Chapter 5 Hematologic and Immunologic Diseases
Immune-mediated and hematologic disorders are commonly seen in veterinary practice. Although these diseases may be interrelated in some cases, this chapter discusses the most important diseases as individual entities. The technician is referred to a veterinary hematology text for review of the sequence of erythropoiesis and the function of the immune system; the introduction to this text also should be referenced. Knowledge of hematology and the functions of the immune system will assist the student in understanding these diseases.
ERYTHROCYTE DISORDERS
Anemia Caused by Hemorrhage
The most common cause of hemorrhage is trauma, although platelet abnormalities and abnormal clotting chemistries must be considered when determining the diagnosis. Acute hemorrhage that occurs as a result of trauma or laceration is usually an easily diagnosable problem. With acute blood loss internally the hematocrit does not reflect the severity of the problem, and as fluid shifts occur to compensate for blood loss, shock may result. Treatment should consist of controlling the hemorrhage and volume replacement.
Blood-Borne Parasites
Several commonly seen blood parasitic diseases produce anemia through hemolysis. Mycoplasma hemofelis is a common cause of anemia in cats. The parasite attaches to the erythrocyte membrane, causing increased destruction of the cells. Animals that have nonspecific signs of weight loss, anorexia, fever, hepatomegaly, and splenomegaly should have blood films examined for the presence of this microorganism. Some of these animals may be icteric on examination.
Babesia canis and Babesia gibsoni both produce hemolytic disease in the dog (Fig. 5-1). The brown dog tick Rhipicephalus sanguineus transmits these parasites. The presence of this intracellular parasite results in hemolysis of the infected red blood cells. Diagnosis is accomplished by finding the intracellular organism on blood films or by serology testing. Symptoms exhibited in the dog include hemoglobinuria, dehydration, fever, anorexia, and depression. Treatment involves tetracycline administration (for M. hemofelis) and supportive care.
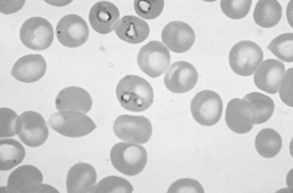
Figure 5-1 Trophozoites of Babesia canis within canine red blood cells.
(From Hendrix CM, Robinson E: Diagnostic parasitology for veterinary technicians, ed 3, St Louis, 2006, Mosby, by permission.)
Toxin-Induced Anemias/Heinz Body Anemias
Drugs can be the source of anemias in small animals. Exposure of the erythrocyte to oxidants in plasma can result in the formation of reversible and nonreversible hemichromes. When the nonreversible form is present, hemoglobin denaturation continues, forming aggregates of the irreversible hemichromes called Heinz bodies. These aggregates may be seen as large eccentric pale structures within the red blood cell of the cat, or as multiple small structures within the canine red blood cell. Cats are considered to be more susceptible to Heinz body formation because of the structure of their hemoglobin. One of the most common causes of Heinz body anemia in the dog is onion toxicity, primarily from owners treating the dog to table scraps. Clinical signs may appear several days after ingestion and they are usually those of a mild anemia. Acetaminophen toxicity also results in methemoglobinemia and anemia in dogs and cats. Toxic doses are usually the result of the owner medicating the animal. As little as half a tablet can result in clinical signs. Methylene blue, which is a urinary antiseptic used in cats, has long been known to produce Heinz body anemia when given to healthy cats. Specific diseases of clinical significance include immune-mediated hemolytic anemia (IMHA), immune-mediated thrombocytopenia (IMTP), ehrlichiosis, and von Willebrand’s disease (vWD).
Immune-Mediated Hemolytic Anemia
DIAGNOSIS
Spherocytes are commonly found on CBC.
TREATMENT



