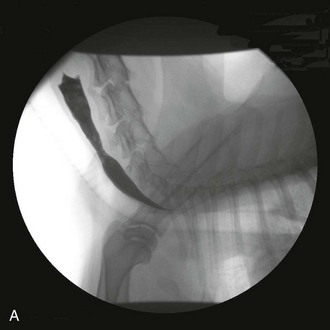
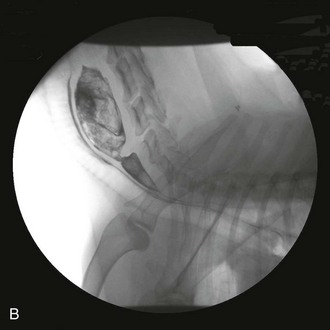
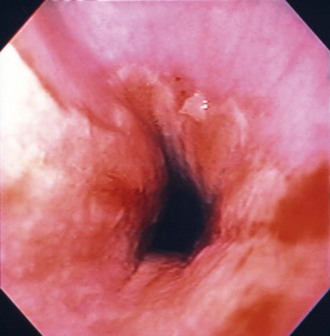
Web Chapter 49 Esophagitis (inflammation of the esophageal mucosa) is caused most often by caustic substances (e.g., gastric acid, drugs, chemicals) or trauma (e.g., foreign objects). Gastric acid can induce esophagitis when the esophageal mucosa is exposed to excessive acid because of gastroesophageal reflux (GER), frequent vomiting of gastric acid (e.g., parvoviral enteritis), or production of greater than normal amounts of acid (e.g., gastrinoma). During GER, gastric contents move into the esophagus unrelated to vomiting. Normal animals experience occasional GER without harm because esophageal peristalsis quickly returns acid to the stomach. However, severe mucosal damage may ensue when acid persists in or repeatedly enters the esophagus. Chronic esophagitis caused by spontaneous GER is documented in cats (Gualtieri and Olivero, 2006; Han, Broussard, and Baer, 2003), and it is usually the result of hiatal hernia or lower esophageal sphincter (LES) abnormalities. Anesthetized animals are a special case because acid can linger in the esophagus for long periods of time (e.g., more than 30 minutes). Anesthesia-associated reflux appears to be an important cause of esophagitis and stricture formation, with approximately 65% of esophageal strictures attributed to anesthetic-associated esophagitis in two studies (Leib et al, 2001; Melendez et al, 1998). The choice of preanesthetic and anesthetic agents, length of preoperative fasting, age, and intraabdominal versus extraabdominal procedures may influence the incidence of intraoperative GER (Wilson and Walshaw, 2004), but esophagitis caused by anesthesia-associated GER occurs erratically and unpredictably. Nonacidic damage may include drug-induced esophagitis, especially from doxycycline (Melendez, Twedt, and Wright, 2000), clindamycin, and nonsteroidal antiinflammatory drugs. Injury is usually acidic or hyperosmolar in nature, although some drugs predispose the patient to GER (Tutuian et al, 2010). Cats in particular are prone to retain tablets and capsules in their esophagus unless they are washed down with food or fluid (Bennett et al, 2010). Cats occasionally lick caustics (e.g., benzalkonium chloride) off of their fur, sustaining oral and esophageal lesions. Foreign bodies cause erosion and/or ulceration at the site of contact. Lesion severity depends on the pressure placed by the foreign object on the mucosa. Bones are the most common canine esophageal foreign objects (Rousseau et al, 2007), whereas hairballs are probably more common in cats. Foreign objects seldom cause strictures because they typically produce focal instead of circumferential inflammation. The esophagus may be infected primarily (usually fungal agents such as pythiosis) or secondarily in immunodeficient patients (e.g., dogs treated with steroids, azathioprine, or cyclosporin for immune-mediated disorders). Rarely an esophageal tumor causes mucosal inflammation. Recently, eosinophilic esophagitis has been reported in a dog (Mazzei et al, 2009). Although an important entity in people, its importance is uncertain in veterinary medicine. It appears to have an immunologic basis. Necrosis of the esophagus (i.e., “black esophagus”) is reported in people but has not been documented in dogs or cats (Altenburger et al, 2011). When the esophagus becomes inflamed, motility can be impaired, allowing food to be retained and ultimately regurgitated. More important, poor esophageal motility allows acid refluxed into the esophagus to remain longer, worsening esophagitis (Rousseau et al, 2007). LES dysfunction may occur secondary to esophagitis, allowing more GER. Chronic esophagitis caused by GER can be associated with severe histologic changes in the distal esophagus, including metaplastic changes somewhat comparable to Barrett’s esophagus in people (Gualtieri and Olivero, 2006; Han, Broussard, and Baer, 2003). If the mucosal damage is severe (e.g., penetrating to the muscularis), healing may be accompanied by cicatrix and esophageal stricture. Most strictures resulting from GER occur between the thoracic inlet and the diaphragm, where GER typically causes the most severe damage. Strictures cranial to the thoracic inlet are often secondary to foreign objects, but severe reflux can cause acid-induced injuries in this region, and even up to and including the nasopharynx and choana. Magnitude of clinical signs depends on the severity, depth, and extensiveness of esophageal inflammation and the presence and degree of strictures. Animals with esophagitis may regurgitate or be hyporexic (ostensibly because of esophageal pain). More severe inflammation may cause anorexia. Blood seldom is present in regurgitated material. An ingested caustic agent may cause concurrent lingual and oral burns. Although regurgitation is expected in patients with esophagitis, persistent vomiting can cause esophagitis, and signs of esophagitis in patients already vomiting easily may be missed. In critically ill and mentally impaired patients, signs suggestive of esophagitis (i.e., anorexia, regurgitation) may be overshadowed or ignored because of generalized depression or other signs. In people, it is important to look for esophagitis aggressively in such patients because they tend to have a worse prognosis if untreated (Cardin et al, 2007). Signs of esophagitis secondary to anesthesia-associated GER often begin 1 to 3 days and occasionally up to 2 weeks after the causative anesthetic event (Wilson and Walshaw, 2004). Esophagitis may produce immediate (caused by inflammation) or delayed (caused by stricture) signs. Animals with profuse vomiting may begin to regurgitate concurrently. Regurgitation in animals that were vomiting previously is consistent with esophagitis developing secondary to vomiting and persistent exposure of esophageal mucosa to excessive gastric acid. Animals with previously asymptomatic esophageal hypomotility that vomit can retain substantial amounts of gastric acid in the dysfunctional esophagus. They subsequently may start regurgitating because of resulting esophagitis. Esophagitis or esophageal stricture may be suspected based upon history (as described previously) or clinical circumstances. Survey thoracic radiographs are seldom diagnostic; esophageal dilation is often minimal or absent. Mediastinal or pleural air or fluid may indicate perforation. Contrast radiographs typically can diagnose strictures (if done correctly, see later) but are unreliable in detecting inflammation. If perforation seems likely (e.g., pneumothorax or septic pleural effusion), contrast films seldom are needed. If perforation is suspected and the clinician needs to do a contrast study, an iodinated contrast agent should be used instead of barium. Otherwise barium often provides a more definitive study. Esophagitis is suggested by a roughened esophageal mucosa as seen by irregular retention of barium on the mucosa. Liquid barium may pass quickly through a partial stricture, making it easy to miss the obstruction even when using fluoroscopy. Nonetheless, dilute liquid barium should be administered first because it may be diagnostic, and aspiration of small amounts of liquid barium typically produces minimal to no morbidity. If no lesions are detected using dilute liquid barium, barium mixed with canned food (this should be a relatively solid consistency) should be used next (Web Figure 49-1). Fluoroscopy may be needed because it may reveal partial obstructions not seen with static images (i.e., a bolus may “squeeze” through a partial stricture in the period between the bolus being eaten and the radiograph being obtained). Barium paste offers no substantive advantage and is not recommended. Web Figure 49-1 A, A barium contrast esophagram performed using liquid barium. It is not clear that a stricture is present. B, A barium contrast esophagram performed following A, in which barium was mixed with food. It is now obvious that a stricture is present. Endoscopy is the most sensitive and specific way to detect esophagitis. Erythema, friability, bleeding, erosions, and exudative pseudomembranes usually are obvious (Web Figure 49-2). The esophageal mucosa just aborad to the cricopharyngeal sphincter normally is a little rougher than the rest of the esophagus. People may have esophagitis that can be diagnosed only histopathologically, but such cases have not been well documented in dogs and cats. Nonneoplastic canine esophageal mucosa is difficult to biopsy adequately with flexible endoscopic biopsy forceps. Rigid forceps or a biopsy capsule is often necessary to obtain an adequate biopsy specimen of canine esophageal mucosa that is not obviously diseased. Distal feline esophageal mucosa is easier to sample with flexible forceps. Histopathology is required to diagnose eosinophilic esophagitis. Web Figure 49-2 An endoscopic image of an esophagus that has hyperemia and mucosal irregularity resulting from esophagitis.
Esophagitis
Pathophysiology
Clinical Signs
Diagnosis
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


