20 Small Airway Disorders
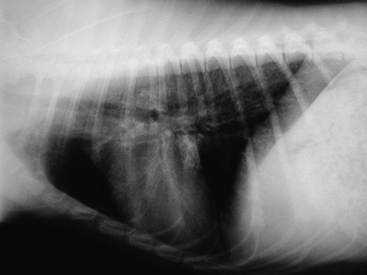
The minimum database of complete blood count, serum chemistry, and urinalysis is helpful to exclude other causes of coughing. Heartworm serologic and fecal examinations should be included to rule out possible parasitic disease. Some cases of bronchitis will demonstrate a peripheral eosinophilia; polycythemia may be seen as a result of chronic hypoxia; serum alkaline phosphatase and alanine aminotransferase may be increased. Pulmonary function testing is becoming a more commonly used diagnostic tool. Arterial blood gas analysis may demonstrate hypoxemia (oxygen pressure less than 80 mm Hg at sea level). A concurrently elevated carbon dioxide pressure is associated with a poorer prognosis. Thoracic radiographs are an important part of the workup for bronchitis. They also are important for ruling out other differentials for coughing (e.g., congestive heart failure, neoplasia). Normal thoracic radiographs do not rule out the possibility of bronchitis. The most commonly reported changes on radiographs are a result of increased thickening of bronchial walls. These thickened walls are termed “tram lines” when viewed longitudinally and “doughnuts” when viewed in cross section. An increased interstitial pattern is also associated with bronchitis. However, one study found a similar frequency of interstitial patterns in dogs with bronchitis and normal controls. This same study showed only thickened bronchial walls and increased numbers of visible bronchial walls as significantly increased in dogs with bronchitis. Figure 20-1 shows a lateral thoracic radiograph of a dog with chronic bronchitis, demonstrating multiple “doughnuts” and prominent airway markings. Pulmonary hyperinflation and diaphragmatic flattening have been reported, though these are more common in cats. Bronchoscopy with bronchoalveolar lavage is considered the diagnostic test of choice for chronic bronchitis. It is recommended that this procedure be performed early in the course of the disease, when the animal’s respiratory status is not severely compromised and anesthesia is still relatively safe. Bronchoscopic findings in affected airways include: erythema, mucus, nodular proliferation, irregular mucosa, and, potentially, dynamic airway collapse. Cytologic evaluation of airway secretions in dogs with active disease shows primarily neutrophilic inflammation. Other cell lines that may be present include eosinophils and macrophages. Curschmann’s spirals also may be present. Samples should be obtained for culture and sensitivity, and it is recommended to perform a quantitative assessment of bacterial numbers. Cytologic samples should also be examined for intracellular bacteria or degenerate neutrophils to help determine the significance of possible infectious agents. It has been suggested that septic inflammation, single agent bacterial cultures, atypical bacterial resistance patterns, or acute clinical exacerbations (fever, inflammatory changes in the complete blood cell count, and radiographic evidence of pneumonia) may represent better evidence for a significant bacterial infection.
Treatment is geared toward control of clinical signs and improvement in quality of life, not cure of the disease. Environmental factors should be addressed and potential airway irritants reduced or eliminated (e.g., smoke, dust, deodorizers). If the animal is overweight, a weight loss program should be instituted. If weight loss is difficult, evaluation for underlying endocrine disease should be performed (e.g., hypothyroidism, hyperadrenocorticism). Medical management generally involves antitussives, antiinflammatories, bronchodilators, and, potentially, antibiotics. Medications commonly prescribed for the treatment of chronic bronchitis is provided in Table 20-1. Antitussives are contraindicated when the cough is productive, because mucus retention can exacerbate airway inflammation and worsen disease progression. After inflammation is resolved and infection has been cleared, antitussives may be used. Sedation and constipation may be seen with these medications. The role of bronchoconstriction in chronic bronchitis is questionable. However, bronchodilators may have the beneficial effects of improving mucociliary clearance, improving diaphragmatic contractility, and allowing reduction in the dosage of glucocorticoids. Adverse effects include tachycardia, gastrointestinal upset, and excitability. Enrofloxacin, which may be a useful antibiotic for respiratory infections, impairs the metabolism of theophylline. This results in toxic levels of theophylline. Plasma levels of theophylline may be measured through human laboratories; the peak goal range is 5-20 μg/ml. If these two medications are used simultaneously, the theophylline dose should be decreased by at least 30%. In some cases, generic alternatives for theophylline may be available. The bioavailability of some of these alternatives has been questionable, so generic substitutions should be avoided in most cases. Antibiotics are indicated with concurrent bacterial infection. Ideally, antibiotic choice is based on culture and sensitivity results. If culture results are not available, and there is sufficient evidence for a bacterial infection, a bactericidal antibiotic with gram negative spectrum and good penetration into respiratory tissues (e.g., fluoroquinolone, amoxicillin/clavulanic acid) should be chosen. There has been recent discussion about the use of inhalant therapy for dogs with chronic bronchitis. There has not been clinical evidence to support the use of inhalant therapy. Other medications that have been used in cats with feline asthma (cyproheptadine, cyclosporine) would not be expected to be of benefit in the treatment of dogs with chronic bronchitis.
Table 20-1 Commonly Prescribed Medications for the Treatment of Chronic Bronchitis
| DRUG | ACTIVITY | DOSAGE (ALL DRUGS GIVEN ORALLY) |
|---|---|---|
| Bronchodilators | ||
| Terbutaline | Beta agonist | 1.25-5 mg/dog q 12 h |
| Theophylline | Methylxanthine derivative | 20 mg/kg q 12 h (sustained release) |
| Albuterol | Beta agonist | 0.02-0.05 mg/kg q 8-12 h |
| Antitussives | ||
| Hydrocodone | Opiate agonist | 0.22-1.0 mg/kg q 6-12 h |
| Butorphanol | Partial opiate agonist | 0.55-1.0 mg/kg q 6-12 h |
| Codeine | Opiate agonist | 1-2 mg/kg q 6-12 h |
| Antiinflammatories | ||
| Prednisone | Glucocorticoid | 0.5-1.0 mg/kg q 12-24 h for 5-7 days, then taper to alternate day dosing |