molecular characterization of Giardia duodenalis isolates from pet ferrets show that genetic sequences from isolates in ferrets differ from isolates of humans and other animals, suggesting that Giardia isolates from ferrets may be host specific.1 Giardia species can be detected by identifying cysts or trophozoites in a fresh fecal smear or zinc sulfate flotation, or by fecal ELISA. Treat ferrets with giardiasis with metronidazole (20 mg/kg PO q12h) for 5 to 10 days. Fenbendazole (50 mg/kg PO q24h for 3 to 5 days) is used in dogs and cats, but safety and efficacy in ferrets are unknown.
Cryptosporidiosis can occur in a high percentage of young ferrets.53 Infection is usually subclinical in both immunocompetent and immunosuppressed animals. Although most immunocompetent animals recover from infection within 2 to 3 weeks, infection can persist for months in immunosuppressed animals. Oocysts of Cryptosporidium are small (3 to 5 μm) and difficult to detect but can be found in samples of fresh feces examined immediately after acid-fast staining.3,53 No treatments exist for Cryptosporidium infection. Because of the zoonotic potential, ferrets may be a source of infection for human beings, especially immunocompromised individuals with acquired immunodeficiency syndrome (AIDS).53
Heartworms (Dirofilaria immitis) can cause disease in ferrets. Ferrets that are housed outdoors in heartworm-endemic areas are most susceptible to infection; however, all ferrets in endemic areas should be given preventive medicine. Oral administration of ivermectin is currently the most practical preventive measure because it is administered once per month (see Chapter 5 and Appendix).
Ectoparasites
Ear mites (Otodectes cynotis) are common in ferrets, but affected animals rarely exhibit pruritus or irritation. This mite species also infects dogs and cats, and animals in households with multiple pets can transmit mites to other animals. A red-brown, thick, waxy discharge in the ear canal and pinna characterizes infection. A direct smear of the exudate reveals adult mites or eggs. Because ferrets normally have brown ear wax, the color or appearance of debris in the ear canal is not pathognomonic for mites. At the initial examination, check all ferrets for ear mites and do follow-up checks at the annual examination in ferrets kept in multiple-pet households. Several products, including selamectin, are effective in treatment (see Chapter 9).
Flea infestation (Ctenocephalides species) is most common in ferrets kept in households with dogs or cats. Ferrets with chronic infestation can become severely anemic. Check all ferrets during the physical examination for signs of fleas or flea dirt. Treat infested animals with products safe for use in cats and institute flea control measures (see Chapter 9).
Ticks are rarely seen in domestic ferrets, and Lyme disease in ferrets has not been reported.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree