CHAPTER 2 Birth and the First 24 Hours
Parturition
To avoid a multitude of complications and to best prepare for the event, it is very important to accurately predict when the parturition will occur. There are many different ways to make this prediction, and some ways are more accurate than others (Box 2-1).
BOX 2-1 Methods for predicting delivery date
Natural Birth
Cesarean Section
Neonatal Resuscitation after Cesarean Section
Resuscitation of neonates delivered by C-section involves mostly the same process as outlined in the section on natural birth, except that many puppies will need resuscitation simultaneously as opposed to a more evenly distributed and extended timeframe. Additionally, the fetuses that were in distress before the C-section began should be given priority and may require more extreme measures to resuscitate (see next section on more extensive resuscitation measures).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


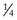 -inch away from the body wall, then tied off with a piece of suture, and finally dabbed with either a chlorhexidine or Betadine solution. Once the neonate is dry and breathing well, it can be put with the dam/queen. A healthy neonate should actively search for the dam’s teat and should start suckling almost immediately.
-inch away from the body wall, then tied off with a piece of suture, and finally dabbed with either a chlorhexidine or Betadine solution. Once the neonate is dry and breathing well, it can be put with the dam/queen. A healthy neonate should actively search for the dam’s teat and should start suckling almost immediately.