52 Lameness
Nerve root tumours
CASE WORK-UP
Electromyography is a useful tool. It detects an unstable muscle membrane caused by denervation and aids differentiation of orthopaedic from neurogenic causes of lameness. Lumbar CSF should be collected even in the absence of ipsilateral hindlimb signs. A compressive spinal cord lesion often results in elevated total protein levels and its presence would signal that invasion of the spinal canal has taken place. Enlargement of the intervertebral foramen by an encroaching nerve root tumour can be detected on non-contrast radiography. Myelography has been used to rule out extension of the tumour to the spinal canal. Oblique views are required. An intradural-extramedullary pattern (‘golf tee’) compression is seen. MRI and CT have replaced myelography to a large extent.
Lumbar CSF: The total protein was elevated at 0.80 g/l. WBC = 7/mm3. Cytology was normal.
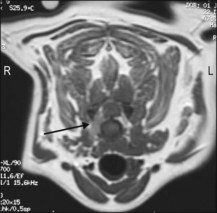
MRI showed enlargement of the right-sided C7 nerve root. And ventral compression of the cord by an irregular mass at the level of the C6–7 IVD space (Figs 52.1 and 52.2).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree